As several cadets streamed into the cavernous, darkly lit second floor of Cullum Hall, the task at hand is anxiously simple for them — get swabbed for COVID-19. To fight complacency in a bubble environment, the U.S. Military Academy has continued its rigorous COVID-19 strategy from the summer with the proactive approach of executing surveillance testing on a weekly basis during the academic year.
Currently, as the testing strategy stands, the U.S. Military Academy and the U.S. Military Academy Preparatory School tests 2.5% of cadets, about 115 total, randomly per week. About 1% of the USMA population to include DOD civilians, staff and faculty and 10% of clinical health personnel are tested every two weeks. About 100-150 Corps Squad athletes are also tested per week according to NCAA guidelines. Cadet athletes are required to do 100% testing within 72 hours of competition.
With the testing strategy in mind, Col. Laura Dawson, USMA medical officer, attests that the living conditions in Central Area is easily susceptible to have a communal spread of any virus or bacteria like Strep Throat among cadets. The importance of a continual testing program for COVID-19 is vital to keeping it to a minimal inconvenience on post rather than a debilitating outbreak, which could bring operations at West Point to a screeching halt, Dawson added.
“Putting a surveillance testing plan in place, and when developed appropriately for our community, it potentially allows us to identify an outbreak before there is significant growth,” Dawson said. “Ultimately, that is what you want from your surveillance program — you want to identify asymptomatic positives who could unknowingly spread the virus to those around them. After identifying a positive (result), now you want to direct efforts to determine if there is disease growth around the positive result.”
Laying the groundwork for the surveillance program began in late April as COVID-19 was exploding in numbers in the United States and the cadets were told to stay home in the latter part of the spring semester.
The impetus of the surveillance testing plan, Dawson explained, was to identify and ideally suppress growth of the virus in the barracks while also testing within the community since the DOD civilian and military staff have daily contact with the cadets. Leading the development of a surveillance program that would address some of the unique features of the West Point community, members of the Department of Systems Engineering and the Math Department — Cols. Paul Evangelista and Matt Dabkowski and Lt. Col. Nick Clark — started working multiple modeling concepts aimed at determining the optimal program for COVID-19 surveillance testing at West Point.
“In April, as the academy was working toward graduation, we started talking about what would be next; how do we prepare for the summer and the academic year,” Dawson said. “And what would be a sustainable way of protecting our community in the COVID-19 environment. Unfortunately, with the novel nature of COVID-19, data and research on how to best conduct surveillance testing is not available.”
Dawson said there were concerns about what was the right percentage of random testing needed for it to be effective. Was it 5%, 10% or 40%? By late June, the Department of Defense released a Force Health Protection supplement providing guidance on randomization values for surveillance for different categories of individuals dependent on the mission, location and status.
“When (Evangelista, Dabkowski and Clark) ran their models with various levels of randomization, their simulations indicated upwards of 30-40% of the barracks population would need to be tested weekly to detect and prevent a potential outbreak,” Dawson said. “With how much test costs, the number of tests needed, manpower requirements and the impact to the cadets in order to test 30 to 40% of the Corps every week, it would be difficult to sustain.”
After several weeks and running more than 1,000 simulations, the Math Modelers presented an adaptive model that works synergistically with the randomization program provided in the DOD’s FHP supplement.
“They demonstrated by randomly testing 2.5% of the cadets every week and then adaptively testing those cadets who met a certain level of interaction with a cadet who tested positive, the potential to identify a brewing outbreak significantly increased,” Dawson said.
The PCR Test
The cadets began to settle into Cullum Hall. First, they checked in with a member of the Keller Army Community Hospital team who welcomed them by confirming their ID, setting them up with a label and moving them forward to the testing area. The testing is performed by four separate teams — the Dean’s Office, U.S. Corps of Cadets staff members, Army Cyber Institute/DENTAC/Veterinarian’s Office and the Office of the Directorate of Intercollegiate Athletics.
Dawson watches over the staff during the testing process as the staff initially received training through Keller Hospital from two-to-four hours’ worth of training, depending on what their background was prior to the training.
