FORT BENNING, GA – A critically ill patient gets admitted to the intensive care unit. Do you know how to stabilize the patient? Saving his or her life may require mechanical ventilation, a central line or a chest tube. What if you are deployed? Same situation, severely injured person, fewer resources. Remember, every second counts.
Last week, Brooke Army Medical Center’s (BAMC) Critical Care Team spent three days refreshing those life-saving procedures for Martin Army Community Hospital’s (BMACH) residents and staff. It’s the first time the physicians from Fort Sam Houston combined Fundamental Critical Care Support (FCCS) skills with Individual Critical Task List (ICTL) skills in one course.
“The goal is to empower the physicians to be comfortable with critically ill patients [who get] admitted and require management while they get stabilized and/or transferred,” said BAMC Simulation Center Chief Maj. John Hunninghake. ”We developed the course for primary care physicians who might deploy as intensivists [physicians who specialize in the care of critically ill patients].”
After two days of lectures and hands-on skills refreshers, BMACH physicians got to validate their ICTL skills on the third day. Residents and staff performed various emergency procedures under the watchful eye of the BAMC Critical Care Team.
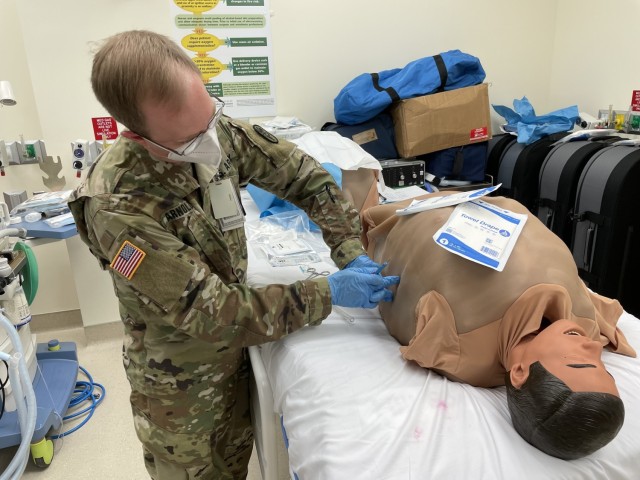
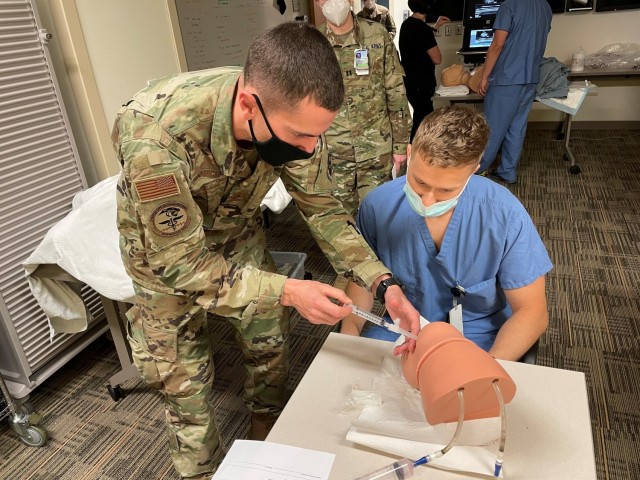
“Airway intubation are for patients who are unable to breathe on their own,” explained Pulmonary and Critical Care Medicine Chief Lt. Col Robert Walter. “The breathing tube is always the preferred mechanism because it’s the least traumatic. We use the surgical airway (cricothyroidotomy) only if we are unable to secure an airway through the traditional ET (endotracheal) tube.”
