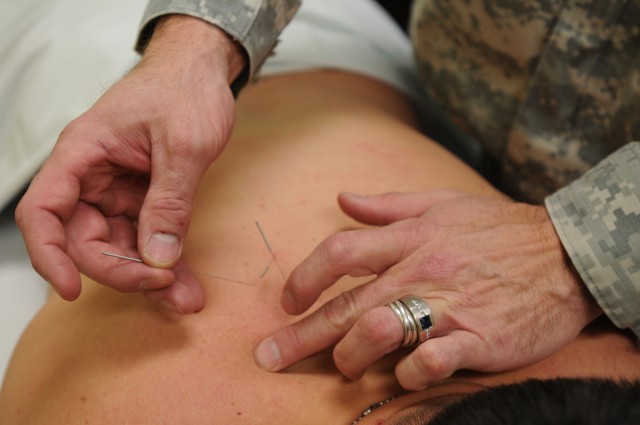
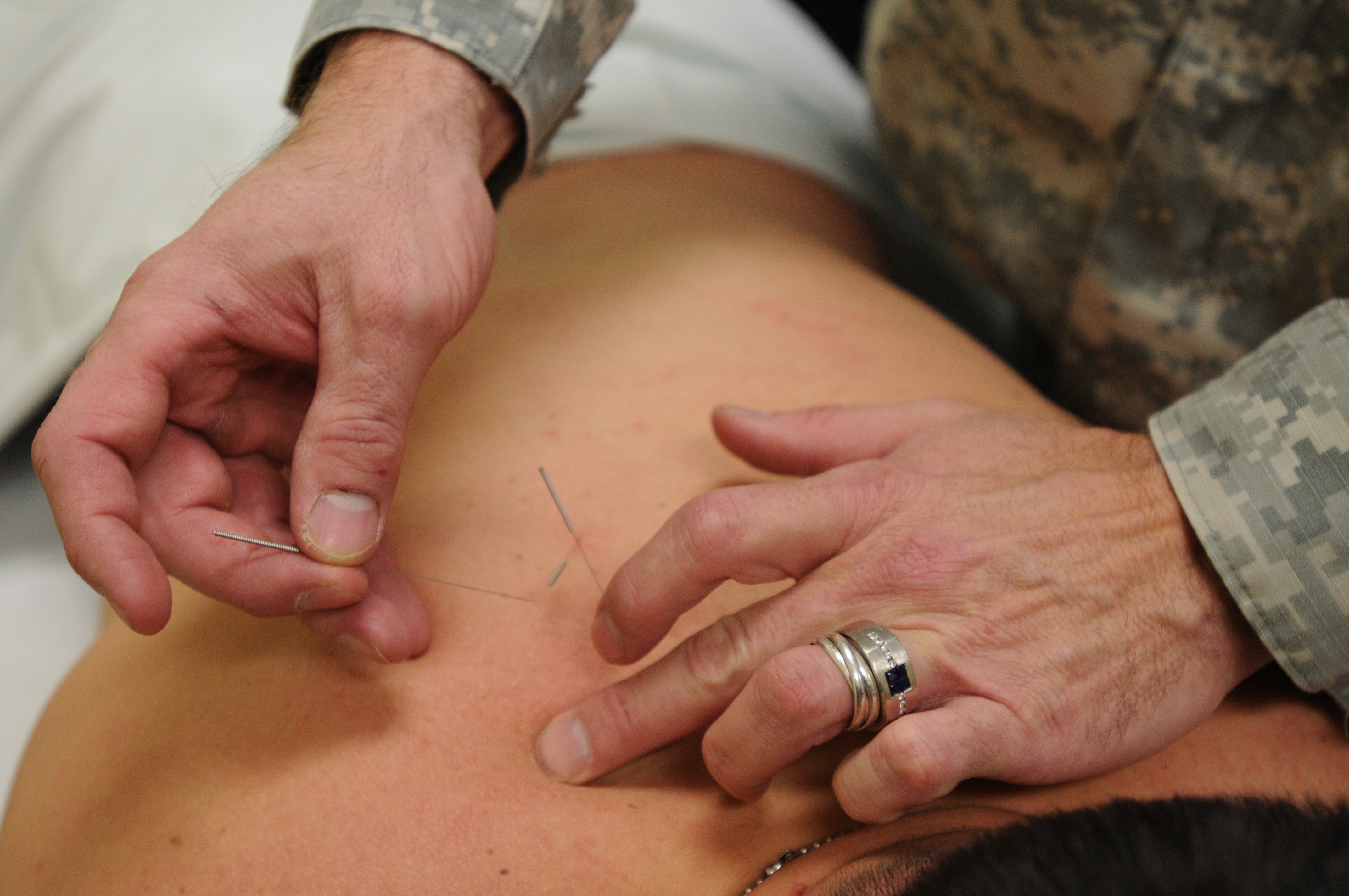
WASHINGTON (Army News Service, May 2, 2014) -- Acupuncture and other forms of alternative and complementary medicine are helping reduce the use of opioids to block pain in Army patients, the service's assistant surgeon general said.
