JOINT BASE SAN ANTONIO-FORT SAM HOUSTON, Texas (Jan. 7, 2022) -- A Marine Corps spouse and mother of five was 28 weeks pregnant when she caught a “mild case” of COVID-19 in June 2021.
Ashley Savidge Hernandez felt tired but wasn’t too concerned until she began to have trouble catching her breath. Alarmed for their baby, retired U.S. Marine Corps Gunnery Sgt. Carlos Hernandez drove his wife to Brooke Army Medical Center’s emergency room just to be safe.
Ashley had no idea she and her baby were about to embark on a month-long battle for their survival.
“It all seems surreal to me now,” she said on a phone interview, her voice still raspy from the ventilator. “I had no idea at the time how dire the situation was for me and my baby.”
Rapid Decline
Ashley had received the positive COVID-19 results on a Friday and by Monday, her condition had grown much worse.
“When I went in the room to check on her, I instantly knew something was wrong,” her husband said. “Her breathing was labored, and she could hardly get a full sentence out because she seemed out of breath with each word.”
Hernandez quickly loaded their five young children into the van and rushed Ashley to BAMC.
“I placed her in the wheelchair (and) took her into the ER, but I had to go get the kids and move the van, so I told her, ‘I'll be right back,’” he said. “Those were the last words I said to her, and they haunted me for weeks because at several points I thought God might be calling her home.“
Ashley’s oxygen levels began to quickly dip. Her health care team tried low-flow, then high-flow oxygen, but to no avail. In the intensive care unit, Ashley was told she needed to be intubated, which is when a tube is placed in the throat to help air move in and out of the lungs.
“I remember asking them what that meant, but things got hazy after that,” she said.
Ashley was in and out of consciousness, but vaguely recalls the tubes being removed and the loud hiss of the high-flow oxygen drowning out the concerned voices in the room.
U.S. Air Force Col. Phillip Mason was familiar with Ashley’s case, but thought she was improving until that point – until he got an urgent call.
“Ashley was deteriorating quickly,” said Mason, medical director, BAMC Adult Extracorporeal Membrane Oxygenation Program. “For some people, COVID-19 is a very rapidly progressing disease.”
After consulting with her husband, Mason and his team made the difficult call to put Ashley, now 29-weeks pregnant, on ECMO. “Ashley was on the brink of cardiac arrest without intervention,” Mason said. “We needed to stabilize her to allow for a better delivery and the best outcome for both patient and baby.”
“It was really the last-ditch effort to try and save her life,” Hernandez said. Knowing that felt “like a freight train just smashed into my own chest.”
ECMO Explained
Extracorporeal Membrane Oxygenation, more commonly known as ECMO, is a heart-lung bypass system used when other lifesaving interventions, such as oxygen therapy or a ventilator, have been exhausted. It removes blood from central vessels, oxygenates it, and delivers it back into the bloodstream. In essence, it replaces the natural functions of the heart and lungs while treatments and natural healing of the affected organs take place.
Established in 2012, BAMC has the only adult ECMO center in the Department of Defense and remains one of the few centers in the world with global air transport capability. In July 2013, the ECMO team completed the military’s first trans-Atlantic movement of an adult on external lung support -- a 5,000 mile, nonstop flight from Germany to San Antonio.
“We have a tremendous and unique capability to deploy to a combat zone, initiate ECMO and transport the service member back to a medical center,” Mason said.
While it’s been used for severe cases of influenza and other pulmonary diseases, in more recent years, ECMO has proven lifesaving for some patients with COVID-19-related respiratory failure. COVID-19 patients on ECMO typically have a 50-60 percent survivability rate, Mason noted, which offers an avenue of hope for patients and their families.
“In Ashley’s case, we were running out of options, and were concerned for her baby,” he said. “ECMO was the best course of action for her.”
Ashley’s husband vividly remembers the the call from BAMC, asking for his consent to place her on ECMO.
“I asked if they could wait for one hour so I could get my kids settled with someone, get to the hospital before the procedure, and at least tell her I loved her before she was sedated, but they said there was just no time, they had to move forward, so I agreed,” he said. “I knew what that acknowledgment could mean for her, the baby, and us as a family. It was in God’s hands at that point.”
The Delivery
As a specialized team inserted the ECMO tubes, obstetric and neonatal intensive care unit (NICU) teams were poised to deliver and care for the baby as soon as the team gave the all clear. “Once we got Ashley on ECMO, things began to move very quickly,” Mason recalled.
