
MADIGAN ARMY MEDICAL CENTER, Joint Base Lewis-McChord, Wash. – In garrison, military medicine may not look too different from civilian healthcare. But, downrange? That is quite a different thing. Over years of medical school and residency, military doctors get a wealth of knowledge and experience in providing care to patients. Yet, they get precious little exposure to how they will function as military doctors when they are deployed, especially to a combat zone. Madigan Army Medical Center on Joint Base Lewis-McChord, Wash., works to change that.
Each spring, the month before graduation, the Andersen Simulation Center presents a week-long event known as Capstone.
“The goal of the GME [Graduate Medical Education division] Capstone field exercise is to expose all graduating interns, residents and fellows to the continuum of casualty care from point of injury through strategic evacuation,” said Lt. Col. (Dr.) Benjamin Baker, emergency medicine physician and director of the Andersen Simulation Center. “Capstone provides didactics and hands-on experience to help prepare them for the roles they will fulfill in both garrison and deployed environments and highlights the operational expertise of enlisted medical personnel.”
Early on in the week, attendees get those didactics – the classroom training and information sharing. Later in the week, they donned their combat equipment and took to Leschi Town for as real world an experience as they have had yet.
The event consists of lectures, subject matter expert panels, tactical combat casualty care certification, procedure demonstrations and an operational continuum of care field exercise where all graduating residents, interns and fellows get fully immersed in combat care.
Over the dozen years this culminating event has been staged, it has expanded and added new elements with each iteration. The original half-day seminar on leadership and expectations for Army physicians has become a week-long, hands-on experience.
This year, the 124th Forward Resuscitative Surgical Detachment treated the residents to a demonstration of advanced resuscitation capability such as resuscitative endovascular balloon occlusion of the aorta (REBOA) which serves to hold critically ill patients over until they can receive life-saving surgery. These demonstrations took place in the FRSD’s advanced trauma life support section in their new chemical biological protective shelter.

Another feature of this year’s event was the incorporation of training with military working dogs. Though physicians do not get training in canine medicine, their medical expertise could be needed to sustain a MWD’s life if no veterinarian is available in a deployed situation.
“It was great to see the interactions between the residents and vet staff as they learned and appreciated new skills including physical examination of MWD's, canine CPR, how to muzzle a dog appropriately, etc.,” said Maj. (Dr.) Jeannie Bay, chief of Allergy/Immunology and director of the GME Central Curriculum.
During this exercise, medicine is brought out of the conceptual realm and into the real world these doctors will inhabit.
“In addition to getting exposure and experience with operational medicine, we also sought to cover transition to practice topics to help prepare them as they transition from trainee to staff physicians,” said Bay.
Those who participated in the exercise agreed on its value.
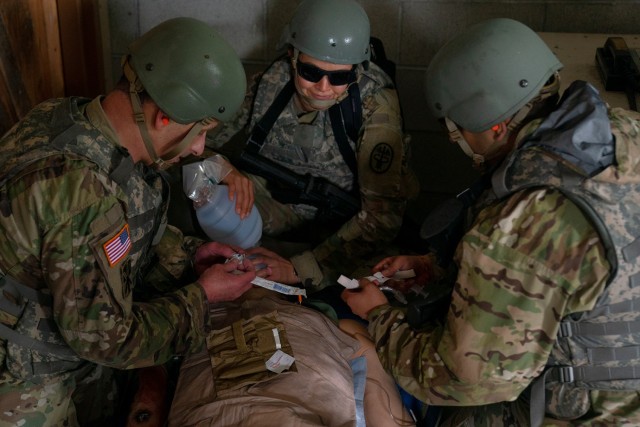
“We saw the techniques we have learned applied to life-like models and gained a valuable opportunity to practice skills,” Capt. (Dr.) Joshua Pollock, a resident physician in internal medicine said. “We received solid instruction on the first two days that is pertinent to upcoming moves and practice moving forward. The days that were spent in the field and with the round robin instructions were certainly the highlight.”
As Capt. (Dr.) Francis “Greg” Gause, a family medicine resident who attended Capstone, pointed out, this was some of the only operational-specific training these trainees receive.
Going into a combat-like environment in the practice village of Leschi Town with teams of military medical professionals from across the local military community filling out their roles as combat medics, medical evacuation pilots and flight crews, as well as Soldiers providing an approximation of a combat situation, Madigan’s trainees had to perform combat care to sustain their patients through the point of evacuation.
“It was the most "real-world" Army thing that I have done and really excellent training that brought a lot of different aspects of Battlefield Medicine into play,” said Gause.

The Sim Center team is likely already at work planning next year’s event as it is no small undertaking.
One aspect that residents and organizers alike repeatedly comment on as a distinct highlight of the exercise is the chance to work with other units they will be supporting when deployed.
“Our team had a great experience collaborating with MEDCOM [Medical Command], FORSCOM [Forces Command], SOCOM [Special Operations Command] and units across JBLM. Additionally, units from the U.S. Army Reserve, U.S. Air Force Reserve, and U.S. Navy Reserve and Washington Army National Guard significantly enhanced the graduating residents’ Capstone experience,” said Baker.
Madigan’s Capstone event is getting attention from well beyond JBLM’s gates.
Dr. Brian Lein, the assistant director for Healthcare Administration for the Defense Health Agency, was visiting while Capstone was occurring. He took the opportunity to get a look at the exercise.
“From I Corps, all of the people that came out that support this training event for our residents is unparalleled anywhere else in the military. And my hat's off to the I Corps leadership for continuing to support this,” he said. “I think it is an absolutely phenomenal coordinated training event that I think every resident regardless of service should be going through.”
Madigan’s Social Media Links:
Madigan’s Facebook:
www.Facebook.com/Madiganhealth
Madigan’s Twitter:
www.Twitter.com/Madiganhealth
Madigan’s Instagram:
www.Instagram.com/Madiganmedicine
Madigan’s LinkedIn:
www.Linkedin.com/company/madigan-army-medical-center/
Madigan’s YouTube:




Social Sharing