“They train on how to safely and properly don and take off the (personal protective equipment), proper technique for testing (swabbing) and how to place the specimen in the vial prior to handing it to the lab technician.” Dawson said. “Another important part of their training includes completing HIPAA training along with meticulous review of the patient’s identifiers that are printed and placed on the vial.”
The test used to determine COVID-19 is called the real-time reverse transcription polymerase chain reaction (rRT-PCR) test, or PCR test for short.
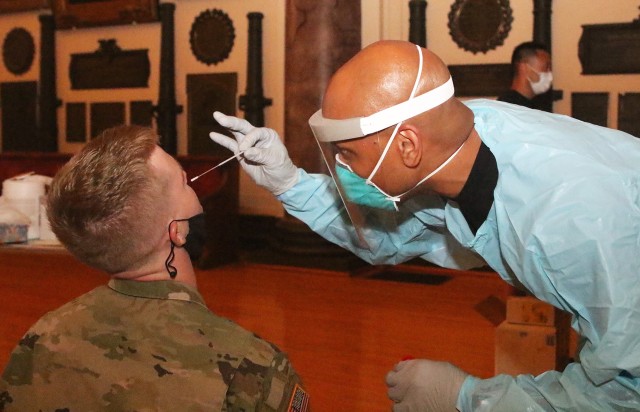
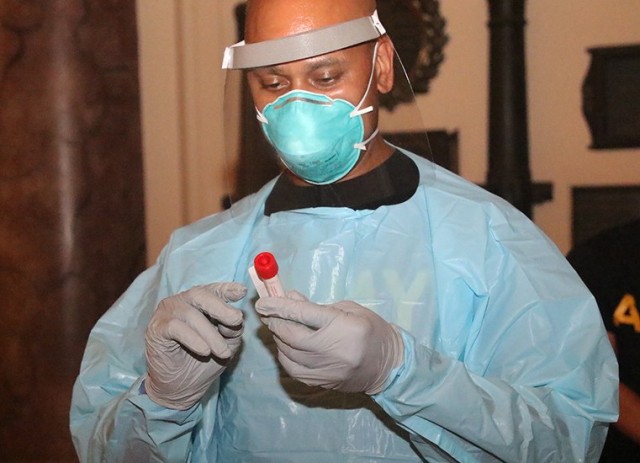
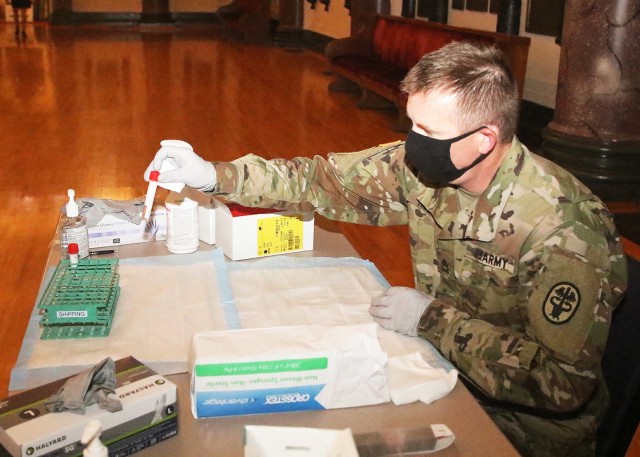
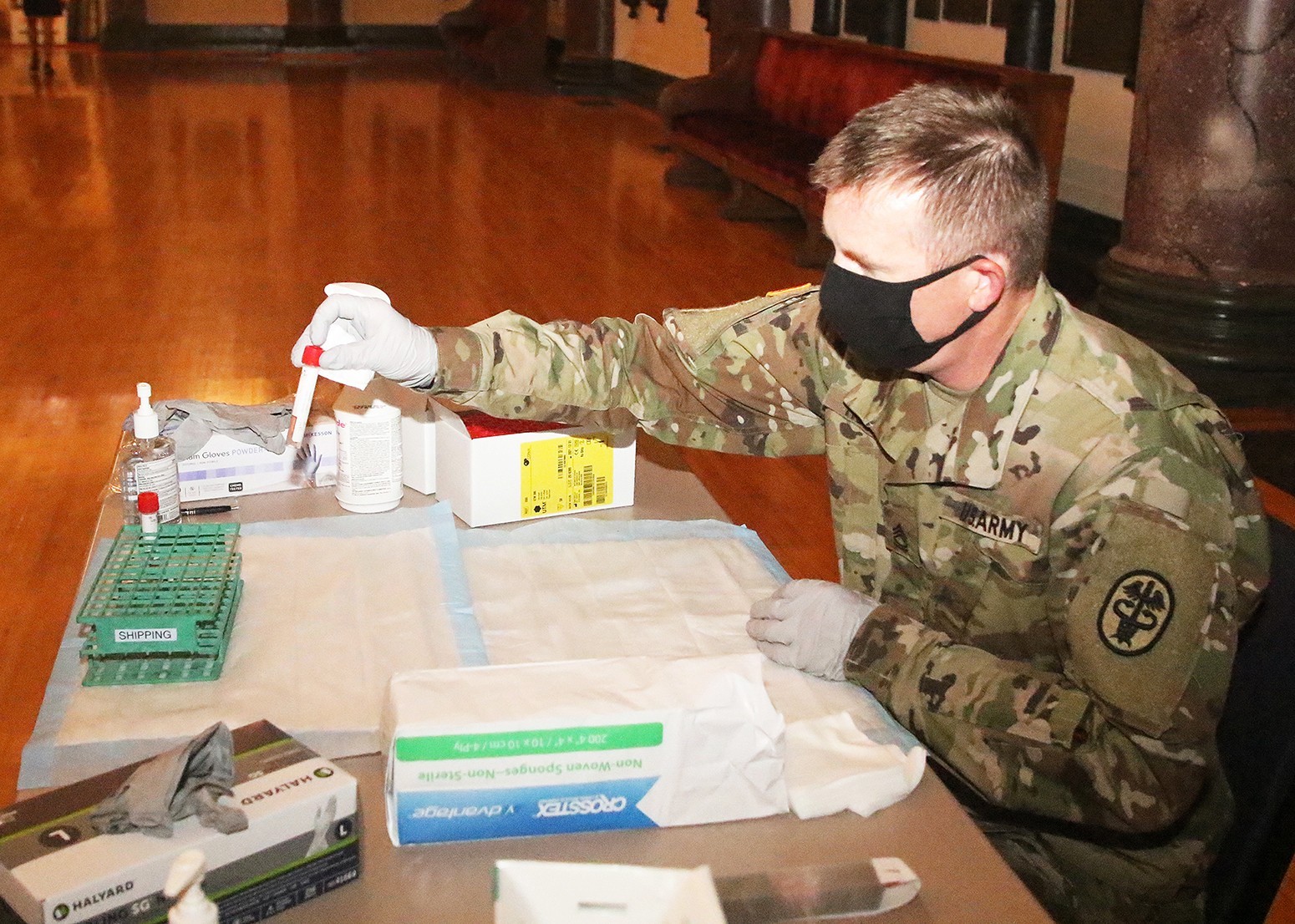
As Dawson describes, the PCR test begins with a long swab that is placed up the nose of the patient, gently “swabs” the tissue in the back of the cavity, then the swab is placed into a viral transport media (test tube) which protects the contents, then the specimen is transported to the lab at KACH. Specially-trained lab technicians then prepare the specimen under a safety hood before placing it into the GeneXpert analyzer.
Once the specimen is prepared and scanned, it is placed in the analyzer. Once in the GeneXpert, it takes about 50 minutes for the analyzer to provide a test result. The GeneXpert and PCR platforms look for a piece of RNA and, if found, amplifies the strand so that the analyzer can determine if the specimen is positive or negative.
If someone tests PCR positive, most likely the person will be directed to complete 10 days of isolation. For cadets that test positive, they will stay in Building 624, or a similar building, for their 10 days. Once they have completed their 10 days and are without any medical symptoms, they can be cleared by a provider and released to return to duty.