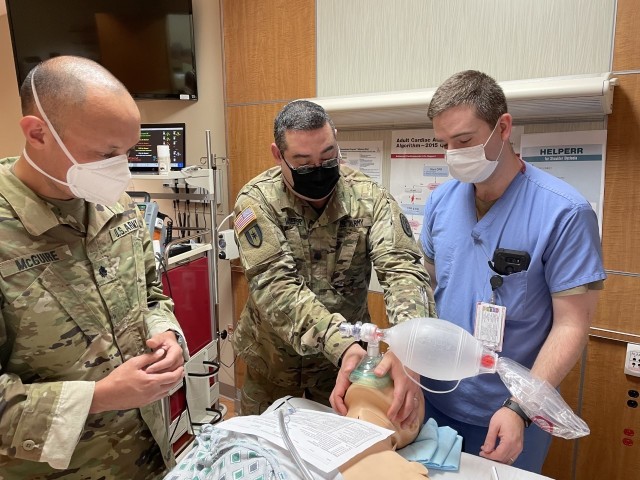
Walter walked the BMACH team through intubation, starting with tips on pre-oxygenating the patient with a bag valve mask (BVM).
“Using your fingers to go behind the mandible and pull the face into the mask while pressing down with your thumbs will get you a good seal,” shared Walter. “But be careful how far those fingers go toward the midline. People have a tendency to overreach, especially on smaller people and that will actually pinch their airway a bit so you have to really stay at the edge.”
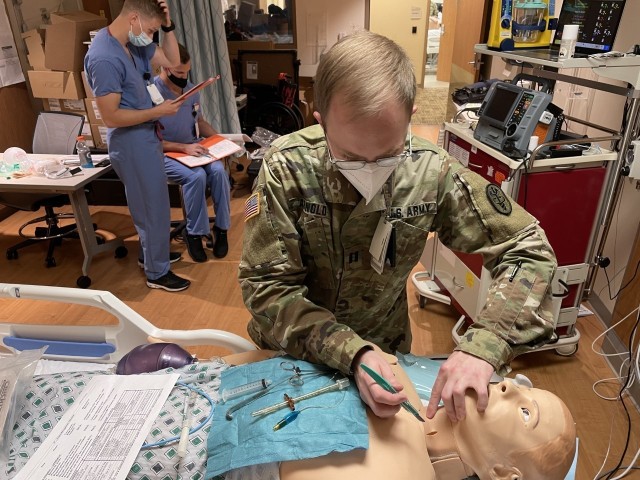
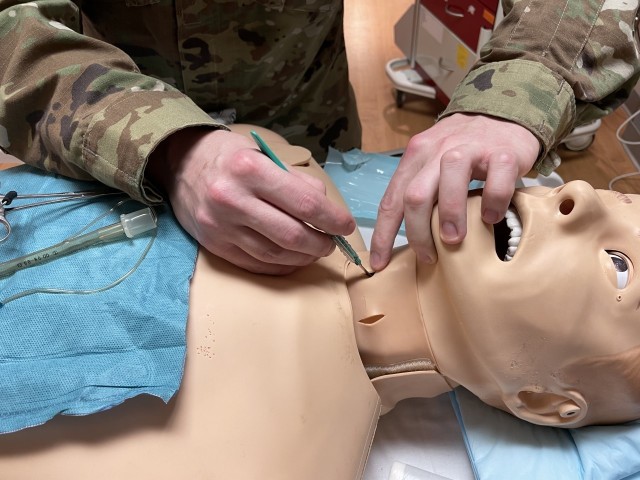
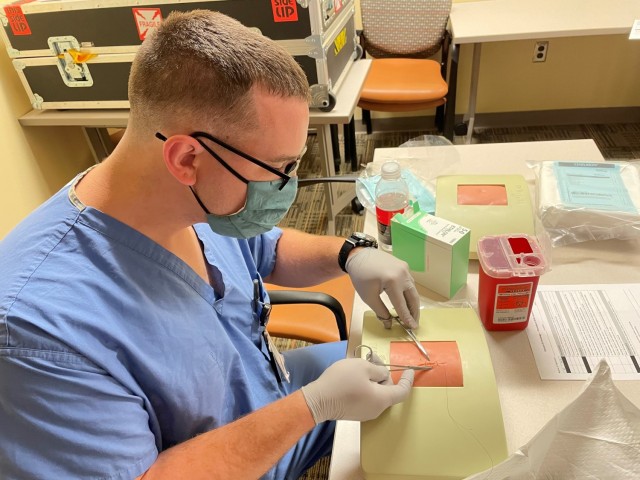
The San Antonio Pulmonary Chief said the most difficult part of intubation is being able to visualize the larynx to make sure you pass the tube through the vocal chords and into the main airway, and not into the esophagus. If the patient has facial trauma that prevents you from placing a breathing tube, that’s when you resort to a cricothyroidotomy.
