FORT BENNING, GA – “A cricothyroidotomy bleeds a lot,” warned Grady Health System Interim Trauma Medical Director Dr. Jonathan Nguyen. “Use combat gauze to pack it really tight when the airway is in. Then either whipstitch or take a stapler and physically close the space as much as possible.”
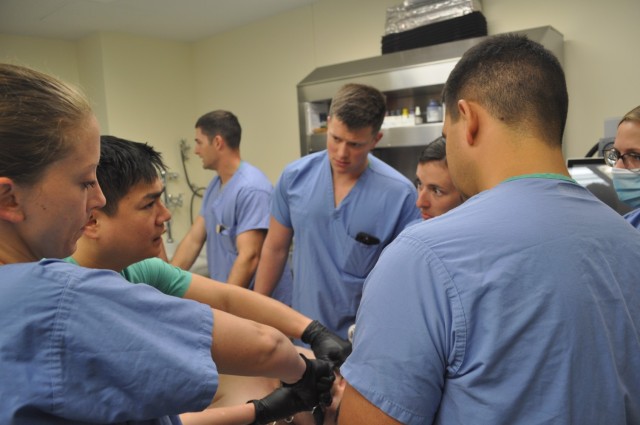
The Atlanta doctor walked 7 Martin Army Community Hospital graduating residents through the emergency procedure to establish an airway as part of the Family Medicine Residency Experience (FMRx). The weeklong operational medicine course is the capstone of the three-year residency program. It’s designed to reinforce the Tactical Combat Casualty Care (TCCC) needed to treat trauma on the battlefield.
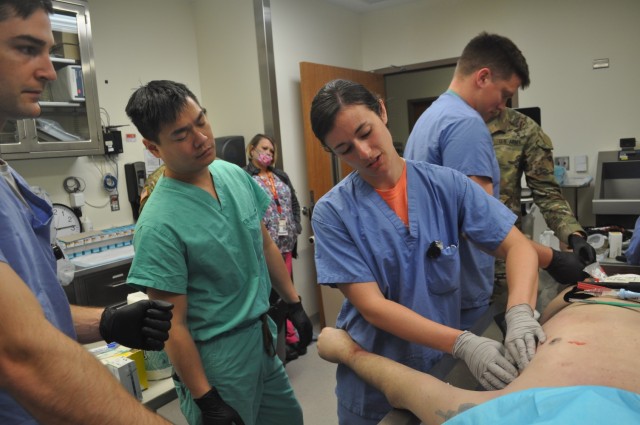
Under the guidance of Nguyen and BMACH Director of Osteopathic Medicine Maj. Michael Aguilar, the residents operated on a cadaver to practice making a quick incision on the throat through the cricothyroid membrane in order to place a breathing tube.
Capt. Victoria “Tori” Hall will be pcs’ing to Fort Campbell to serve as a Battalion Flight Surgeon for the 2-17 Cavalry Squadron of the 101st Airborne Division, after graduation. The Army brat who chose medicine because she wanted to make a difference in people’s lives said practicing the cricothyroidotomy on a cadaver definitely fortifies their readiness to perform the life-saving measure.
“Working on real human tissue is hands-down more valuable than a plastic model,” said Hall. “[A cricothyroidotomy] is an emergency procedure that is really a last resort.”
Fellow Uniformed Services University of the Health Sciences 2019 graduate Capt. Kyle Warren said while their medical school had a robust cadaver program, this tissue lab was unique.
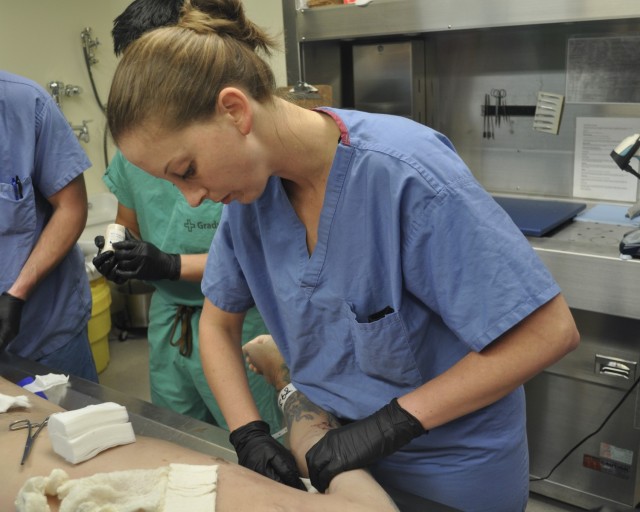
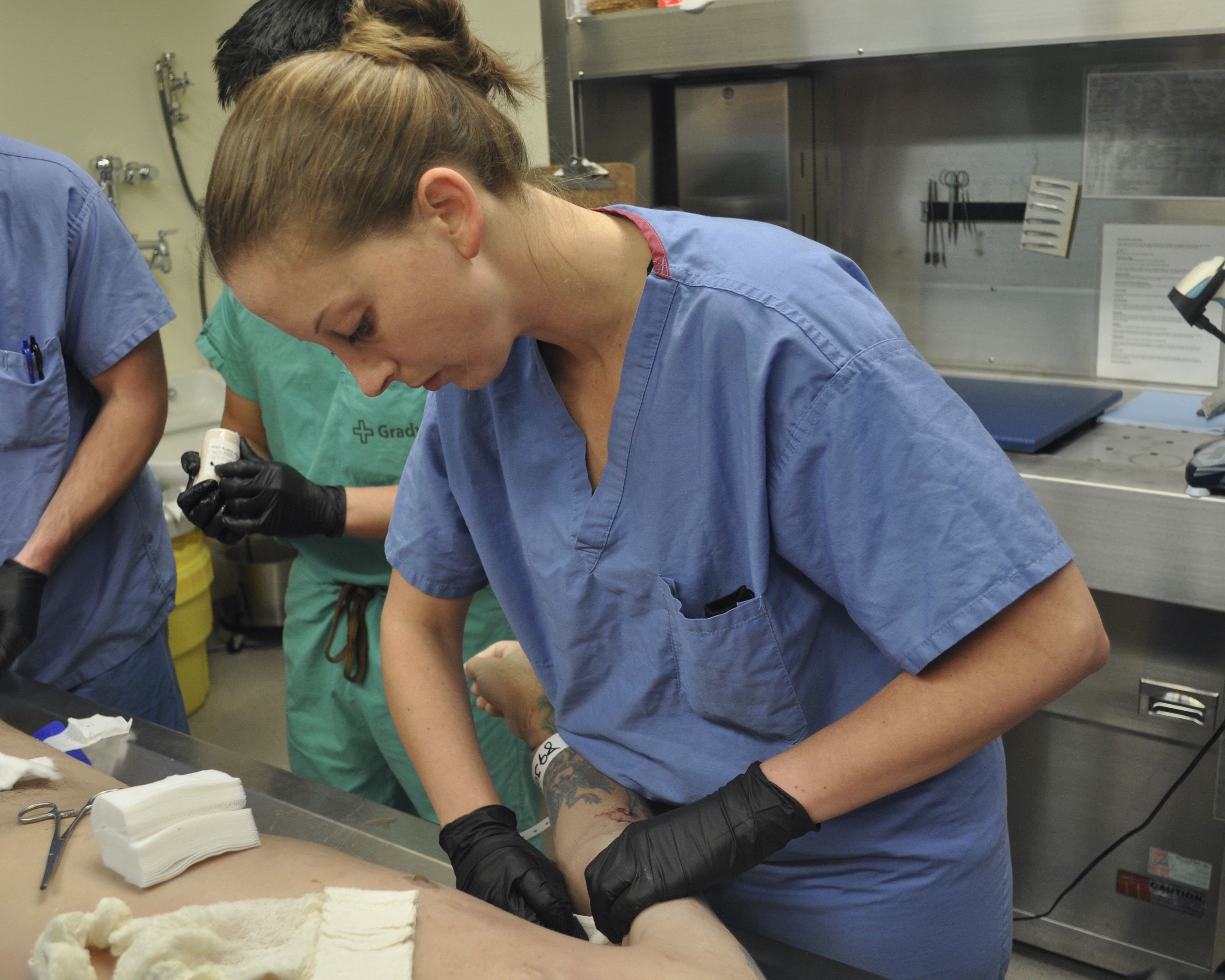