After the cesarean section, the NICU team rushed the baby to the next room for treatment. Aside from needing a ventilator to aid his 29-week-old lungs, Ashley’s newborn son was otherwise healthy. At the time, the staff didn’t think about the historic nature of the moment, which marked BAMC’s first patient to give birth while on ECMO.
Ashley has no memory of her delivery and the days after were “extremely foggy,” she said. It all “snapped back to reality” when her nurses came in with a poster with her son’s updated height, weight, and hand and foot prints, and she became intent on getting well enough to hold her son.
Due to a 30-day isolation, Ashley was able to see her baby via video chat but didn’t meet him in person until weeks later. “It was heartbreaking,” she said. “I wanted to be with him, to hold him and feed him.”
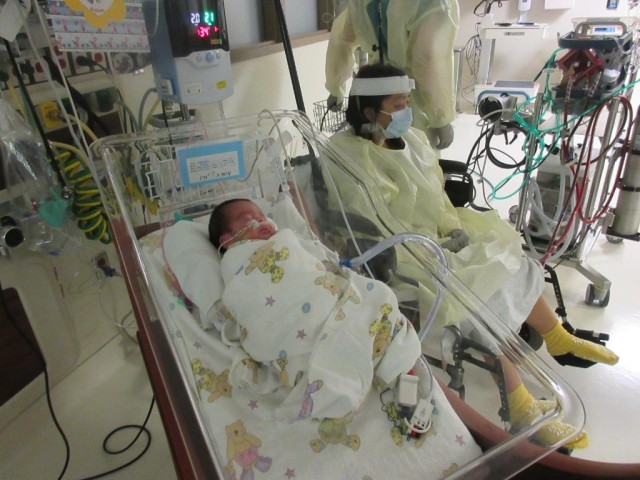
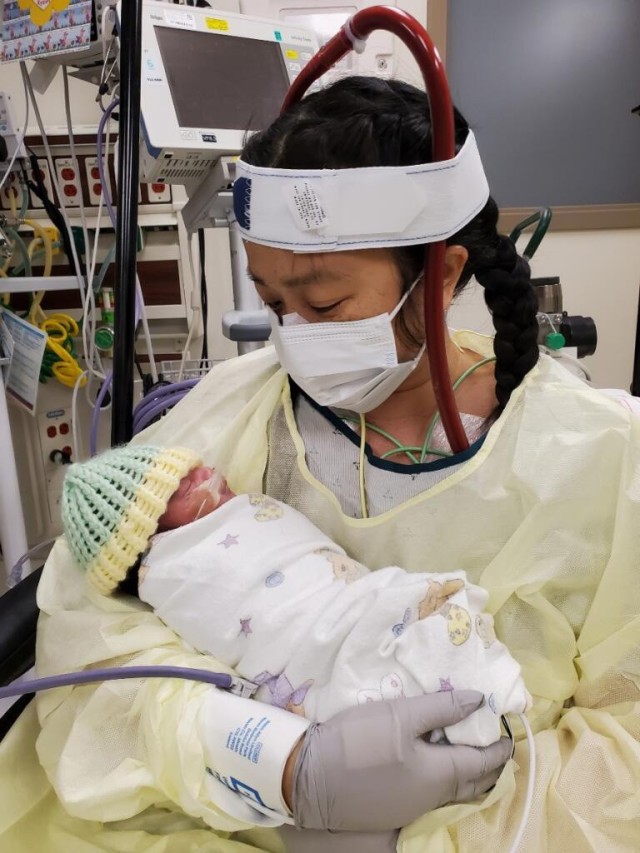
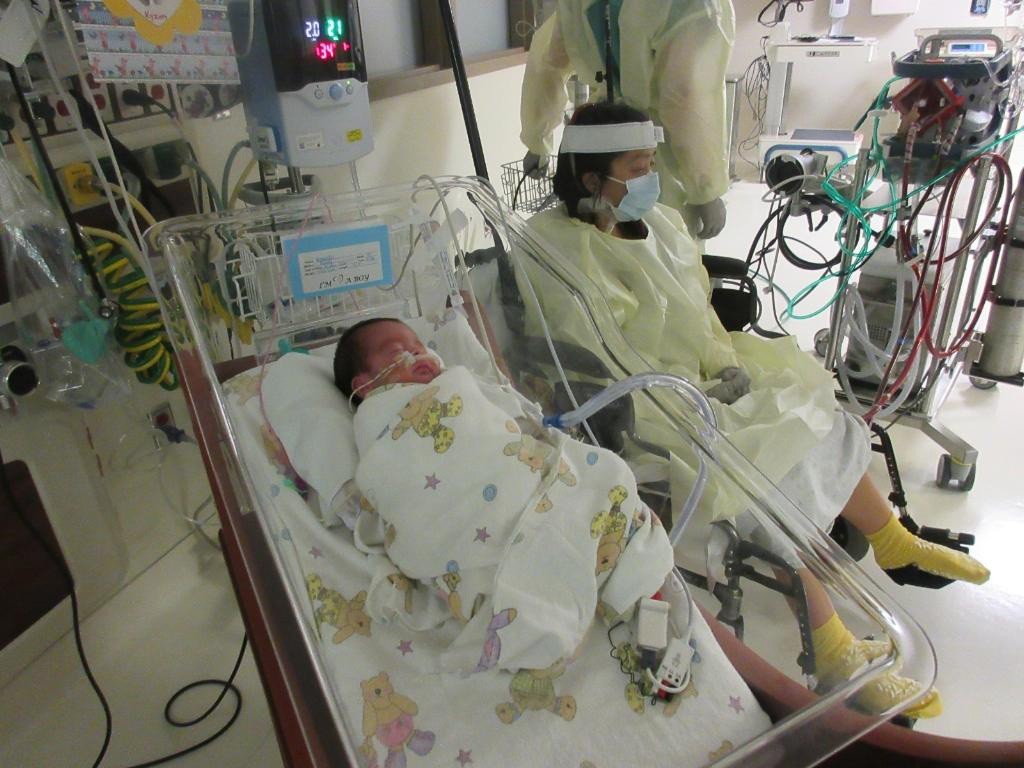
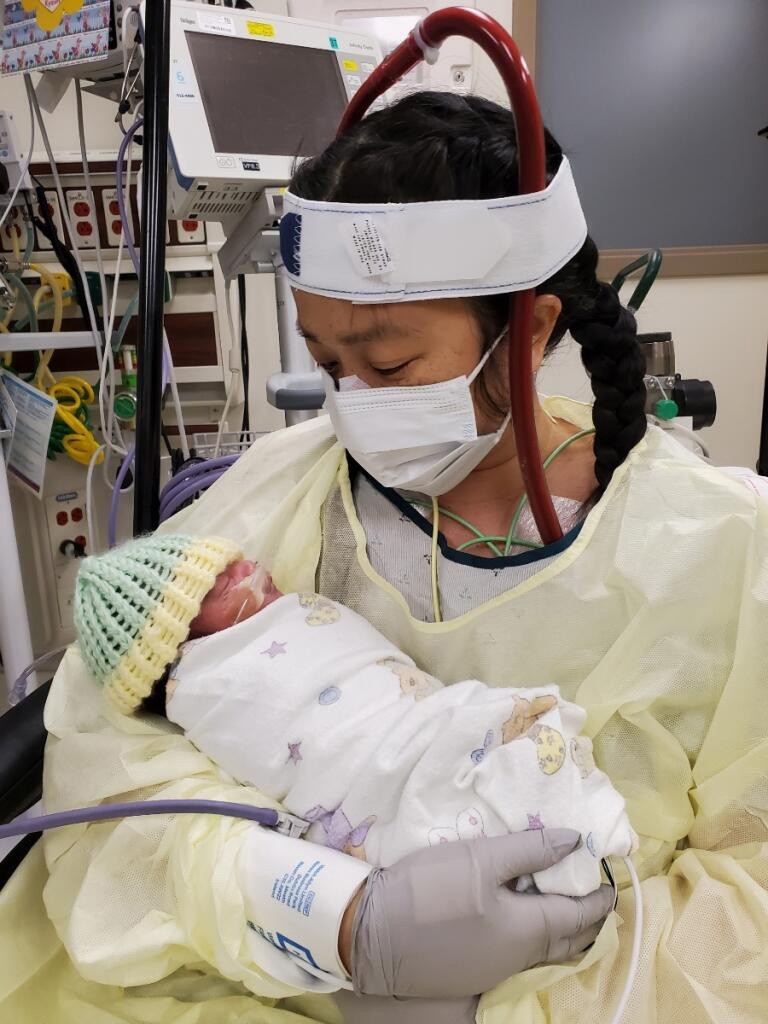
On July 17, Ashley was finally able to visit with her son in the NICU. Still on ECMO and fighting exhaustion, she sat in a room, donned in a gown and mask, and held her baby for the first time. “He felt very heavy and very small,” she said. “But I was so relieved to hold him.”