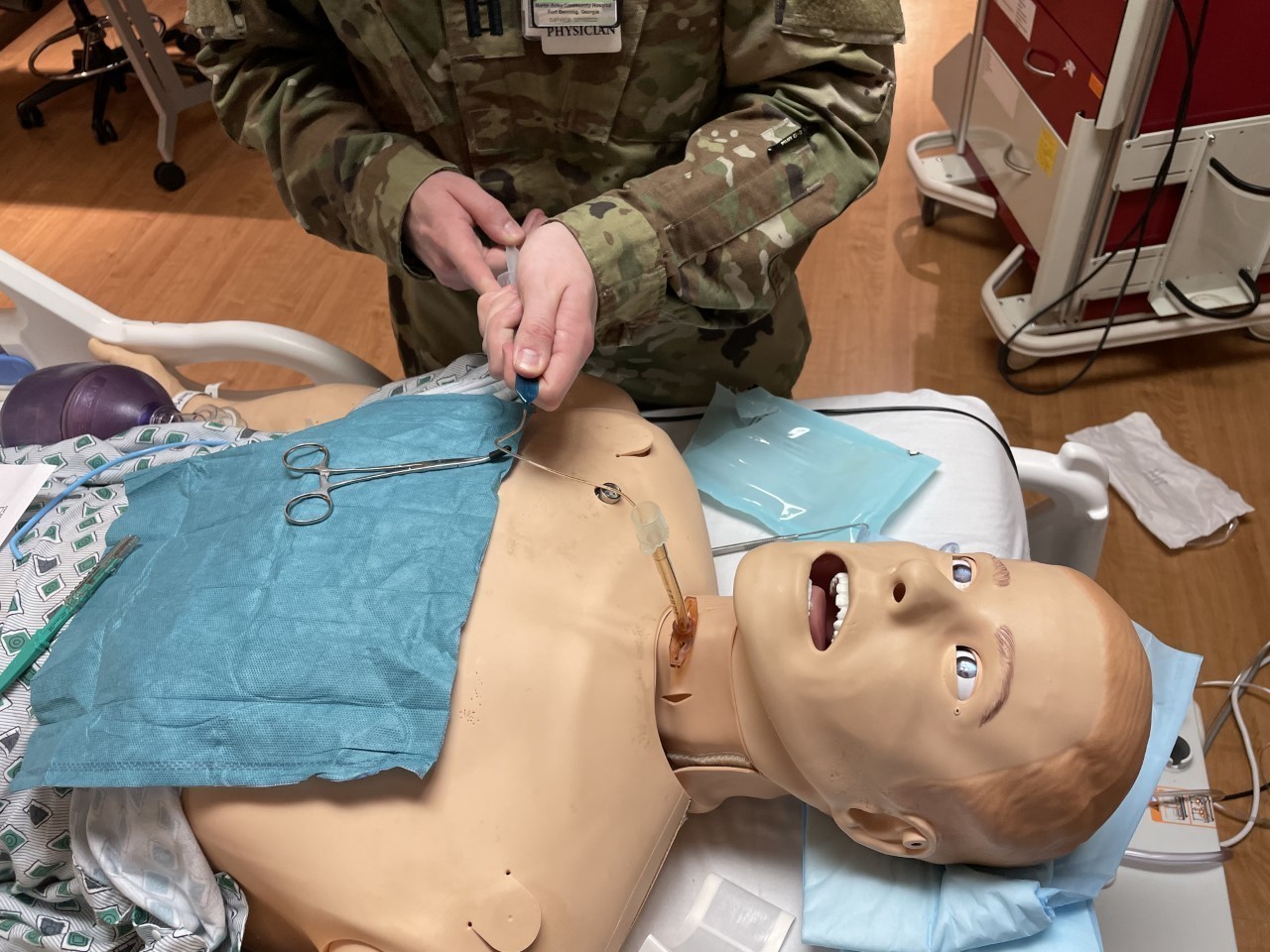
“We’re making an incision through the neck and through the membrane between the cartilage that constructs our main airway called the trachea, and then inserting the breathing tube to be able to breathe for them,” said Walter. “This will be the immediate procedure that’s done. It’s then revised usually by a trauma surgeon or someone who is a little bit more deft at doing what we just did to make sure it’s a long term solution.”
