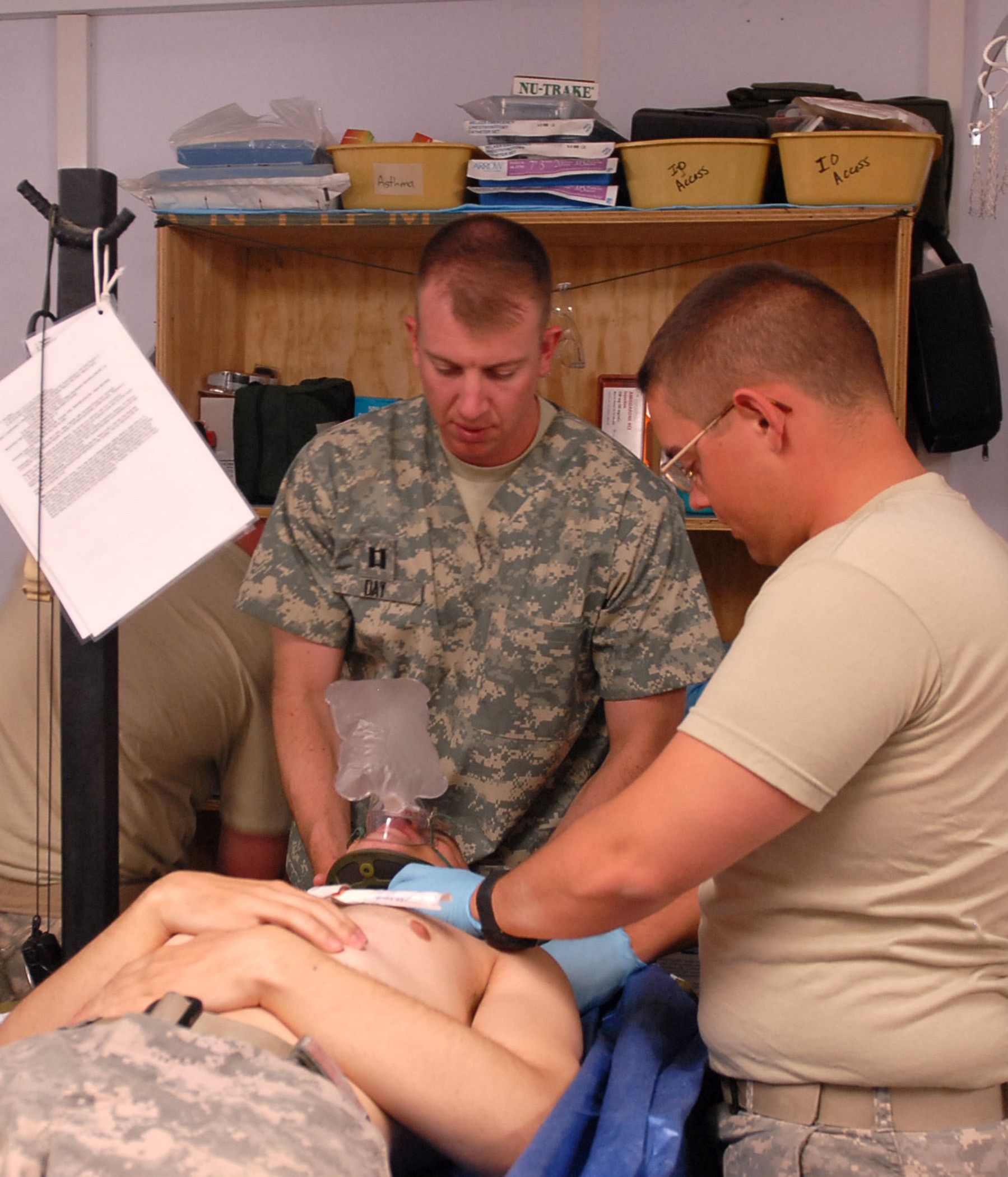
WARDAK, Afghanistan - It's late at night, as medics from 4th Battalion, 25th Field Artillery Regiment and 2nd Battalion, 87th Infantry Regiment, 3rd Brigade Combat Team, 10th Mountain Division, hover over U.S. Army Pfc. Nicholas Henrich's prone body inside the medic station at Forward Operating Base Airborne in Wardack province, Aug. 8.