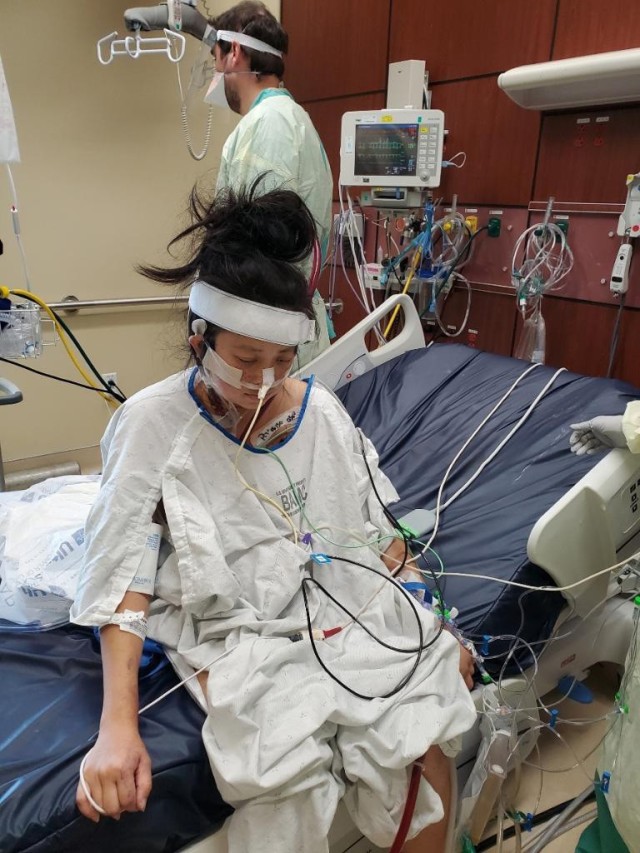
Ashley was on ECMO for 30 days, mostly while awake to help build her strength and stamina. But like many ECMO patients, she felt “horrible anxiety” and leaned heavily on her health care team for comfort. She especially relied on her nurses, Roxann Naud and U.S. Army Capt. E.J. Rauch, she said.
“She felt very overwhelmed,” Naud said. “She was very concerned about her baby in the NICU and her other children. We did our best to reassure her and let her know her feelings were very normal and okay; that she will get through this.”
Fortified by seeing her baby, Ashley’s condition began to improve. She was removed from ECMO on July 26 and cleared to return home a few weeks later. “I couldn’t wait to get home to see my husband and children,” she said.
Homecoming
Ashley’s husband drove her home from the hospital. As she slowly walked into her house with an oxygen tank, her normally rambunctious children – ages 7, 6, 4, 3 and 1-- were surprisingly calm. “I sat down and they didn’t leave my side for several days,” she said.
A few weeks later, Ashley and her husband welcomed their new baby, Kyzon, home. Now 5 months old, “he’s doing great – eating and sleeping and laughing,” she said.
About a month ago, Ashley had a checkup and received a clean bill of health. “I’m very grateful that God saw fit that I needed to still be here for some reason,” she said, holding Kyzon tightly on her lap. “I’m also extremely grateful to BAMC for the compassionate care.”
“It was an experience unlike we have ever faced, together or apart, but truly a miracle,” her husband added. “Only by God's grace and both the skill and care of the BAMC staff that my family is whole today.”
While ECMO was key, Mason also credits Ashley’s positive attitude and the hard-working team members who sat by her side, rubbing her temples and feet or brushing her hair when she felt anxious.
“We are absolutely thrilled to see Ashley doing so well,” he said. “It’s been a tough few years filled with heartbreaking loss and amazing survival stories. Ashley’s outcome is energizing for all of us.”
With COVID-19 transmission on the rise, Mason continues to encourage people to get the vaccine. “We have not had a fully vaccinated patient on ECMO or close to being on ECMO at BAMC,” he said. “It’s not too late; please get vaccinated.”



Social Sharing