After a tour in Germany, Maj. Elizabeth Holshouser was ready to move back to the U.S. to begin an assignment at Fort Bliss, Texas. A week before her move, her annual mammogram revealed a pair of tumors.
Prior to leaving Germany, Elizabeth and her husband had begun considering treatment options should tests come back positive for breast cancer, a diagnosis neither were anticipating and would alter future plans for Holshouser, who was slated to deploy with a Forward Surgical Team and the 131st Field Hospital. Additionally, the couple were concerned the relocation would limit accessibility to first-class care for her condition.
"When you find out you have cancer, you immediately think of (world renowned cancer centers)," said Kenneth Holshouser, Elizabeth's husband. "You want to make sure you have the best care when it comes to cancer."
As a certified registered nurse anesthetist, returning to Fort Bliss meant an opportunity for Elizabeth to discuss treatment options with familiar medical professionals, as she had previously spent a tour at the Texas base.
"I hand-delivered the (radiology) disc to the general surgery group (at William Beaumont Army Medical Center)," said Elizabeth, who has served in the Army for 25 years. "(The staff) scheduled me an appointment quickly for biopsies, which came back positive."
As part of WBAMC's multidisciplinary approach to treating cancer, several healthcare professionals discussed treatment options with Elizabeth, including reconstructive surgery, if she elects to do so.
"They told me like 50,000 treatment options, we talked about it for hours," said Elizabeth. "They wanted to do the best thing for me."
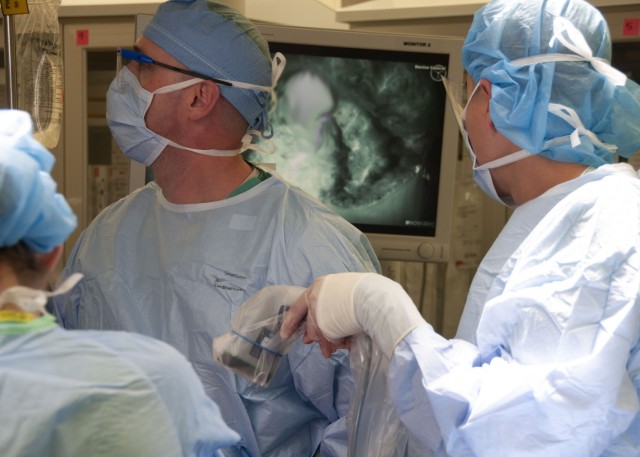
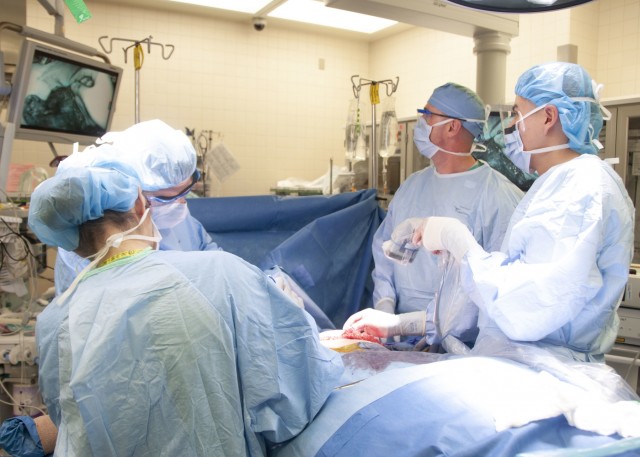
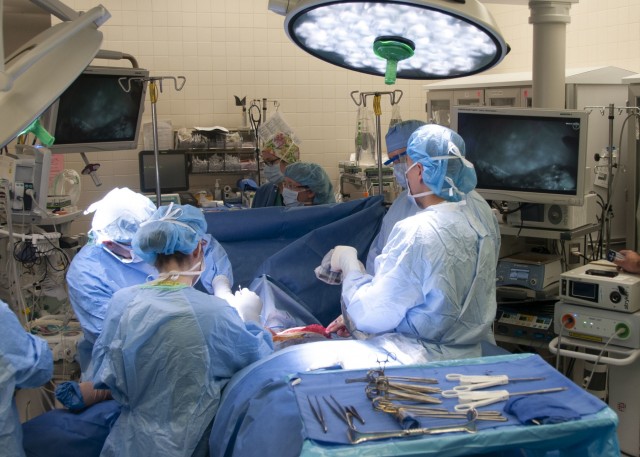
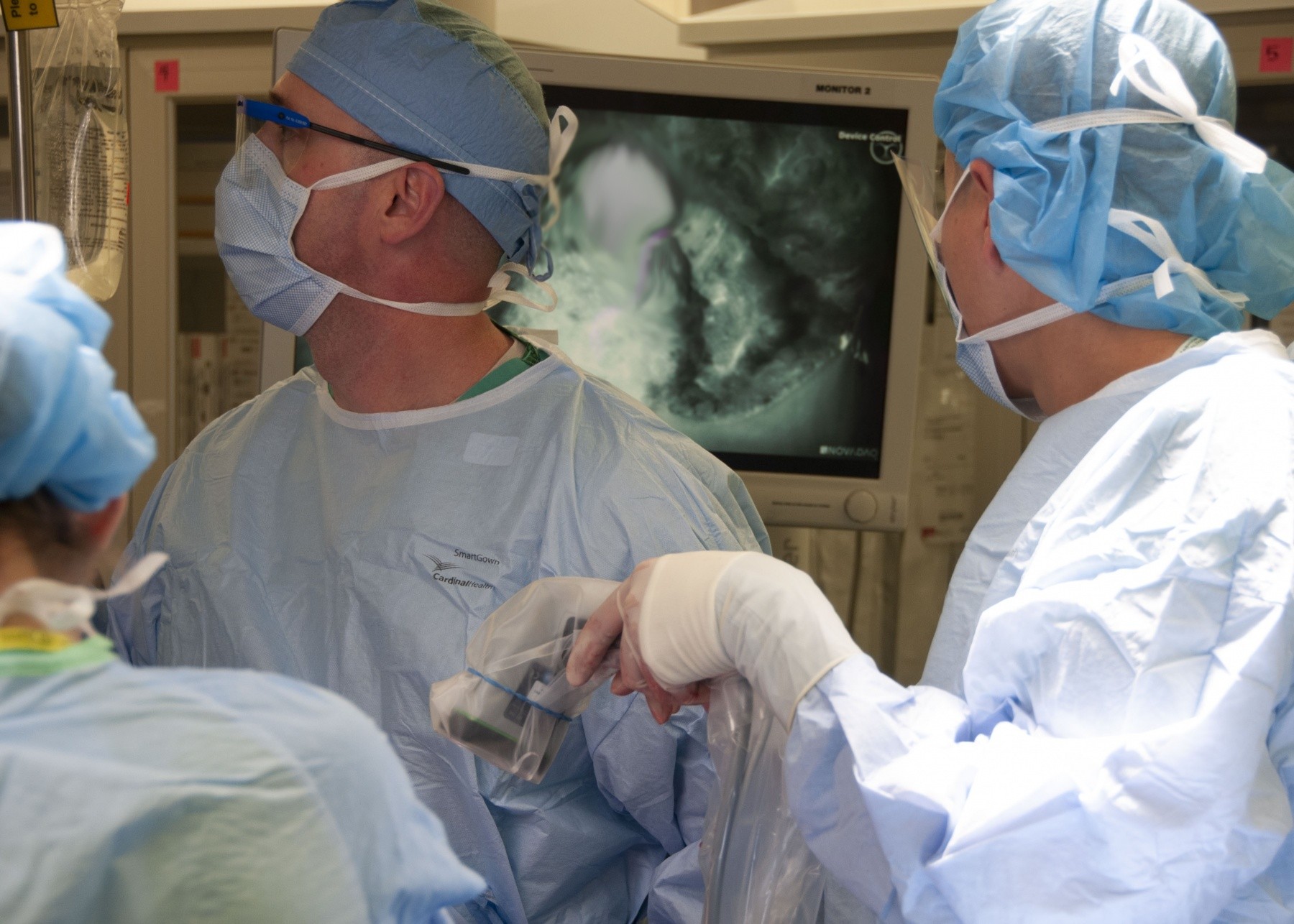
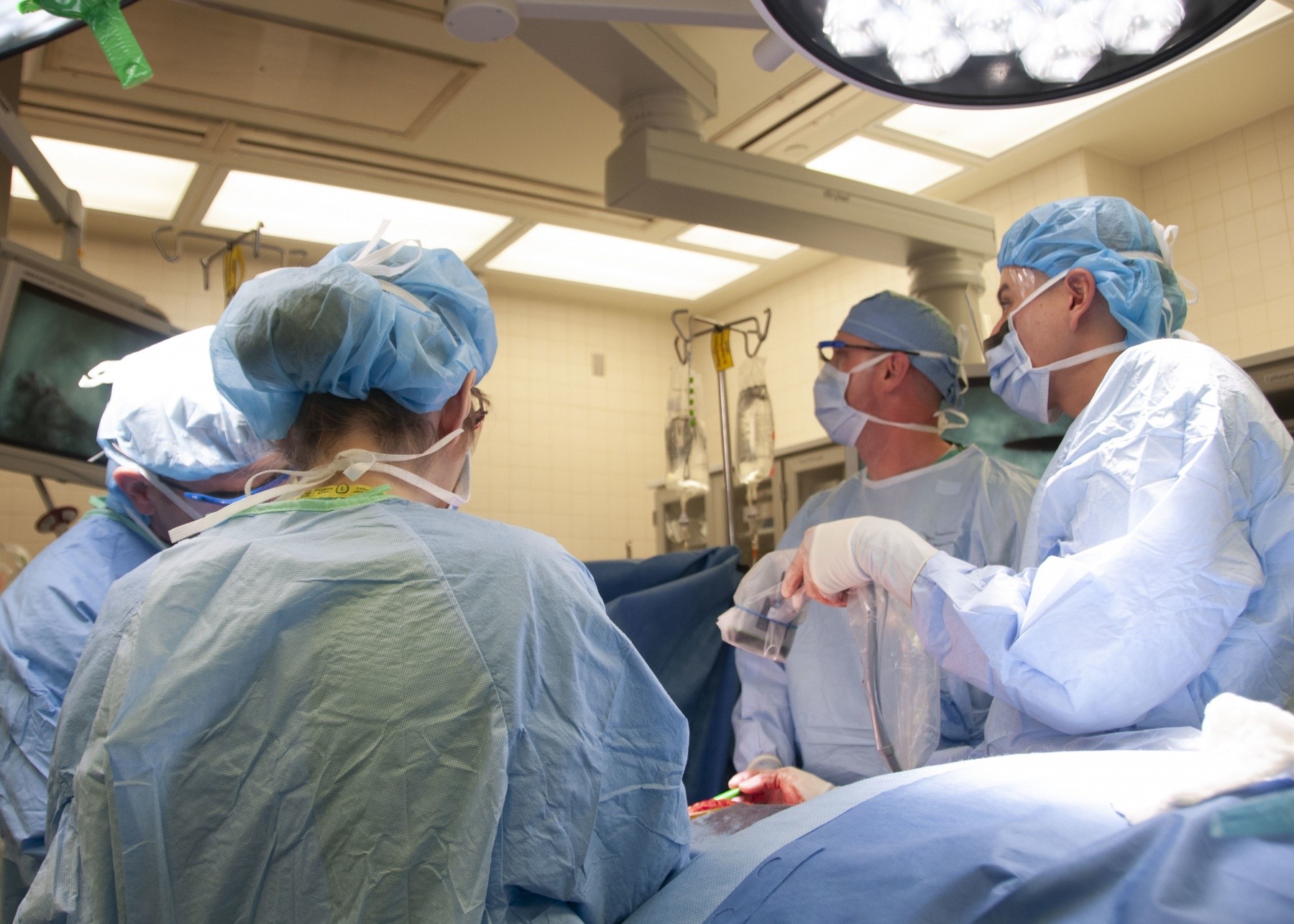
