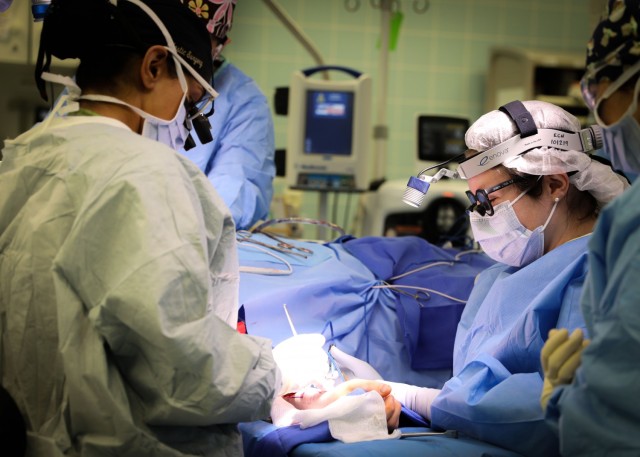
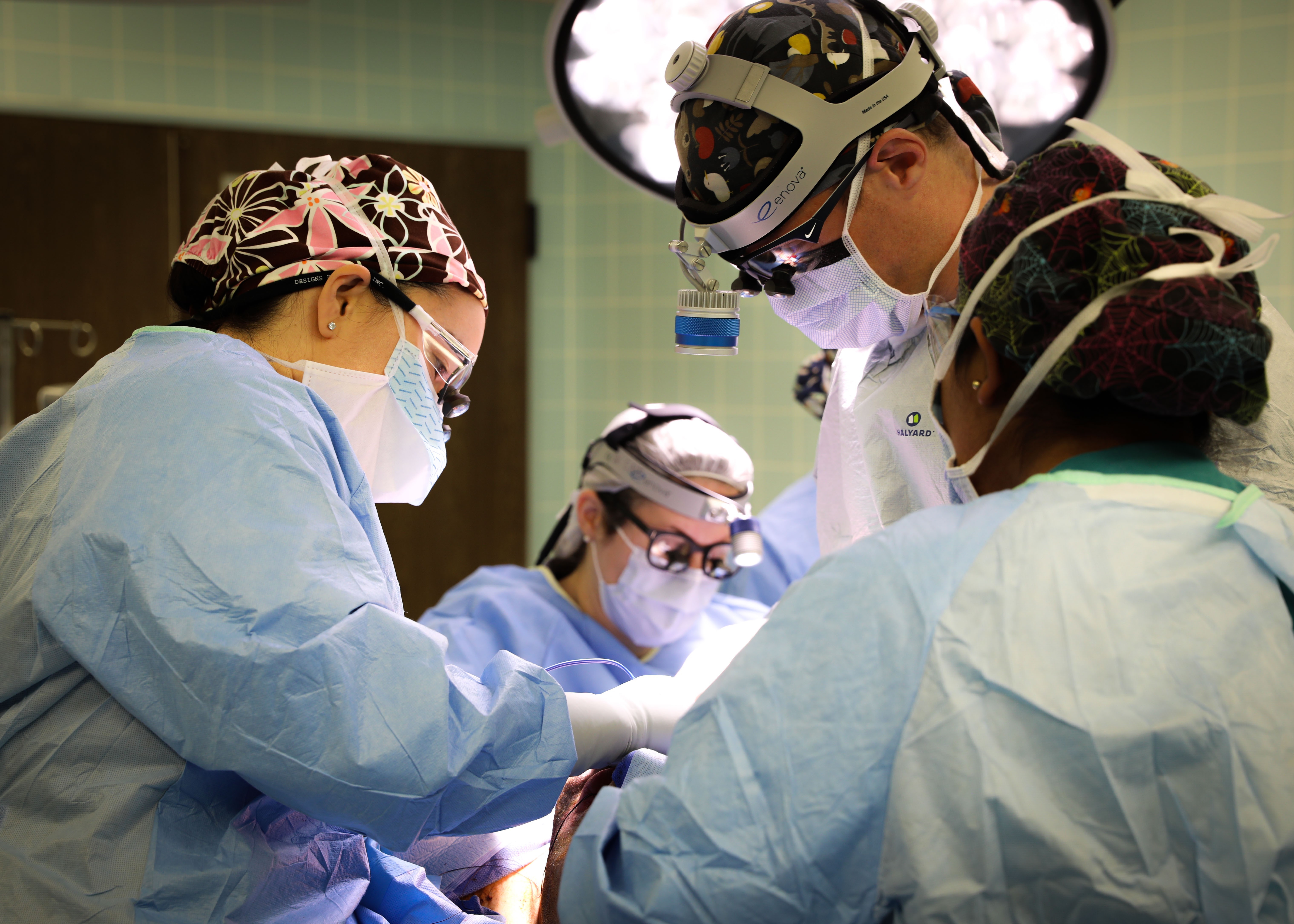
LANDSTUHL, Germany — U.S. Army Surgeons performed the first microvascular reconstruction and anastomosis procedure at Landstuhl Regional Medical Center, Dec. 3.
The first-of-its-kind procedure at LRMC expands services and capabilities at the only Level II Trauma Center outside the United States and principal evacuation and treatment center for all injured U.S. Service Members, civilians and Coalition Forces serving across Europe, Africa and the Middle East.
Microvascular anastomosis procedures involve the removal of soft-tissue defects followed by reconstructive techniques such as flap reconstruction where healthy, live tissue is moved from one part of the body to another. The procedure is effective in treating severe trauma and advanced diseases such as cancers, to maintain form and function.
