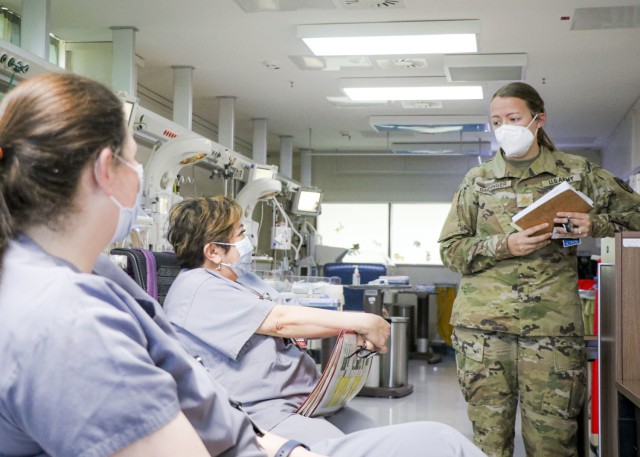
A decade ago, newly minted Army Nurse Corps officer, Rebeccah Dindinger’s future was outlined on a 3-by-3 inch note.
Before tackling ROTC throughout college, Dindinger knew she wanted to make a difference. She thought she could accomplish this not just by becoming a nurse but becoming an Army nurse and take care of Service Members and their families. Following her graduation in 2010, Dindinger found her calling in the Labor and Delivery Ward.
“I thought (being able to serve) was really awesome. We were in the height of war, and I really felt like that was a way I could give back,” said Dindinger, now a major working at Landstuhl Regional Medical Center’s Division of Women’s Health and Newborn Care. “I noticed that the nurse was always in the room a little bit more than the provider was, so (nursing) is what I wanted to do and how I wanted to take care of people.”
After observing the attention to patient care Clinical Nurse Specialists (CNS) demonstrated, Dindinger knew there was more she could do to help patients and the Military Health System.
“I had a great clinical nurse specialist, she was doing lots of education and teaching and keeping us up on the latest research,” says the Lilburn, Georgia native. “Then I went to my next duty station and had another great CNS, doing the same thing.”
Knowing the potential Dindinger demonstrated, the CNS encouraged her to pursuit further education toward advanced practice to better serve patients and staff.
“She sat down and planned out my life on a note, she was my second call after I got into graduate school,” said Dindinger.
Clinical Nurse Specialists are Advanced Practice Registered Nurses (APRNs) who not only provide patient care but specialize in mentoring, educating and progressing clinical practices in specific patient populations.
“Research and evidence-based practice really helps military medicine stay at the forefront of the care we provide. Both help (medical professionals) do the best we can for our patients,” said Dindinger.
History links military medicine to medical advancements, particularly in trauma care. Today, the U.S. Armed Forces have unprecedented survival rates for combat casualties arriving to military treatment facilities, as high as 98 percent. It’s through technology, research and lessons learned that these advancements have been possible. According to Dindinger, these innovations save lives.
Today, Dindinger serves as the CNS for her ward, while still heavily involved with mentoring and assisting novice Service Members interested in the research field.
“It's really rewarding for me, to help grow the bench because I know someday I'm going to retire from the military, it's important to build the people that are coming up in the field,” she said.
A testament of her dedication to research and advancing military medicine was demonstrated recently when Dindinger received honors at the annual TriService Nursing Research Program’s Research and Evidenced-Based Practice Dissemination Course, where she earned the Outstanding Podium Presentation Award for her presentation on Intimate Partner Violence (IPV) during pregnancy, a topic she unfortunately knows too well.
“I'm really passionate about it because I'm a victim of emotional abuse and (IPV) from my first marriage. It really influences maternal child outcomes both during the pregnancy and for the life of the child,” shared Dindinger. “I was an Army officer and no one ever asked me (if she was a victim of IPV) so I hope my experience and research can help make a difference in someone else's life. I got to talk to leaders from across the Department of Defense and hopefully influence them to address this issue and help build our health systems better to address IPV.”
Amusingly, Dindinger’s award-winning presentation during the course was outlined on a 3-by-3 inch note.
“You can give a 15 or 30 minute presentation from a (note). I think we tend to forget that we can do that sometimes,” suggested Dindinger.

Social Sharing