Brig. Gen. Norvell V. Coots, deputy commanding general of the U.S. Army Medical Command and assistant surgeon general for force projection, testified Wednesday, at a hearing of the Senate Veterans Affairs Committee about overmedication concerns.
In 2011, 26 percent of all service members were prescribed at least one type of opioid medication, Coots said. That number was brought down to 24 percent last year, Coots continued, partly due to the use of acupuncture, yoga and other alternatives to medication.
"It is a small difference, but I think it still represents a big cultural change and a move ahead," Coots told the committee.
Army Medicine has been working to change its culture since 2010, when the Pain Management Task Force issued recommendations, Coots said. The Army-led task force, which included members of other services and the Veterans Health Administration, examined best practices for pain management at 28 medical centers. One of the task force recommendations was to explore alternative treatments such as acupuncture, meditation and biofeedback.
Biofeedback is the process of gaining greater awareness of the body's functions, often using sensors and instruments. The goal is to try to control functions such brainwaves, muscles, heart rate and pain perception. Biofeedback is sometimes used to treat headaches, especially migraines.
The Army has had a large upswing in the use of alternative medicine in the past few years, Coots said, and its use has been written into the Army's Comprehensive Pain Management Campaign.
"All the statistics are showing now that with a big push for cultural change with integration of these alternative modalities, that we're seeing a downturn in opioid usage across the military, particularly across the Army," Coots told the committee.
Robert Petzel, under secretary for Health, Department of Veterans Affairs, also testified at the hearing. He said VA has added chiropractic care, massages, mindfulness meditation, exercise therapy and relaxation therapies to its treatment plan for pain.
"The burden of pain on veterans is considerable," Petzel said.
A 2011 Institute of Medicine report noted that more than 116 million Americans suffer from chronic pain. The annual cost of that pain in the U.S. was estimated at $560 billion, including health care expenses, lost income, and lost productivity. Coots included that figure in his written statement to the committee. That statement was co-authored by Col. Kevin T. Galloway, Army Pain Management program director, who stood by Coots' side at the hearing.
Their statement pointed out that Interdisciplinary Pain Management Centers, known as IPMCs, are being established at each of the Army's eight medical centers. The IPMCs will be staffed by a multidisciplinary team of providers working to rehabilitate patients through a program that includes alternative treatments.
The written statement to the committee also discussed a tele-mentoring initiative involving the IPMC staffs. Called the Army Pain Management Extension for Community Healthcare Outcomes, or ECHO, this initiative is modeled after a project at the University of New Mexico. In fact, the Army is completing a two-year collaboration with the university to adapt this program. Essentially, ECHO uses weekly video tele-conferencing to link IPMC experts with remote primary care providers.
"Treating pain is one of medicine's oldest and most fundamental responsibilities, yet modern medicine continues to struggle in its efforts to understand pain mechanisms and to relieve pain and suffering of our patients," Coots said.
The Centers for Disease Control identified prescription medication abuse as an "epidemic" in the United States, Coots said, adding "The military is not immune to these challenges."
The Army is adding clinical pharmacists to its patient care teams as another initiative to stop medication abuse. Clinical pharmacists can identify Soldiers with polypharmacy risk -- dangers due to using multiple medications -- and communicate those concerns to health care providers.
Coots reported the addition of clinical pharmacists translates into decreased overall costs, fewer adverse drug-related events, reduced hospital admissions, and improved patient outcomes.
"Effective solutions must involve innovative strategies, comprehensive solutions and collaborative efforts," Coots told the senators.
(For more ARNEWS stories, visit www.army.mil/ARNEWS, or Facebook at www.facebook.com/ArmyNewsService)
Related Links:
Army looking at yoga, acupuncture to treat pain
Army takes a hard look at chronic, acute pain
Army Medicine leaders honored for Pain Management efforts
VIDEO: Pain Management Task Force
Social Sharing