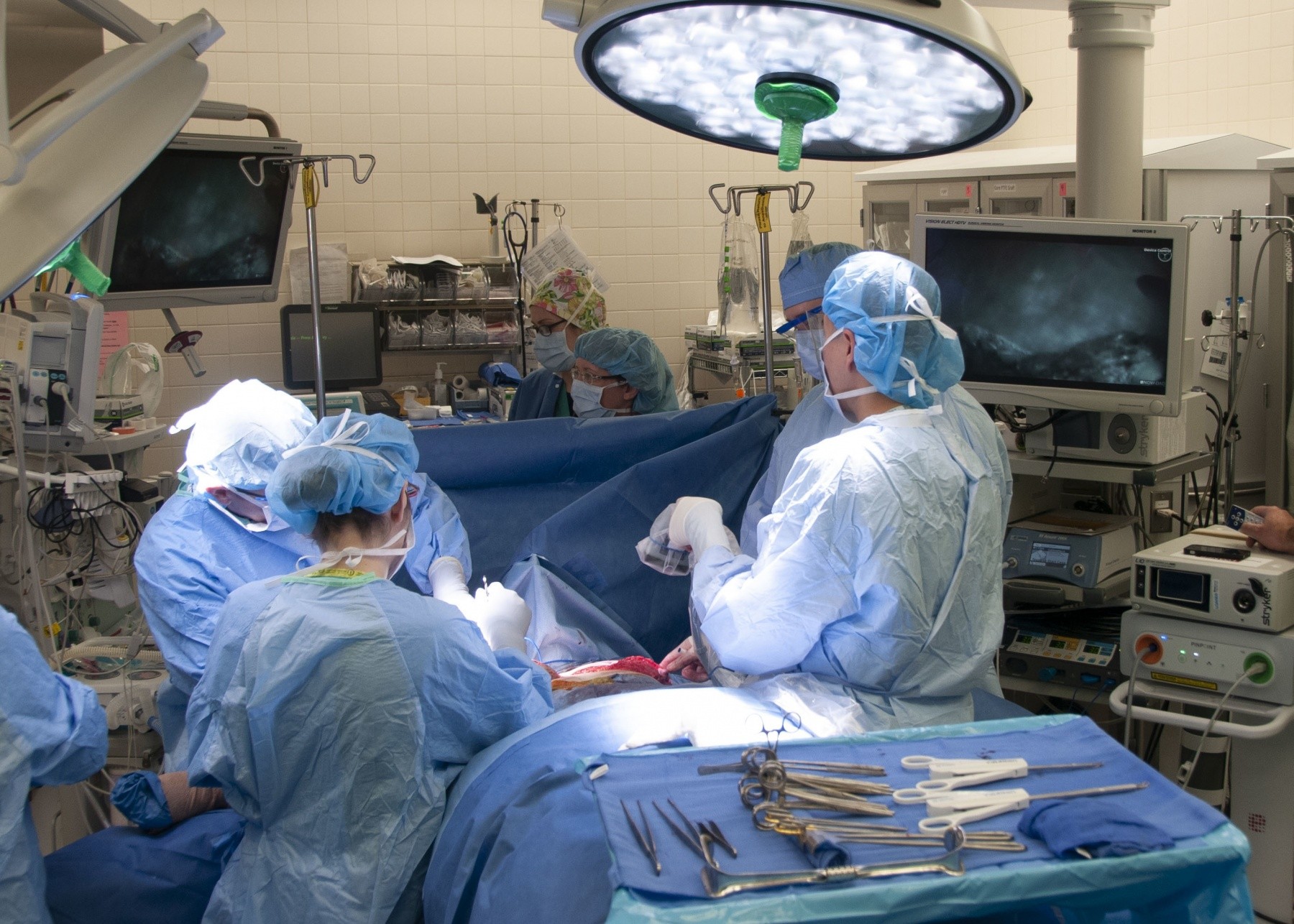
Due to a family history of breast cancer and for emotional well-being, Elizabeth elected to have a double mastectomy. As part of reconstructive options, Lt. Col. Owen Johnson III, introduced Elizabeth to a laser-assisted indocyanine green angiography (LAICGA) portable handheld imaging device, a fairly new surgical tool which enables surgeons to visualize microvascular blood flow and related tissue perfusion, making more complex surgical cases possible. The device had never been offered at WBAMC before Elizabeth's case, but is fairly common at cancer centers.
