
ABERDEEN PROVING GROUND, Md. – “Unprecedented.” That was the buzz word of the day heard around the world in March 2020, when life as society knew it came to a halt to adjust to the COVID-19 pandemic, which had recently been declared a public health emergency by the World Health Organization.
This emerging virus, which had its first reported cases in China, was spreading like wildfire across the world’s seven continents, and public health officials were scrambling to give guidance on how to prevent severe illness and death from the highly contagious disease.
For the first time in modern history, mask mandates were issued for virtually every human being, people were advised to practice “social distancing,” and stay six feet away from other persons they encountered; businesses were shut down (except for those that performed essential services); and people were mandated by government officials to not attend gatherings with more than 10 people.
“For some individuals, it felt like the world was ending. This pandemic had undoubtedly changed our way of life,” said John Resta, who served as the director of the Army Public Health Center, a predecessor organization to the Defense Centers for Public Health-Aberdeen.
Resta recalled the daily meetings with Department of Defense senior leadership on how to protect the DOD workforce. Although DOD public health experts had been called upon to respond to other public health emergencies, the situation faced in March 2020 was like no other.
He knew that responding to this unprecedented event was the “Superbowl” of public health. The stakes were high. Resta had confidence in his team, which was quickly shared by Army leadership.
“On March 15, 2020, I attended a teleconference meeting of Army Senior Leaders where we were briefed by various agencies and staff offices on the anticipated scope of the pandemic, it's potential impact on the nation and the Army,” said Resta. “The meeting started at about 9 a.m. on a Sunday morning and lasted until about 2 p.m. when we were tasked with a long list of questions to answer.”
With the help of Dr. Steven Cersovsky, then APHC’s senior scientist and now the DCPH-A deputy director, they submitted their first response to the Army Office of The Surgeon General that evening a little after 9 p.m.
“They were a little shocked, but this gave them the confidence that we could do this,” said Resta. “That attitude lasted for the remainder of my career, and I suspect is retained today by DOD Senior Leaders.”
It was a long journey, but eventually, the COVID-19 nightmare began to subside, and three years later, public health officials can now see life returning to a bit of normalcy as the COVID-19 public health emergency comes to an end May 11 in the United States. But the lessons learned will be ones that stick with DOD health professionals for life.
COVID-19 TASK FORCE
In the spring of 2020, when the COVID-19 virus was spreading rapidly, there were hundreds of requests for assistance coming from DOD agencies on how to prevent or mitigate the virus.
It became clear that the Army needed a central clearing house for these queries.
Thus, the APHC established the COVID-19 Task Force which served as the nucleus driving the Army Public Health pandemic response by providing project management and coordination across the Army and Department of Defense. This team ensured information and products were comprehensive, consistent, delivered in a timely manner and followed best-available public health guidance from the CDC.

Over the course of the pandemic, the COVID-19 Task Force responded to more than 2,800 requests for information and assistance to disease epidemiology and surveillance, environmental, laboratory, operations, communication, and occupational health topics from more than 225 organizations worldwide. Additionally, the Task Force:
- Completed 1,400 information products
- Contributed to the production of more than 20 webpages
- Developed more than 110 digital and print information products
- Produced 399 COVID-19 social media products
- Produced 23 informational news articles
These products were published more than 2,500 times and reached more than 15 million users. Finally, the Task Force was also instrumental in completing more than 350 Health Risk Assessments for DOD level events. They were recognized twice by Army senior leaders for their efforts to save lives.
“These diverse professionals on the task force were suddenly thrust in a role where they had to understand analytical laboratory processes, infectious disease prevention, virology, immunology, public health communications, knowledge management systems, risk assessment, and epidemiology, among other disciplines all while running at break-neck speeds to complete thousands of requests for information and tasks,” said Steve Starbuck, COVID-19 Task Force Response coordinator.
Dr. Robyn Nadolny, who coordinated the COVID-19 pooled surveillance mission, which was eventually recognized with a military award, shared Starbuck’s sentiments.
“We are stronger together,” said Nadolny. “Only by bringing together personnel, expertise, and connections from across the center and the DOD public health enterprise were we able to stand up an accredited COVID testing laboratory between spring and summer 2020. It took a village, and it took some unshakeable personalities persevering and pressing to do what was right in the face of incredible hurdles. I’m honored to have worked alongside an incredible team supporting our military and civilian communities by providing pooled testing during the worst months of the pandemic, saving key medical supplies so they could be used in clinics where they were needed most, and preventing COVID from spreading among asymptomatic troops.”
REMOTE WORK/TELEWORK
Another challenge that presented itself was how the DOD workforce would adjust to a largely remote working environment to combat the spread of the virus. In the early days, individuals had problems connecting to DOD networks from a remote location, as the existing framework was not prepared for the sharp increase in remote traffic, but as the weeks and months went by, the connections became better. Soon teleworking became the new norm.
Senior leaders say the DOD workforce has proven that the mission can get done, even when personnel work remotely. This newfound success has allowed the DOD and many offices around the world to adapt to a “hybrid” culture that allows employees to have the flexibility of coming in and/or working at home as agreed upon with management.