Part of the learning curve with COVID-19 is that viral fragments, Dawson said, can stay in a person’s body for 30 to 90 days, and for some people, maybe longer which has prompted the Centers for Disease Control and Prevention, along with other agencies, to move away from testing out of isolation after an initial positive COVID-19 test result. Emerging products may allow the academy testers to test for the active portion of the virus with saliva or a small drop of blood in the near future, but Dawson said while the PCR test isn’t a perfect test, it is the best platform they have to detect the virus at this time.
Kudos to everyone supporting the mission
Dawson speaks highly of the many individuals who have performed well under challenging circumstances while dealing and fighting COVID-19 within the community.
Keller Hospital’s laboratory, which is run by Capt. Jeff Baker, supports surveillance testing, normal hospital testing and handles the order and procurement of testing supplies, and has done an impeccable job, Dawson said. If a person tests positive, Baker also validates the results prior to releasing the results.
Once asymptomatic persons are identified as having a positive COVID-19 result from surveillance testing, they are informed of their results by a medical provider. They are then asked to complete an initial trace form and provide that to the USMA Trace Team.
“The USMA Trace Team works with Army Public Health to provide initial recommendations which could include having some people stay in their rooms/home until the Trace Team can complete all the required interviews,” Dawson said. “For a cadet who tested positive for COVID-19, they will most likely be required to complete 10 days of isolation in Building 624, which through the hard work of Team COVID (Majs. Jay Brend and Bryan Ralls) is equipped with desks, lamps and WiFi to help the cadets stay on track with their academic requirements.”
Since March, as the USMA medical officer, Dawson has assisted the USMA staff with medical plans and operations in the COVID-19 environment.
“A lot of what we do includes helping our community leaders and supervisors navigate questions and concerns about safely operating in our current environment,” Dawson said. “Putting the USMA Longitudinal Testing Program (LTP) together was a complete team effort with USMA staff, the Department of Systems Engineering/Math (Evangelista, Dabkowski and Clark) and KACH all working together for several months to make this happen.
“Col. Alicia Madore and her team at Keller set up and provided the hours of required medical training to support the LTP,” she added. “Capt. Baker and his crew worked around the clock to support surveillance testing along with supporting all the lab requirements of a 24/7 ER and hospital. Maj. Will Pitt and his crew set up, tested, transported specimens, tracked those tested and broke down and cleaned up after each testing event (during Cadet Summer Training and at Cullum Hall currently).
“Maj. Marion Keehan, the brigade surgeon, and Maj. Chris Barber are providers who worked directly with the cadets to safely bring them back to West Point and they continue to work with them through sick call and clinic appointments to evaluate, treat and monitor their health,” she concluded.
Dawson gave the KACH staff high marks for its “mental and physical” gymnastics through the last few months of up-tempo work. However, the work will not go away in the foreseeable future as Dawson suspects that COVID-19 testing will most likely continue through academic year 2020-21.
But as KACH and several folks continue to work hard to keep the community safe, the community can still do its part by sticking to things that can keep them healthy such as the use of nonpharmaceutical interventions, or NPI.
“Looking around the country, we see COVID-19 continues to create challenges,” Dawson said. “Consistently using NPI, our community and surrounding partners are currently enjoying low COVID-19 disease prevalence and low positive testing rates. (Superintendent) Lt. Gen. (Darryl A.) Williams mentioned we have to earn this every day, and to do this we need to keep using NPI and fight complacency.”
Outside of four years working in medical school, Dawson has spent 26 years in the Army in quartermasters, aviation and the medical field, including being the deputy commander at Keller Hospital prior to her current post. However, in all that time she served, these last few months, Dawson said, “were definitely the most unpredictable, unique and trying experience.”
However, Dawson concluded, “But, at the same time, watching the West Point community come together to support the USMA Class of 2020 graduation, the execution of Cadet Summer Training, bringing the entire Corps of Cadets back to West Point and now watching these young men and women handle the adversity and overwhelmingly comply with NPI even though they know they are not the population at high risk for serious complications associated with a COVID-19 infection, it reinforces why USMA leads our Army, military and our country in any situation.”






Social Sharing