WIESBADEN, Germany (Feb. 28, 2014) -- Blurry vision, dizziness, mood swings, sleep problems and memory problems: these are all symptoms of traumatic brain injuries, or TBIs, and can last from a few days to a lifetime, depending on the treatment and severity.
March is Brain Injury Awareness Month. A brain injury can happen anytime, anywhere, to anyone. Brain injuries do not discriminate. Approximately 2.4 million people sustain brain injuries in the United States each year. An injury that happens in an instant can bring a lifetime of physical, cognitive, and behavioral challenges.
"It's a multi-system dysfunction that also affects the family," said Col. Debra McNamara, optometrist and TBI specialist at the Wiesbaden Army Health Clinic. "The quicker you get treatment, the quicker Soldiers and their families rehabilitate."
A brain injury can affect a person physically and psychologically, and sometimes the symptoms-like memory problems or emotional and behavioral changes - don't appear immediately. Everyone in the family is affected by TBI and changes in relationships, behavior, finances and social life can add stress to family life.
For example, if a child isn't sleeping well, he or she will be sleepy in school and grades might slip, causing stress for the child and his or her parents. Early and adequate access to care will greatly increase overall quality of life for the patient as well as the family members, who play an important role in the care and rehabilitation of individuals with TBIs.
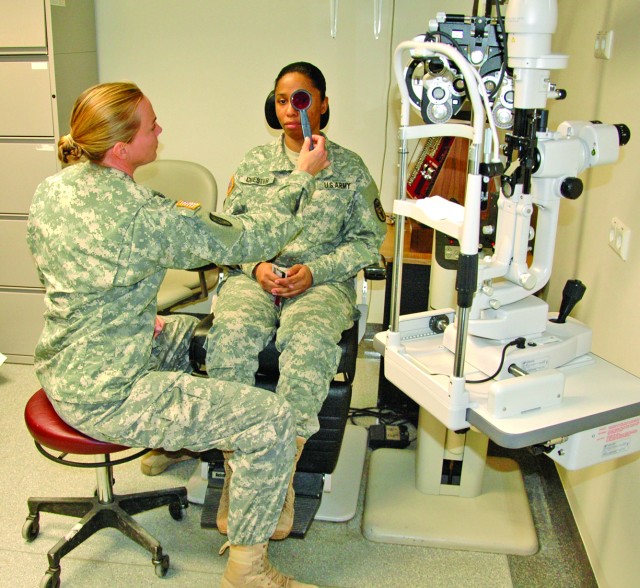
Vision therapy is an integral part of treatment for post trauma vision syndrome, a problem of up to 75 percent of people with a TBI experience. Brain swelling can disrupt ocular motor nerves in the brain, preventing eyes from moving in the same direction at the same time.
When this happens, patients will often tilt their head to avoid seeing double, sending poor information to the vestibular system. The result is poor balance, dizziness and headaches.
Post trauma vision syndrome is often overlooked. Until the vision problems are treated, patients may find reading, computer work, driving and shooting difficult. They might see perfectly with one eye, but not so well with both.
"People will tell me, 'I thought I was crazy -- I didn't know how to explain something was wrong with my vision,'" recounted McNamara.
Most of the time, the problem can be fixed with a pair of glasses, prism and/or vision training. Some of the near-focusing problems resolve after systemic medications are discontinued. Headaches also will disappear.
"Alleviating vision problems significantly improves quality of life, so optometry is a rewarding role to play in TBI rehabilitation," she said.
Other common problems associated with mild TBI include changes in sleep, mood, energy, behavioral and cognitive patterns.
During the height of combat, the numbers of service members who experienced a TBI increased by approximately 10,000 per quarter and the majority of these (80 to 85 percent) have been classified as mild TBI, or mTBI. Although most patients with mTBI recover completely within three months of injury, some patients experience persistent symptoms and have trouble rehabilitating, particularly when they have co-occurring conditions, like Post-Traumatic Stress Disorder -- or suffer another TBI soon after.
As the war winds down, most new TBIs result from fights and ski, bicycle, and other sports accidents.
"If you take a fall and hit your head while snowboarding and end up with a headache, the worst thing you can do is get back on the board and risk taking another fall on the slopes," said McNamara.
Brains need darkness and rest. In Afghanistan, she said, TBI patients would rest in "TBI tents" for up to 72 hours to let their brains heal.
The Defense Centers of Excellence for Psychological Health and Traumatic Brain Injury Information & Referral hotline (1-866-966-1020) is staffed 24 hours/day, every day of the year, as is the Crisis Intervention line (1-800-273-8255). Visit the Defense and Veterans Brain Injury Center (DVBIC) online at dvbic.dcoe.mil or brainlinemilitary.org for more information.
--------
Ten facts to keep in mind about Traumatic Brain Injury:
-2.4 million people suffer a TBI in the U.S. every year.
-Blasts are a leading cause of TBIs in a warzone. Otherwise, falls account for 35 percent of TBIs; motor vehicle crashes, 17 percent.
-TBI is a contributing factor to a third of all injury-related deaths in the U.S.
-TBIs can increase the risk for epilepsy, Alzheimer's disease and Parkinson's disease.
-Males are about 1.5 times as likely as females to sustain a TBI.
-Children aged 0 to 4 years, teens aged 15 to 19 years, and adults aged 65 years and older
are most likely to sustain a TBI.
-Having a concussion increases the risk of having another, and those with multiple concussions take longer to recover.
-Kids who suffer a concussion may have a much slower recovery if they've sustained one or more blows to the head in the past, according to studies.
-Studies have also shown that kids who have the most mental activity after a concussion took the longest time to fully recover -- an average of 100 days.
-Bicycling, football, playground activities, basketball, and soccer are associated with the greatest number of TBI-related emergency room visits.
(Information courtesy of the Brain Injury Association of America and www.webmd.com)
Related Links:
Defense and Veterans Brain Injury Center
STAND-TO!:Traumatic Brain Injury
Army.mil: Traumatic Brain Injury
Injury Prevention & Control: Traumatic Brain Injury
U.S. Army Medical Research and Materiel Command: Combat Casualty Care Research Program

Social Sharing