“One of the impressive features that I hadn’t experienced in the past was the capability to perfuse the cadaver (i.e. blood pumping through the vessels),” said Warren. “As such, we were able to simulate bleeding wounds that we could practice packing with gauze or applying a tourniquet to see if we could control the hemorrhage.”
Perfusing a cadaver enables BMACH faculty physicians to better test the skills they are training.
“The blood is coming from the right anatomical positions,” explained Aguilar. “It more readily translates to ‘real-world’ patient care. Getting realistic training … closer to actual patient care … will bring new insight for the learners.”
A critical skill expected of them as deployed field surgeons is stopping massive bleeding.
“When we talk about hemorrhage control, direct pressure is always preferred,” said Nguyen. “And if you guys have never put a tourniquet on before, I would suggest you put it on each other because it hurts. People will scream at you. It’s a lot of pressure.”
The residents then took turns performing a lateral canthotomy and cantholysis (LCC), in a bid to save a patient’s eyesight after blunt trauma to the face. The 5-step procedure quickly releases pressure on the optic nerve caused by sudden bleeding behind the eye.
“Basically you are going to clamp down on either side of that ligament and then you are going to take your iris scissors and cut all the way through,” explained Nguyen. “When you place your scissors down there, you are going to feel this really hard thing. It sounds morbid but keep cutting until it stops crunching.”
“The ophthalmologist will tell you, whatever cut you need to make, make it,” added Aguilar. “But don’t cut the globe.”
If a critically ill patient requires a rapid infusion of blood, medication or fluids, doctors must establish intraosseous vascular access. Nguyen showed the residents how to drill a sturdy hollow bore needle through bone to place an IO (intraosseous cannulation).
