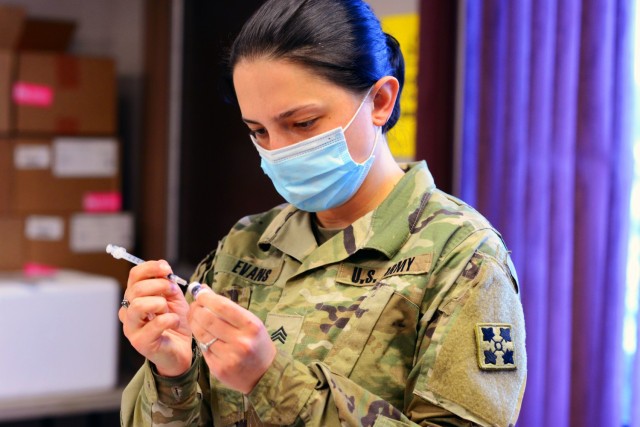
ABERDEEN PROVING GROUND, Md. — The recent death of former U.S. Secretary of State and retired Army Gen. Colin Powell of complications related to a COVID-19 breakthrough infection has led some to criticize the effectiveness of COVID-19 vaccinations. Powell, who was 84 years old, was also immunocompromised due to multiple myeloma, a blood cancer that studies show can make the vaccine shots less effective.
“Saying ‘vaccines don’t work’ is like saying ‘seat belts don’t work’,” said Dr. John Ambrose, Army Public Health Center senior advisor for Clinical Public Health & Epidemiology. “Car accidents are a risk despite any individual’s best efforts. However, by wearing a seatbelt, an individual is far more likely to survive if in an accident.”
Ambrose says getting vaccinated is like wearing body armor.
“Vaccines strengthen the body’s immune response to a particular pathogen,” said Ambrose. “When the body’s immune system needs to fight pathogens, having a vaccine is like having body armor. I don’t know of a Soldier that would prefer to be without body armor when heading into a battle.”
Sometimes the reporting around breakthrough infections can create a perception that the COVID-19 vaccines are not effective, but this is far from the case. Unvaccinated individuals are at a far greater risk of hospitalization and death than those who have been vaccinated, said Ambrose.
“When comparing the clinical outcomes of SARS-CoV-2 infection between fully vaccinated and unvaccinated individuals, the data are clear,” said Ambrose. “Unvaccinated individuals are far more likely to both test positive and to die due to infection when compared to fully vaccinated individuals of similar ages.”
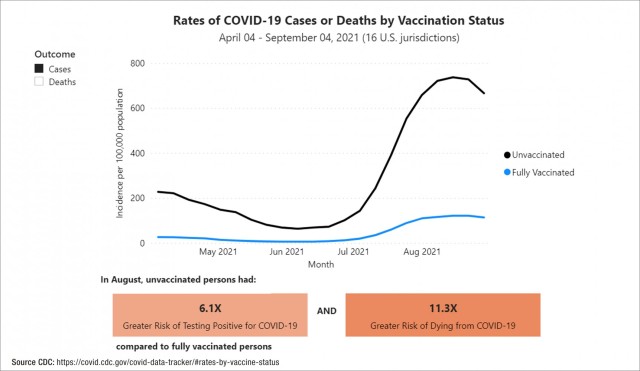
Ambrose explains the data have been consistent throughout the pandemic, but the relative risk of being unvaccinated (compared to fully vaccinated) was especially pronounced in August 2021, where unvaccinated individuals (compared to fully vaccinated) were:
- 6.1x greater risk of testing positive
- 11.3x greater risk of dying from COVID-19
This is illustrated in a chart shared by the Centers for Disease Control and Prevention that tracks case and death rates by vaccination status. The chart below [Figure 1] shows only cases, but charts for both cases and deaths are available from the CDC.
