HONOLULU --Tripler Army Medical Center started receiving low-level trauma Department of Defense beneficiary patients, Jan. 25.
Tripler, who treated 307 patients last year who were qualified to be trauma patients, was approached by the State of Hawaii to enter into their integrated trauma system.
"The driving force behind Tripler's participation is their commitment to patient care," said Navy Capt. Kenneth Kelly, chief of the Emergency Department, TAMC.
According to Lt. Col. Kurt Edwards, chief of Trauma/Surgical Critical Care, TAMC, up until recently, Tripler did not have a systematic way of assessing trauma patients.
Tripler does not have unused capacity to make additional treatment possible, but they do have unused skill.
"We have a certain amount of expertise and if you were really to look on (Army Medicine), Tricare, and Military Health System mission statements, their missions are to provide care and promote health of the military person," Edwards said. "One of the biggest things that kills and injures our Soldiers is trauma."
When entering the state's trauma system, Tripler will become part of their Trauma Registry and be able to share trauma data.
"As a part of the Trauma Registry we will share data and outcomes to improve the overall trauma system in Hawaii," said Brig. Gen. Keith Gallagher, commanding general, Pacific Regional Medical Command and TAMC. "We are honored to be part of this system and to help improve the trauma system and to share our experiences and insights gathered from multiple combat tours of our providers and nurses."
A hospital's capability to care for trauma within the state is currently based on four level systems with Level IV being the lowest capability and Level I being the highest.
"A State of Hawaii Level III trauma center does not require instant presence of a trauma surgeon, anesthesiologist, or operating theater personnel," Edwards explained. "There are no requirements to have a sub-specialty, surgical services, other than orthopedics, available.
"The most likely reason to bypass a Level III facility and proceed to a Level II would be a person sustaining an injury severe enough to cause them to not be normally responsive," Edwards added.
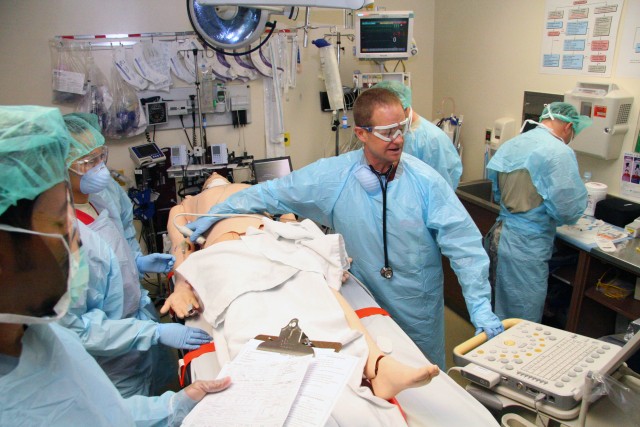
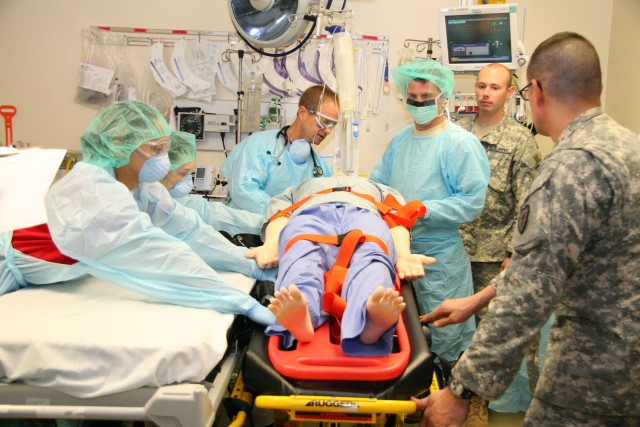
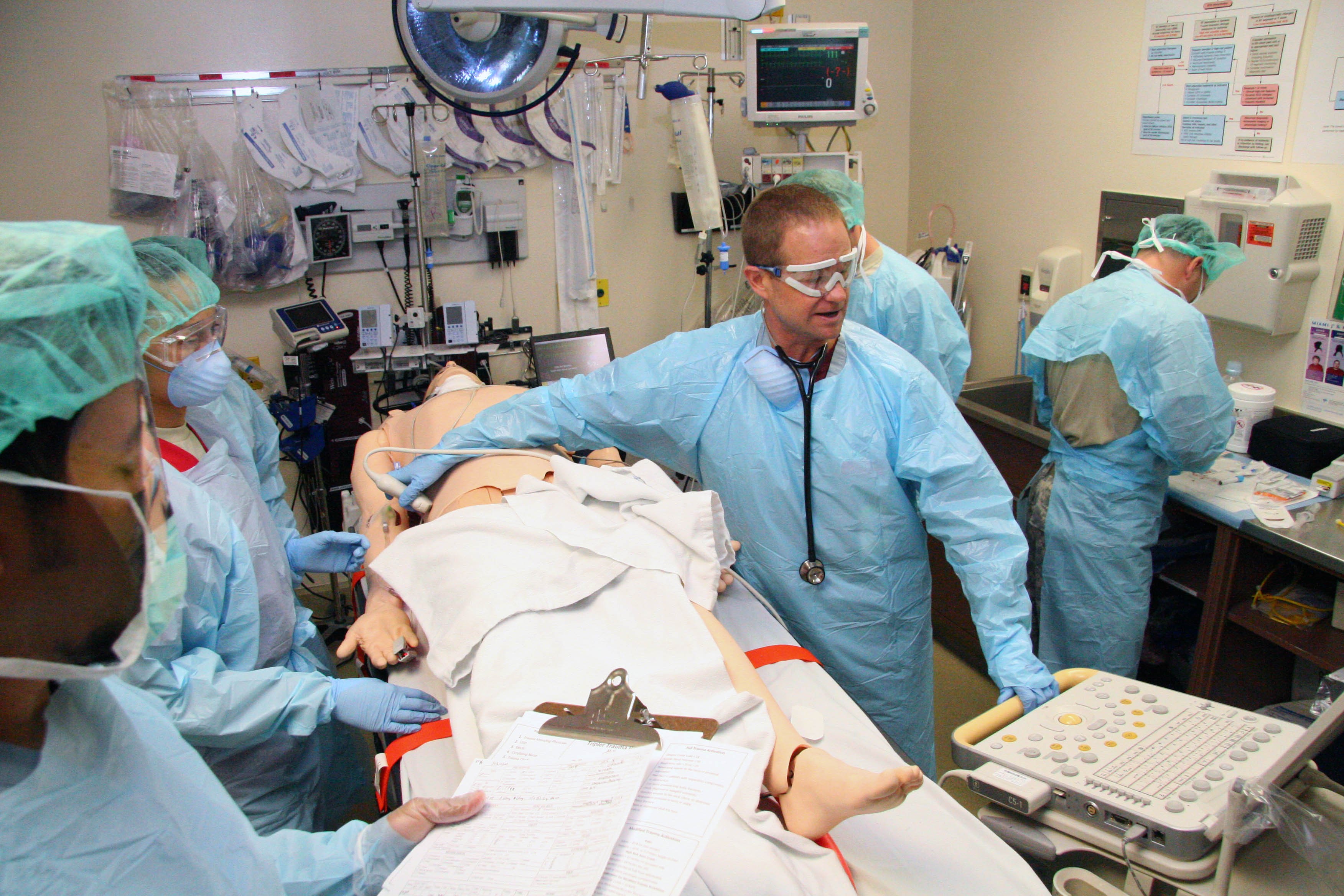
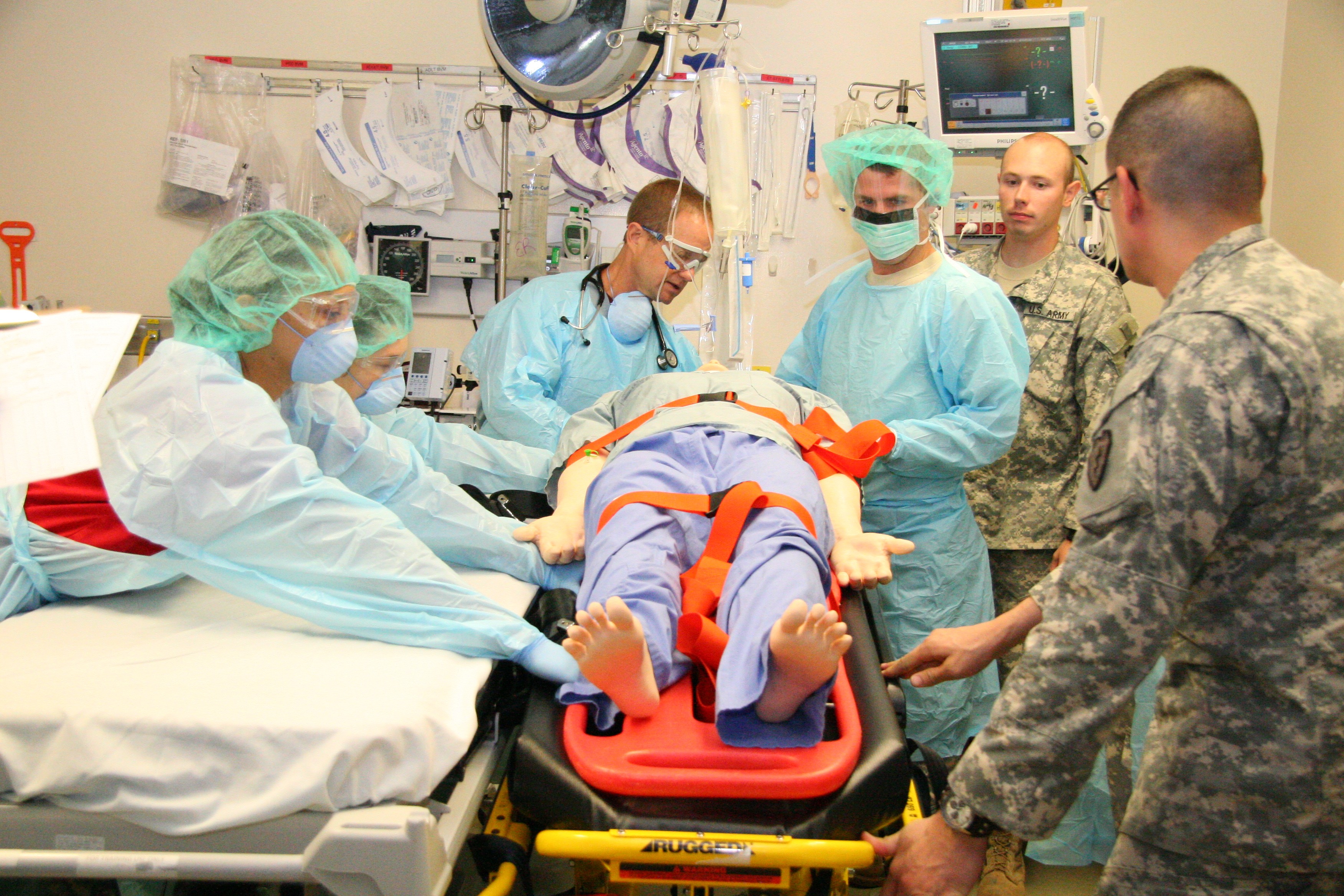
Tripler, just like any other military organization, has prepared for their new trauma duties by training. Prior to Jan. 25, they held multiple trauma assessment simulations using their simulation center's SimMan 3G patient simulator.
Edwards said they learned two valuable lessons from the mock activations; the physicians must be trained to answer the radio calls from Emergency Medical Services and TAMC needed to create a system of group paging to notify trauma teams when a trauma patient is en route.
Edwards said when it comes to trauma activations, everyone involved, no matter what the level, all play a vital role.
Prior to activating the trauma team, the physician must take the radio call from the EMS first responders. Edwards said this is important because it helps determine the facility the patient will actually be transported to.
As TAMC settles into its new role, the next step for the hospital is to expand their trauma personnel by hiring two additional trauma surgeons.
This is not a requirement to join Hawaii's trauma system, but Tripler's command wants to ensure they can provide excellent coverage for the hospital and its patrons prior to accepting civilian patients, explained Edwards.
Since Jan. 25, Tripler's trauma program has responded to seven trauma activations.
"(Our goal is to ensure) that trauma care is better today than it was yesterday," Edwards said.
Social Sharing