"Hey man, what happened'" asked Spc. Timothy Currie as he holds Henrich's neck stable while leaning down to hear his response.
"We got hit by an (Improvised Explosive Device)," replies the Fairborn, Ohio, native with a raspy voice. "I was the driver, and we were just sitting there. It's hard for me to breathe."
To the side of the trauma table U.S. Army Sgt. Jean Nelson watches as the medics begin treating the young Soldier. The initial signs indicate Henrich may have suffered severe damage to his chest. However, the prognosis is good for this Soldier because he is only playing the role of a casualty.
"This is a part of our mandatory (Emergency Medical Technician) recertification training," Nelson stated. "Tonight, we are covering the steps necessary to properly assess and treat different injuries associated with trauma to the chest."
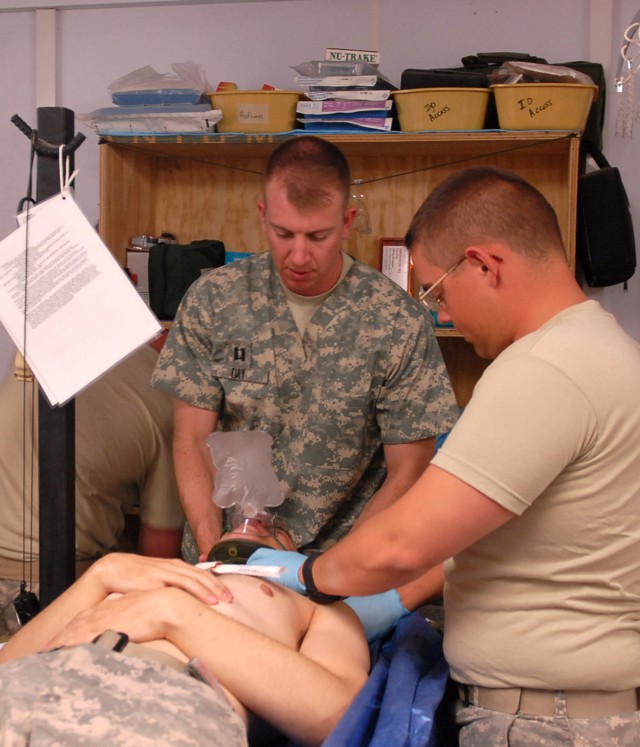
Currie reaches to his right to grab the oxygen mask and place it over Henrich's face to help him breathe as U.S. Army Pfc. Robert Shipley and Spc. Frank Romanowski work from head to toe, looking for any other injuries and symptoms that could help them diagnose and treat Henrich faster.
According to Nelson, the medic at the head of the table normally runs the trauma, while two more medics flank him to his left and right - one working on obtaining vitals as his counterpart targets IV access.
"Scenarios like this are important," stated Shipley, a medic who will soon be working with Company A, 2-87 INF, in the Tangi valley region. "We're always doing classes and refreshers so we don't forget anything, and it reminds us we always have to be on our toes."
Nelson said it's imperative for the medics to move with speed and efficiency when treating patients, regardless of whether they are in the aid station or out in the field, while keeping a clear head.
"Sometimes, when things are crazy, you're moving fast, and this training helps us to stay up to date on our procedures to help treat the patient and get him ready for transport quickly," the Newark, N.J., native said.
For this training, the noncommissioned officers and the battalion surgeon stand off to the side, offering helpful reminders, adding new kinks, and evaluating their troops along the way as they work through the trauma.
"There are two methods to this training," U.S. Army Capt. Charles Day, 2-87 INF, surgeon, added. "We can lay out a basic, well-planned scenario ahead of time so they know what they're going into, or we can throw them into it. The latter is what we're doing, and it allows us to assess what improvements are needed."