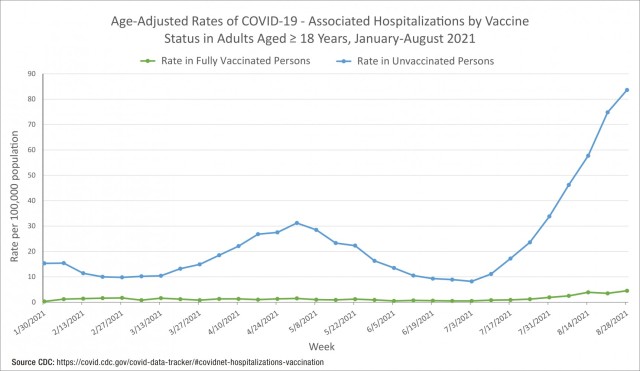
The CDC also tracks age-adjusted rates of COVID-19-associated hospitalizations with respect to vaccination status [see Figure 2]. The blue line in the chart shows hospitalization rates per 100,000 for unvaccinated individuals 18 years old and above and the green line shows the hospitalization rates for vaccinated individuals in the same age group. This chart tracked hospitalization rates from January to August 2021. Unvaccinated individuals were hospitalized at a rate of nearly 85 percent vs. about 5 percent for vaccinated individuals.
“The bottom line is that unvaccinated individuals are at significantly greater risk – and this is true for infection, hospitalization, and death,” said Ambrose.
Ambrose said vaccines for SARS-CoV-2 remain an effective measure to prevent severe cases of COVID-19. While the vaccines may not prevent all cases of disease, they are very effective in preventing severe cases of diseases. No vaccine is 100 percent effective – this means that some breakthrough cases of SARS-CoV-2 infection will occur despite being fully vaccinated.
“The vaccine will still greatly reduce the clinical impact of the infection,” said Ambrose. “Breakthrough cases resulting in hospitalization or death are quite rare, even among elderly individuals who are fully vaccinated.”
The first and most important thing immunocompromised individuals can do to reduce their risk is to get fully vaccinated, said Ambrose. Additional mitigation efforts to decrease risk to immunocompromised individuals have largely remained the same throughout the pandemic:
- All immunocompromised individuals should make reasonable efforts to avoid unnecessary prolonged contact with other unvaccinated (or potentially unvaccinated) individuals.
- Always wear a mask that covers your nose and face when visiting public places or coming into contact with others.
- Ensure others that you come into contact with on a regular basis are vaccinated.
- Try to maintain at least six feet of distance between you and other individuals if you have to go into a public or social setting.
- If hesitant about vaccination, discuss the risks and benefits of the vaccine and booster shots with a medical provider that you trust.
When interacting with people who are immunocompromised, there are a number of things people can do to reduce the risk, said Ambrose. First, try to avoid close contact (i.e. within 6 feet) with immunocompromised individuals unless they live in your household. If that is not an option, limit face to face contact with them to a minimal amount of time and attempt to stay at least six feet apart during the conversation. If you are experiencing any upper respiratory symptoms, any contact with immunocompromised individuals should be strictly avoided (even if individuals are within the same household).
Another topic of discussion that has invited criticism or misinformation is around vaccine boosters. The critics say if the vaccine is effective, then why is there a need for a booster?
A vaccine booster restores the effectiveness of the original vaccine, which can decrease over time, said Ambrose. A recent Lancet article evaluated the effectiveness of the BNT 162b2 (Pfizer-BioNTech) vaccine, and the data indicated that effectiveness (for preventing hospitalization) was high (93 percent) for all ages for up to six months. At that time, certain groups at higher risk (e.g. older age groups) may significantly benefit from a booster.
Ambrose also explained the distinction between a “third dose” and a “booster”. He referenced a recent article on Yale Medicine’s page which explains it nicely.
- Doctors use the term third dose when referring to people with compromised immune systems who may not have gotten the level of protection they need from the first two doses. The third dose provides that level of immunity.
- A booster shot is recommended due to concern that the effectiveness of the vaccine decreases over time and may not protect against a new strain, such as Delta. A booster may be given to older people or those with chronic medical conditions or other risk factors. In other words, a booster restores the effectiveness of the vaccine.

The CDC maintains a continuously updated website tracking cases of COVID-19 breakthrough hospitalizations and deaths. Ambrose says the majority of “clinically significant” breakthrough cases, defined here as cases resulting in hospitalization and/or death, occur in individuals over 65 years of age.
APHC also maintains a searchable COVID-19 page containing a wealth of information about the virus.
The U.S. Army Public Health Center enhances Army readiness by identifying and assessing current and emerging health threats, developing and communicating public health solutions, and assuring the quality and effectiveness of the Army’s Public Health Enterprise.




Social Sharing