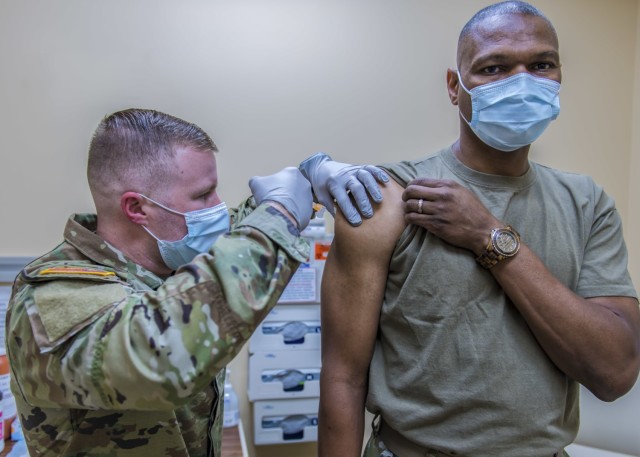
U. S. Army Command Sgt. Maj. Michael Gragg, Senior Enlisted Leader of the Defense Health Agency, prepares to receive his COVID-19 vaccine booster at the Belvoir Hospital Immunization Clinic September 14, 2022.
(Department of Defense photos by Reese Brown) VIEW ORIGINAL
VACCINES
As the months progressed, one of the happiest moments of the COVID-19 pandemic occurred in December 2020, when the first vaccines became available from Pfizer and Moderna. These products, known as “Messenger RNA vaccines” used existing technology to instruct the body to make antibodies to the COVID-19 virus, thereby protecting individuals from COVID infection.
“With vaccines available, there was light at the end of the tunnel,” said Cersovsky. “Taking the vaccine protected our workforce, our communities, and our nation.”
Within DOD, vaccine administration was initially targeted to deploying forces, health care workers and other essential personnel, and those most at risk for severe disease. Within a few months, as larger quantities became available, the vaccine availability expanded to all DOD beneficiaries.
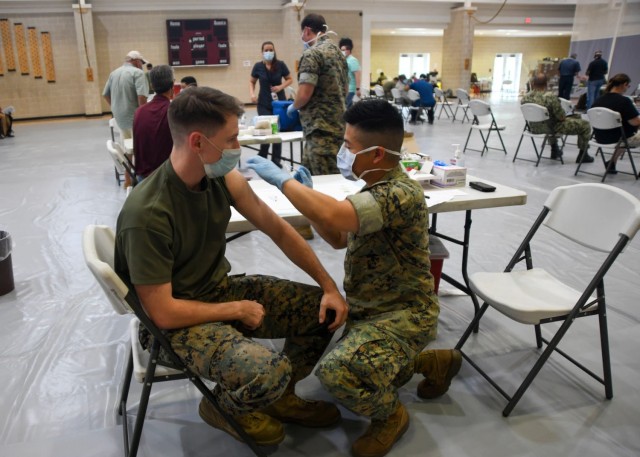
DOD would eventually administer more than 2 million vaccine doses to its beneficiaries.
Eventually, cases of severe illness and death dropped significantly as more people were vaccinated against the virus.
LABORATORY OPERATIONS
As they reflect over the past three years, public health professionals say that one of the most enduring contributions of the DOD public health response was the role of laboratory professionals in combatting the spread of the disease. At the height of the response, these lab officials established the Army Public Health Laboratory Enterprise COVID-19 surveillance concept and capability, which could analyze more than 2,000 samples per week.
Nadolny credits the Laboratory Directorate leadership with setting the example in the early days of the response.
“Having the laboratory leadership (including the lab director and the lab manager) show up to work alongside the analysts on the front lines the first days that we received samples for testing, was inspiring,” said Nadolny. “They were onsite, over the weekend, in PPE, acting as ‘runners’ and supporting the new testing effort in every way they could, including buying lunch for the teams that were working overtime and weekends to get the mission accomplished. That’s leadership! And pizza is a powerful morale booster!”
In April 2023, DCPH-A opened a public health laboratory that will leave them poised for the future, should duty call. The 280,000-square-foot laboratory building is comprised of 67 individual lab spaces that feature mobile casework and are tailorable to future public health missions, including another pandemic response.
POISED FOR THE FUTURE
“As we wind down the public health emergency known as the COVID-19 pandemic, we learned that a joint response to our global public health challenges is the best approach,” said RDML Brandon Taylor, DHA Public Health Director “The work we do in Defense Public Health saves lives by stopping or preventing disease in our DOD community.”
Cersovsky agrees and said he is proud of the role DOD public health played in navigating the uncharted waters of the COVID-19 pandemic.
“We had a great team here at DOD public health that helped us safely reach this milestone—officially ending the COVID-19 public health emergency,” said Cersovsky. “For more than three years, DOD public health experts have been our go-to consultants as we faced a worldwide public health crisis and fought against the COVID-19 pandemic. All of these accomplishments demonstrate Defense Public Health’s commitment to protecting the health of the Force and maintaining the readiness of our DOD beneficiaries.”
Although the COVID public health emergency is ending, and DOD public health professionals reflect on what took place over the course of it, they say the work of public health continues. They remind DOD beneficiaries that COVID has not gone away, and that individuals should still take steps to preserve their overall health and well-being.
“We will have to remain vigilant on what may emerge next,” said Kevin Delaney, chief of public health communications for DCPH-A. “COVID is transitioning and will exist alongside other threats, like influenza, that we must prepare for annually and ensure the necessary steps are taken to protect our forces, our families, and ourselves.”
Delaney said public health professionals remain committed to protecting the health of the force.
“The pandemic highlighted the role of public health, which is often silent; it’s a good thing when people don’t see us,” said Delaney. “While we may be drifting out of the spotlight, the dedication and professionalism of public health professionals, not only in the Department of Defense, but across the nation, and world, will carry on.”
The Defense Health Agency supports our Nation by improving health and building readiness – making extraordinary experiences ordinary and exceptional outcomes routine.
NOTE: The mention of any non-federal entity and/or its products is for informational purposes only, and not to be construed or interpreted, in any manner, as federal endorsement of that non-federal entity or its products.




Social Sharing