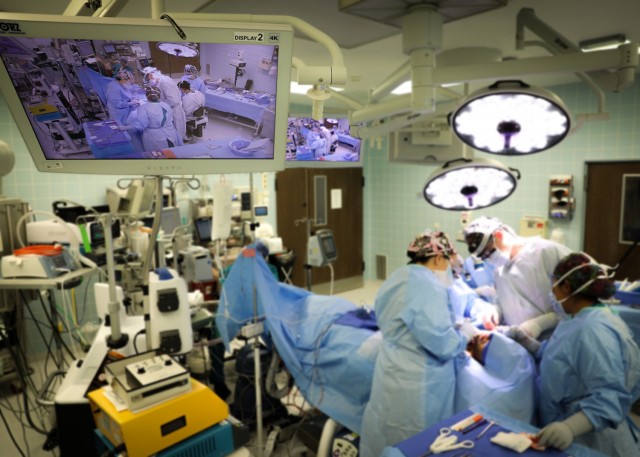
“We can take skin from someone's arm and attach it to vessels in the neck to reconstruct, for example, someone young, in order to allow them to have better functionality, better aesthetics and better overall quality of life after a major surgery that would otherwise leave them with some degree of disfigurement,” explains U.S. Army Lt. Col. Shimul Patel, chief, Plastic Surgery Services, LRMC. “This capability affects many of our beneficiaries here in Germany, ranging from active duty Service Members who may have devastating injuries to their limbs or other parts of their body that need tissue to our cancer population as well.”
During the inaugural procedure at LRMC, Patel and other surgeons operated on a patient with a type of head and neck cancer, successfully removing the tumor and applying free flap reconstruction to the resection.
“[The introduction of microvascular reconstruction] is exciting because it expands our capability to take care of cancer patients and patients who've had significant traumas,” said U.S. Army Lt. Col. Jessica Peck, a facial plastic surgeon and chief of LRMC’s Ear, Nose and Throat Clinic. “That ability to offer additional reconstructive options improves quality of life and, in the long term, maintains function and has better cosmetic outcomes.”
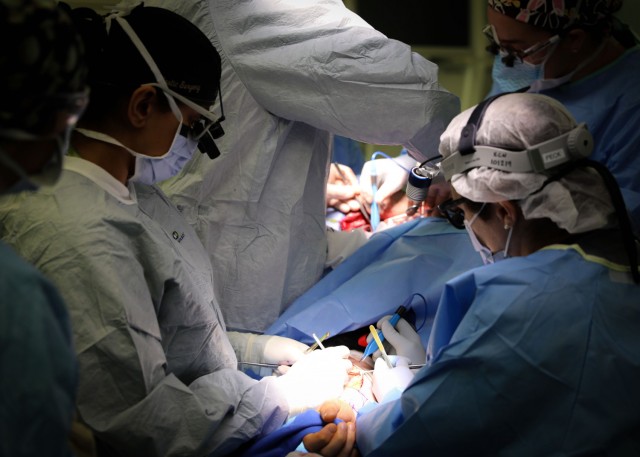
Peck, a native of Farmington, Utah, notes this is particularly significant for patients who suffer trauma or disease in visible areas such as the head or neck.
Although the technique has been practiced for decades, LRMC’s role has traditionally focused more on stabilizing and evacuating deployed trauma patients back to the Continental U.S. or their respective countries rather than reconstruction efforts.
“Our mission here is in support of all our forward (Combatant Commands) and receiving patients from those locations, stabilizing them and then offering them the opportunity to go back to (the U.S.),” explains Patel, a native of Laurel, Maryland. “With this capability here we can put them on their path to recovery in a more expedited manner and also allow them to have surgery done in the comfort of a place that speaks their native language.”
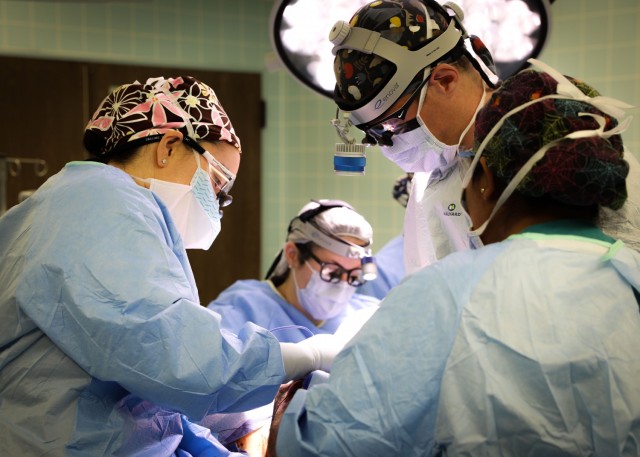
According to Peck, because the surgery is labor intensive, with some operations lasting 10-12 hours at a time, at least two specialty-trained surgeons are required for the operation which is rare at some Army Medical Treatment Facilities.
Both Peck and Patel are hopeful the introduction of the new procedure will not only help patients but also keep military surgeons, who are trained in the procedure, battlefield ready, while boosting talent acquisition efforts.
“To be able to continue offering those services and bring those services here enhances all of our readiness,” said Patel, a West Point alumna who completed plastic and reconstructive surgery training at Tulane University / Ochsner Clinic in New Orleans, Louisiana. “LRMC surgeons will have the opportunity to be able to continue to do what they've been trained to do while taking care of trauma and cancer patients.”



Social Sharing