Instead of oxygen, sometimes patients are in dire need of medication or fluids. That’s when you would place a central line.
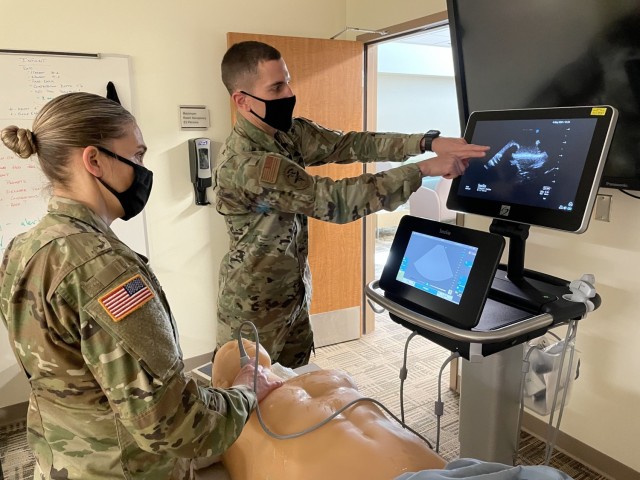
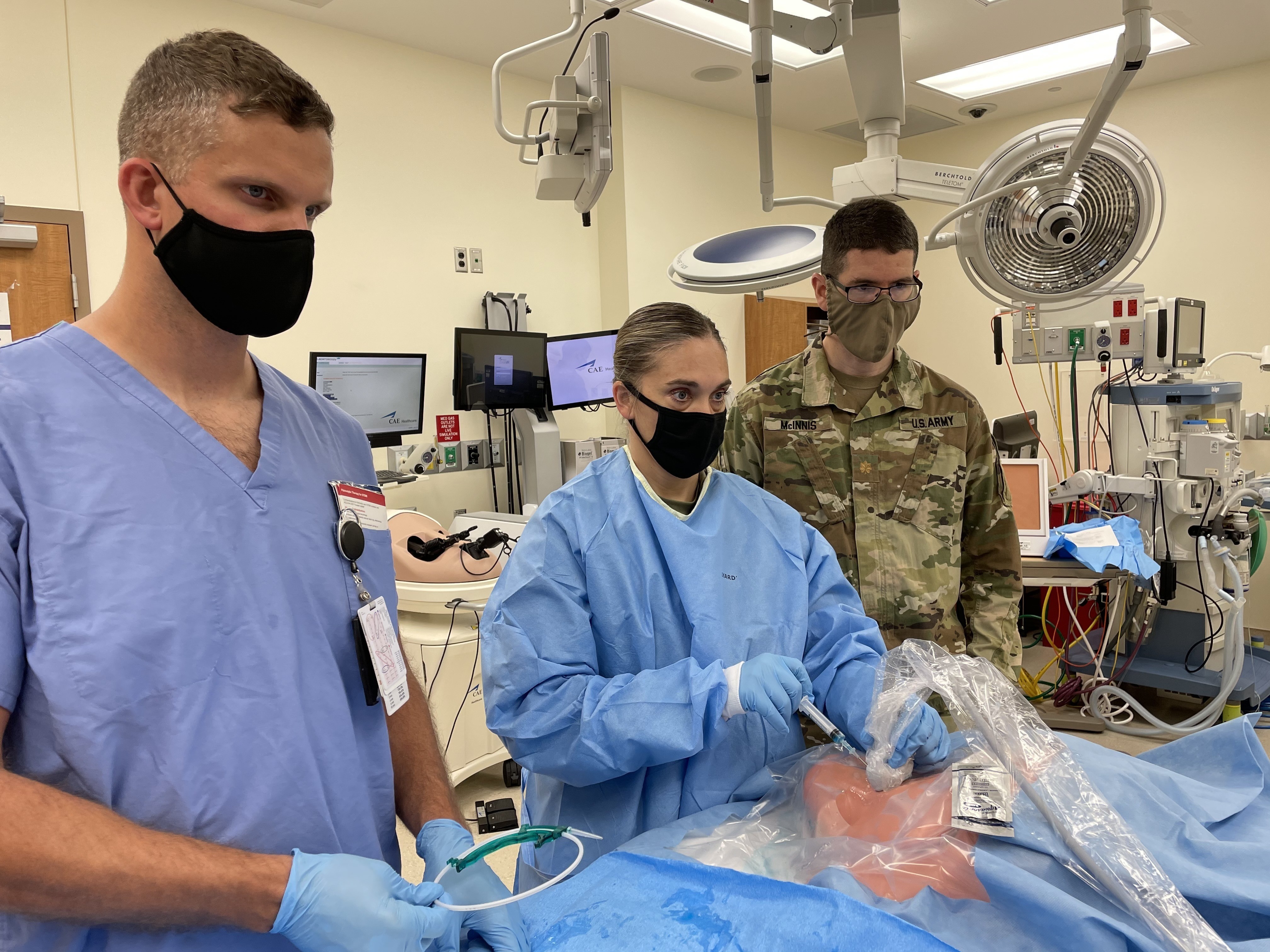
“Central lines are commonly placed in the internal jugular vein, the subclavian vein and the femoral vein to obtain vascular access to the deep veins of the neck, the groin, etc,” explained Pulmonary and Critical Care Medicine Physician Maj. Ian McInnis. “Entering the vein if it’s very collapsible because they are dehydrated can be technically challenging.”
