JOINT BASE SAN ANTONIO-FORT SAM HOUSTON, Texas (March 15, 2022) -- Brooke Army Medical Center reopened its Pediatric Intensive Care Unit March 1 after a two-year hiatus.
The PICU mission was temporarily paused due to the COVID-19 pandemic and to conserve resources and personnel.
“Our first step is the opening of two pediatric intensive care beds on our pediatric ward staffed by pediatric critical care nurses,” said Army Col. (Dr.) Matthew Borgman, pediatric intensivist. “As we get more trained nurses,” the aim is to expand into a stand-alone PICU in the future, he added.
“Having a higher level of care available to our younger beneficiaries allows us to expand the type of capabilities, surgeries, and procedures to children and adolescents of all ages,” said Air Force Lt. Col. (Dr.) Renee Matos, pediatric critical care physician.
“This also allows us to better coordinate care for our patients with complex medical needs who are intentionally stationed here through the Exceptional Family Member Program,” Matos said. “Many of our patients have close relationships with their (Joint Base San Antonio) pediatric subspecialty team, and now they will be able to be a part of their care should they need to be admitted to the PICU.”
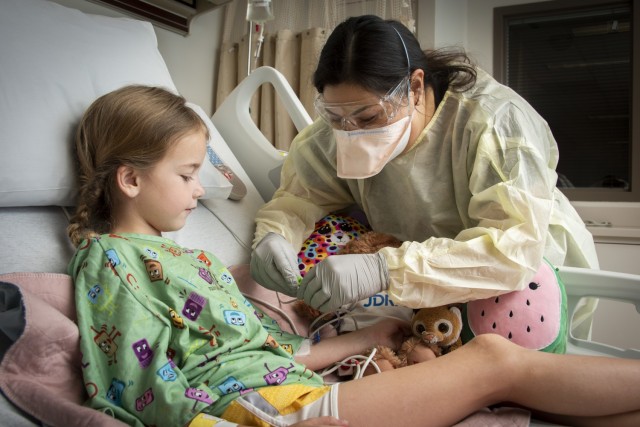
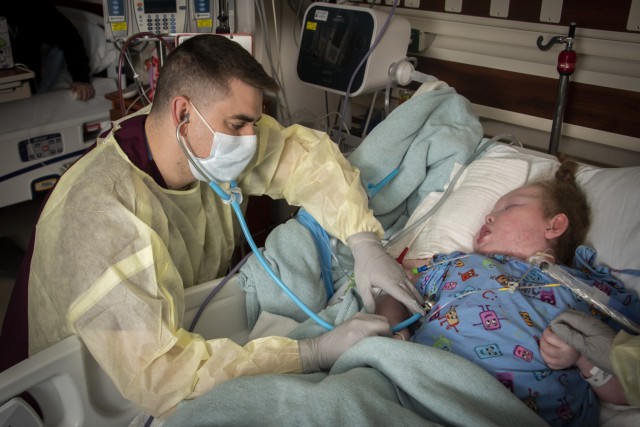
Courtney Moses’ daughter, Kaileigh, was admitted to the PICU March 8, after a visit to the Emergency Department for possible sepsis.
“Kaileigh was actually born at BAMC at 24 weeks, and was in Neonatal ICU for quite a while,” Moses said.
The 10-year-old has epilepsy and hydrocephalus, a build-up of fluid in the cavities deep within the brain. She also has a tracheostomy, is on a ventilator and has a feeding tube, Moses explained.
Moses feels continuity of care is important because of her daughter’s ongoing medical concerns.
“She sees all her subspecialty doctors at BAMC,” Moses said. “So being here definitely makes it easier for her providers to keep up to speed on her status and where she is at with the management of her healthcare while she is in the ICU.
“We feel like the nurses and doctors here are like another family to us,” she said. “They know her history from the very beginning and they know us so well. It just makes it easier knowing that she’s going to get amazing, above-the-notch care at BAMC.”
Melinda Moore agrees. Her 7-year-old daughter Margaret was the first patient admitted to the new PICU after being diagnosed with Type 1 diabetes.
“The care has been phenomenal, everything from being down in the ER to the transition up here (to the PICU),” Moore said. “Everyone has been courteous and really helpful with making sure she is comfortable with what’s happening and that we have the information we need.”
Reopening the PICU also benefits the graduate medical education residents and fellows across multiple departments because they are able to expand their experience and exposure to children with complicated health cases, which increases their readiness capability.
“The ability to care for critically ill children provides experience and exposure to our entire medical care team, including nurses, techs, respiratory technicians, and others who also benefit from increased readiness,” Matos said.
“More importantly, having these ICU capabilities allows our pediatric patients who are at their sickest to remain with their own doctors and care team rather than being transported to a new facility with new providers,” she added.




Social Sharing