"Medicine is a perishable skill," added Currie, who is running the trauma for only the second time. "You don't want to second-guess yourself while trying to think through the scenario. You ask yourself, 'What could be happening' What do we need to be doing to make this better''"
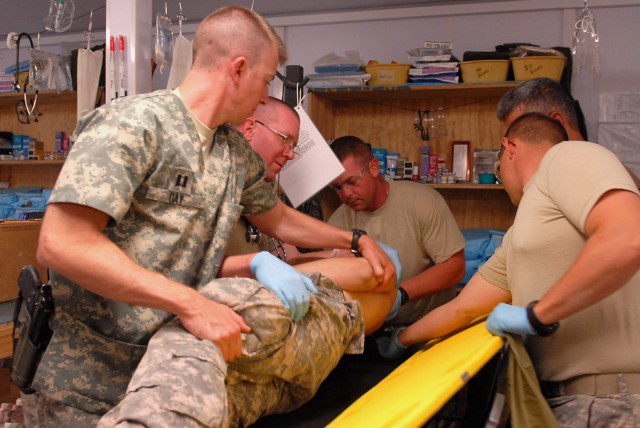
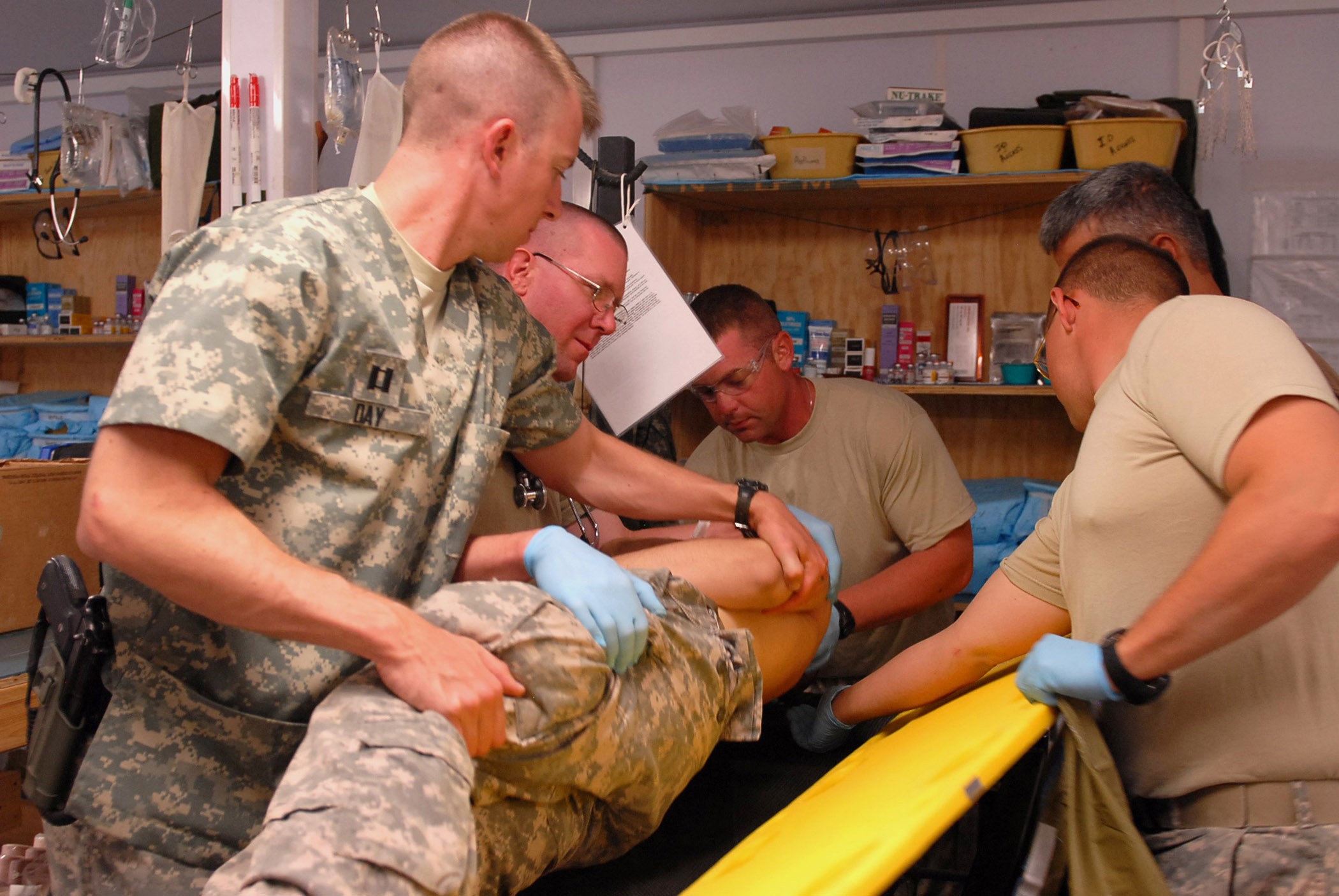
Currie quickly calls for a backboard. Within seconds, what looks like a yellow surfboard is in plain sight and the medics prepare to carefully roll Henrich to his side to slide the board underneath him.