"(Laser-assisted indocyanine green angiography) uses laser and fluorescence from an injectable medication called indocyanine green to look at very small blood vessels which are invisible to the naked eye," said Johnson, chief of Plastic and Reconstructive Surgery at WBAMC. "Using this technique, you can (theoretically) use a permanent implant on the same day as their mastectomy, so it's all done in one day."
Although the one-step breast reconstruction, also known as Direct to Implant, has been practiced for years on select candidates, Elizabeth's anatomy and location of the tumor made the procedure risky without the aid of the LAICGA device. The device consists of a portable-handheld imager which surgeons aim at the surgical area, and can then visualize minute vessels for perfusion assessment on displays, a capability Johnson describes as "having x-ray vision". By doing so, the innovative procedure decreases chances of tissue necrosis. The device is also considered safe for use in microsurgery and gastrointestinal surgery cases.
"We're always in a position where we have to make a prediction or guess as to whether there is enough blood supply that (skin) will live," said Johnson. "If we're wrong, if we think the skin looks okay, and we put in tissue expanders or soft tissue implants and a week later all that skin is dead, then the implants get infected we go back to surgery and remove everything. It's a huge disaster because now the patient has had additional surgeries, they have infected wounds that will take a while to heal, and the reconstruction basically starts all over."
According to Johnson, Elizabeth's tumors were very close to the surface, so close that following the mastectomy the skin was so thin doctors could see their fingers through the skin.
"This is the exact scenario that if I had not had (the device) I wouldn't have proceeded," said Johnson, a native of Woodbridge, Virginia. "Under normal circumstances I would have abandoned reconstruction. If (surgeons) proceed with reconstruction (in cases such as Elizabeth's) and they're wrong it's devastating for the patient. Reconstruction would take multiple surgeries and probably two years to recover from that, so it's a very high-stakes decision (operating without the aid of the device) to make."
While the Holshousers wait for test results from biopsies to determine if all the cancer was removed, and for medical reasons, Elizabeth opted for tissue expanders, which will allow her time to recover and adjust before her final surgery for permanent implants. Without the use of the device, Elizabeth would have been looking at a longer reconstruction period than what was offered her.
"I felt completely blessed to have (WBAMC Oncology and Plastic and Reconstructive Surgery) as my medical team. They've been on board with each other and I've had appointments with both to discuss at the same time," said Elizabeth.
"The amount of time these guys put in with (Elizabeth) and thinking outside of the box, it's amazing, these guys are incredible," said Kenneth. "If more patients can have the benefit of the new device, that's good news all around."
Aside from minimizing procedures and recovery time, the introduction of the device at WBAMC changes the operations available to breast cancer patients while providing confidence that WBAMC may provide the same cutting-edge technology available at other medical centers.
"It really has opened a new frontier of breast reconstruction at WBAMC because now there's truly no treatment we can't offer in terms of breast cancer treatment or reconstruction," said Johnson.
The surgical team at WBAMC has already conducted multiple surgeries using the device, including a successful direct to implant case. The device can potentially be used for trauma patients as well.

Social Sharing