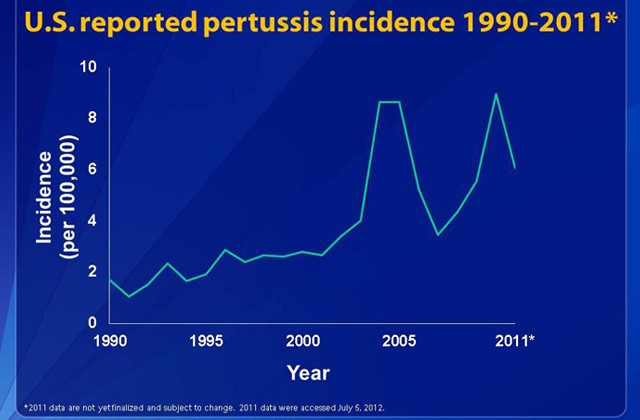
FORT RUCKER, Ala. (August 16, 2012) -- Pertussis, also commonly known as whooping cough, used to be considered a disease of the past, but over the last 20 years there has been a dramatic increase in the incidence of this disease.
Cases have risen in the United States from an estimated 3,000 cases to well over 27,000 cases per year, according to the Centers for Disease Control and Prevention. The number of reported pertussis cases in Alabama in all ages has increased from 68 in 2008 to 315 in 2009. Within the first six months of 2010 there were 93 reported cases of pertussis.
What is pertussis?
Pertussis is a highly contagious bacterial disease that causes uncontrollable, violent coughing. The coughing can make it difficult to breathe and a deep "whooping" sound is often heard when the patient tries to take a breath. It is a serious disease that can cause permanent disability in infants, and even death.
When an infected person sneezes or coughs, tiny droplets containing the bacteria move through the air and the disease is easily spread from person to person. The disease can affect people of any age and usually lasts six weeks, according to the CDC.
Before vaccines were widely available, the disease was most common in infants and young children. Aggressive immunization practices have decreased the incidence in young children and it is often now seen in adolescents and adults who need booster shots to increase their immunity.
How will I know if my child has it?
Symptoms are similar to the common cold and usually develop about a week after exposure to the bacteria. Severe episodes of coughing start about 10 to12 days later. In children, the coughing often ends with a "whoop" noise, although this is not usually seen in patients under 6 months or in adults, according to the CDC.
Between coughing spells the patient may appear well -- it is rarely accompanied by a fever. Of particular concern is when the patient's cough leads to vomiting or loss of consciousness. When this happens, people should seek medical help immediately. Other pertussis symptoms may include a runny nose and diarrhea.
Should I take my child to see a medical provider?
If a child comes down with cold symptoms that include a cough, parents should talk to their medical provider. The initial diagnosis is usually based on the symptoms; however, when the symptoms are not obvious, pertussis may be difficult to diagnose.
To know for sure, the medical provider may take a sample of mucus from the nasal secretions and send it to a lab, which tests it for pertussis. While the results are pending, the medical provider will initiate treatment -- usually a course of antibiotics that can help the symptoms go away more quickly and reduce the patient's ability to spread the disease to others.
Outcomes for older children and adults are generally good, while infants have the highest risk of death and will need careful monitoring to ensure their breathing isn't compromised.
How can I protect my Family?
Prevention of this disease through vaccination is highly recommended. The diphtheria, tetanus, and pertussis vaccination protects children against pertussis infection and can be safely given to infants. A series of five DTaP vaccines is recommended -- given to children at ages 2 months, 4 months, 6 months, 15-18 months and 4-6 years. To boost immunity in older children and adults, the Tdap vaccine is recommended at age 11 or 12, and every 10 years thereafter up to the age of 65.
During a pertussis outbreak, unimmunized children under age 7 should not attend school or public gatherings and should be isolated from anyone known or suspected to be infected. This should last until 14 days after the last reported case.
More information, call the Alabama Department of Public Health at 1 (800) 469-4599; or Fort Rucker Public Health Nursing at 255-7930.

Social Sharing