"Ready on my count," Currie directs. "One. Two. Three."
In one smooth motion, Henrich is rolled to his right side. As Currie and Romanowski hold him as still as possible, Shipley quickly inspects his spine and gives the all clear. The board is then slid underneath him and they carefully move the patient and the board as one, back flat on the gurney.
"This is a great learning experience," said Shipley, who is the junior medic in the aid station. "There's always something new you can learn as you're taking care of people."
Upon further examination, the medics determine Henrich has an Attention Numo-Thorax, a condition common in blunt-force trauma to the chest that causes the lung to collapse. Henrich will need a chest tube to inflate his lung and help him breathe.
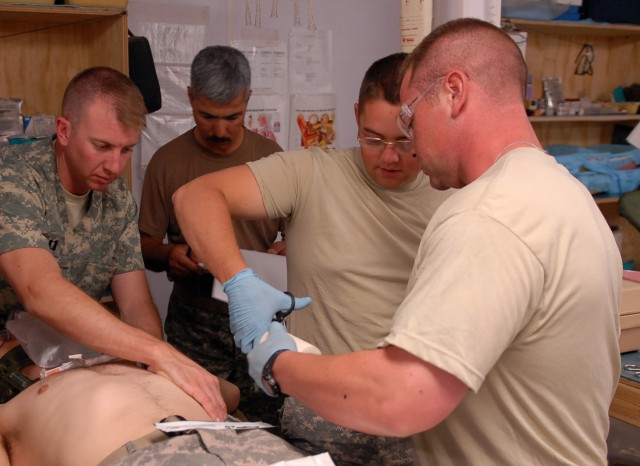
At this moment, the training slows and Day moves in as Currie walks around the table to Shipley. These medics, who have spent most of their time during the deployment in the field, do not place chest tubes in patients outside the wire because, according to Nelson, it offers another obstacle for the patient - infection.
Currie, who hasn't put a chest tube in a patient in nearly nine months, walks slowly through the procedure with Shipley, who also has a long gap in performing this procedure, as Day approaches the table to ensure he is providing the young medic with the right steps and location to properly inflate Henrich's collapsed lung.
"It's a lot of pressure to know somebody's life depends on you," stated Currie with a serious look. "You know at any time you can be the only one there, and this person's life is lying in your hands."
Under the watchful eye of Day, Shipley correctly simulates placing the chest tube in the correct location on Henrich's left side.
The medics have seen their fair share of injuries reflected on this particular procedure. Several months ago, Currie was a part of a team that helped save the life of an Afghan National Policeman.
"Not too long ago we got an ANP guy in here," added Currie. "His vehicle got hit by an IED and he was thrown about a 100 meters. It took them almost 45 minutes to bring him here and when he arrived, he was circling the drain, but we got on it, resuscitated him and saved his life."
"I couldn't be happier with the medics I have," added Day. "They hit the key points and knew the things they were supposed to know. Their professionalism allows me to step back and manage the chaos while they execute everything."

Social Sharing