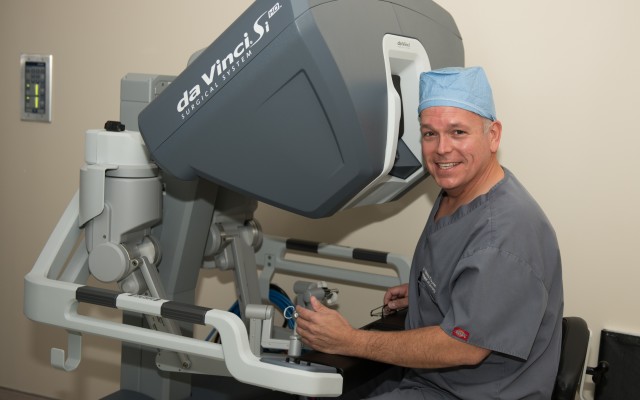
FORT GORDON, Ga. (Aug. 6, 2015) -- "It's not magic," Maj. Thomas Dykes, M.D., said. "It's still surgery." Dykes introduced the Eisenhower Army Medical Center's, or EAMC's, latest surgical tool: the robot-assisted laparoscopic surgery equipment, Aug. 5. The system went into regular use at EAMC late last month.
A long-standing technique preferred in most cases over open surgeries, laparoscopic surgery is minimally invasive surgery, sometimes called bandaid surgery or keyhole surgery. It is a surgical technique in which operations are performed through small incisions.
The robot-assisted technique is a more sophisticated, refined technique designed to expand the surgeon's capabilities.
When compared to conventional laparoscopic surgery, the newer technology "allows the surgeon to dissect and suture with [more] precision and ease," Dykes, a urologist, said.
The benefits compared to open surgeries can include a shorter hospital stay, less blood loss, less reliance on narcotic pain medicine, a faster recovery and minimal scarring.
The robot-assist equipment does not replace the surgeon, Dykes was quick to point out.
"The term 'robot' connotes an assembly line," he said. "The robot doesn't do the operation but is a robotic extension of the surgeon." In other words, the robot is not autonomous. It does not think or act. It's the surgeon who is thinking and acting.
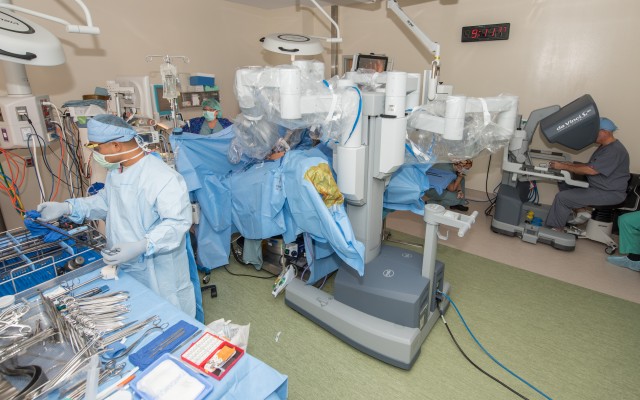
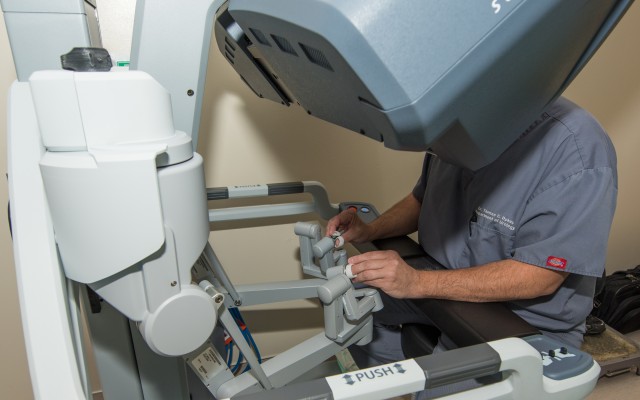
Through small incisions, miniaturized, wristed instruments and a high-definition 3D camera are inserted into the patient. Seated at a console, the surgeon views a magnified, high-resolution 3D image of the surgical site inside the body. The robotic and computer technologies seamlessly scale and translate the surgeon's hand movements into precise micro-movements of the instruments.
The 3D view is created by using two cameras side-by-side to create a binocular view, similar to a 19th century stereopticon or 20th century View Finder. There are no special, movie-theater 3D glasses. The view from a conventional laparoscopic single camera is similar to today's 2D television. The 3D view adds depth and dimension to the surgeon's field of vision. The cameras can provide up to 10x magnification, making the surgeon's motions more "precise and accurate," Dykes said.
"This is a natural evolution of laparoscopic surgery," he said. "Laparoscopic instruments have less articulation." With the new system, called a da Vinci Surgical System, "the instruments have a 'wrist,' similar to the human wrist with a greater degree of mobility, up to 360 degrees," he said.
Having wrists gives surgeons more latitude. "There is greater freedom of movement in a small space," said Col. Yong Choi, M.D., and chief of minimally invasive and bariatric surgery at EAMC. The surgeon can be "more precise in some patients."
Not all surgery patients are good candidates for robot-assisted surgeries, said Col. Jim Frizzi, M.D., and chief of surgery. And the decision to employ the technology is generally up to the surgeon.
The discretion of the surgeon is based on whether or not the use of robot-assisted equipment is medically advantageous to the patient's outcome. There are instances where there is no difference between conventional laparoscopic and robot-assisted surgery.
Sometimes the decision to use the da Vinci system is colored by other, more pedestrian variables such as the sheer length of a surgery.
"There are ergonomic benefits for the surgeon," Choi said. "Sitting at the [control] console reduces fatigue on the surgeon" during long sessions.
These systems, which cost in the neighborhood of $1 million each and have been in development for about 15 years, are installed across Army Medicine. The first robot-assisted pediatric surgery was performed last month at Joint Base San Antonio-Fort Sam Houston, Texas' Brooke Army Medical Center.
According to Choi, however, EAMC has the latest system with two controllers that lets two surgeons work on the same patient at the same time as needed, and is a training aid as well.
Certifying surgeons to use the equipment takes approximately six months, according to Dykes, and includes online training, time on a simulator and in the classroom, followed by hands-on training in an animal lab and finally, proctored human surgery. During proctored training, a certified surgeon oversees the trainee and, similar to some driving instructors, has a dual set of controls giving the proctor the ability to safely interrupt the procedure before a mistake can be made.
The urological staff is currently performing surgeries. Three general surgeons are being trained and, according Frizzi, all six will be trained within the year. Their focus is on bariatric surgery and gallbladder surgery. However, it will soon encompass many of the common laparoscopic surgeries being performed today. The cardio-thoracic and gynecologic surgery services will soon follow.
At EAMC, the robot-assisted surgical capability will be employed by surgeons performing a full range of urological, gynecological, cardio-vascular and general surgeries.
From both the doctor and the patient's perspective, "the surgery doesn't change," Dykes said. "It's the tool that's different."
But robot-assisted surgical equipment does put EAMC on a level playing field.
"[EAMC] is now in line with the new, advanced technology and delivers the same benefits civilian [surgery centers have]," said Choi. "It offers retirees and military members modern care with the best equipment and the best technology out there."



Social Sharing