“Drill perpendicular to the actual bone,” advised Nguyen. “The tibular (tibia – larger bone on inside of lower leg) runs a little bit slower than the humeral (humerus – bone in upper arm), the humeral runs a little bit slower than the sternal (sternum – bone in middle of chest). Medics love the sternal because even if a patient has all four limbs injured, the sternal is still available.
“And if you need two IV access sites, I’ve also learned multiple IOs can work unless there is a fracture. If the tibia is intact, you can put two tibular IOs in and run multiple things at the same time. But if there is a fracture there, it’ll leak out of the fracture.”
Troop Command Commander Lt. Col. Ryan Knight warned placing the wrong size needle in the wrong location can lead to failure. He shared the tried and true technique which has not let him down in a decade of emergency medicine.
“I personally make room for my drill in my kit bag and carry a boatload of needles,” said Knight. “It’s not that heavy. And I’ve had that same drill since 2012. I’ve trained with it. I don’t know when it will finally die.”
A penetrating injury or severe trauma to the chest can cause air to fill the cavity, thereby limiting the lung’s ability to expand. To prevent the patient’s lung from collapsing, doctors must quickly release the air trapped in the chest by a temporary measure such as needle decompression (needle D) or inserting a more durable chest tube in between the ribs.
“When we do chest tubes in trauma, there is blood coming out,” said Knight. “When you clot those things off, you are causing tension pneumothoraces (air trapped in chest cavity or the very condition you are trying to treat) in our patients. When you go to altitude (i.e. helicopter evacuation) that’s where we are really noticing it.
“Don’t put a Heimlich valve (one-way valve) on there when you put your chest tube in, until the blood flow is stopping. You can’t clean it out. There is nothing you can do. All you can do is change it out.”
After the tissue lab, the 3rd-year residents tested their combat medical readiness by treating simulated mass casualties, before calling for a medical evacuation (MEDEVAC) to Lawson Airfield.
“The overarching goal of the FMRx is to intentionally expose the graduating residents to operational/battlefield medicine themes and topics,” explained Aguilar. “The intention is to expand their knowledge by stressing translation of their existing practice to new settings and different patient scenarios that are common to an austere medical provider. The MEDEVAC lanes are a culmination of 3 years of leadership, medical and Army officer instruction; giving the graduating seniors a chance to put it all together.”
Airborne and Ranger Training Brigade (ARTB) Capt. Aaron Spera developed several different scenarios such as severe burns, partial amputations and gunshot wounds to test the residents’ medical skills under stress.
“The best patient simulations are gunshot wounds to the chest that can develop into tension pneumothorax,” said Spera. “That would require a chest tube. And if they missed an injury, they would need to stabilize the casualty mid-flight.”
After carefully organizing and packing their kit bags, the residents ran through the exercise. Just as in combat, the field doctors had no idea what kinds of wounds they would encounter until they came upon the role player. They worked in pairs to assess, continually treat and MEDEVAC the casualty, all while under threat of enemy fire.
“If I have ten seconds to run out there and I see he has a partial amputation and it’s spurting blood everywhere, how much time do I have? I’m going to throw a tourniquet on him and I’m just going to move him out of there,” advised Spera. “The last thing we need is for me to become a casualty, or anybody I have with me. I’m going to get him out of harm’s way where I have got a little bit more time so I can do a more thorough assessment.
“Look at the big things. What is going to kill this guy? Probably not being in the hospital. I want to do what interventions I can. Hey, do I have a pulse on that ankle? Yes, I’m going to splint it as it lies. I’m going to stop these bleeds, I’m going to try to push meds, try to get fluids or blood on board. And I’m going to try to get to that bird as fast as possible.”
Hall said operating in the field and simulating even a portion of what the boots on the ground might experience was the most enjoyable part of the FMRx.
“I’ve flown on UH-60s [Black Hawks] and CH-47s [Chinooks] before and don’t generally get motion sick,” said Hall. “I’m looking forward to working more closely with the flight community soon!”
Warren, who will also be serving as a flight surgeon for one of the aviation units after pcs’ing to Fort Carson, said he chose that particular duty assignment because he is ready to experience the operational aspect of the military after being in school for the past decade.
“My favorite rotation during residency was my time spent on the labor and delivery unit,” said Warren. “There are a lot of raw emotions and it is very humbling to be part of the birth experience and help bring life into this world. It was also one of the most challenging because medical emergencies can happen in the blink of an eye.”
Both Warren and Hall said they will miss the camaraderie among their graduating class … strong friendships that got them through challenges posed by constant staff turnover and COVID.
“There is something comforting about being surrounded by a group of individuals going through the same difficulties as you who are able to comfort you after the loss of a patient, stress of a hard day, or difficult 24 hour call shift,” said Warren. “As I move onto my future assignment, I won’t be surrounded by as many close friends who I can bounce ideas off of or who will intimately understand what I am going through.”


Social Sharing