BMACH 3rd year resident Maj. Shelley Flores demonstrated what she learned by placing a central line aided by an ultrasound, starting with an important safety step.
“We gave lidocaine because you don’t want to stick them with this big needle and then they jerk back and you end up stabbing yourself,” said Flores. “Central line actually goes into the SVC (superior vena cava) on the side of the heart, so [medications] get into the patient faster as opposed to peripheral where it’s in the arm, the hand, the foot. Some medications can feel like they burn when they go through a peripheral IV like potassium.”
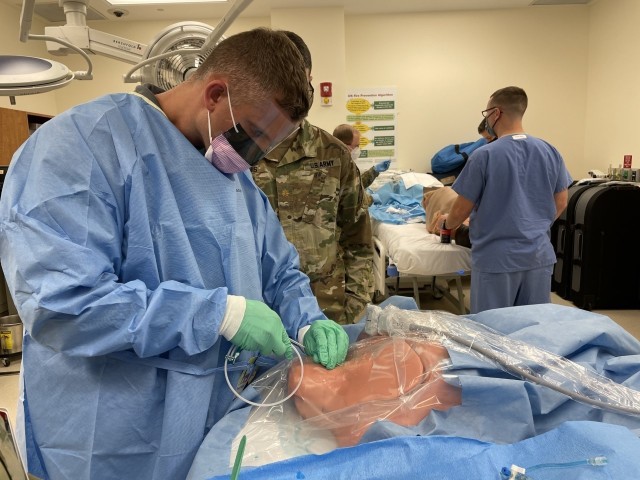
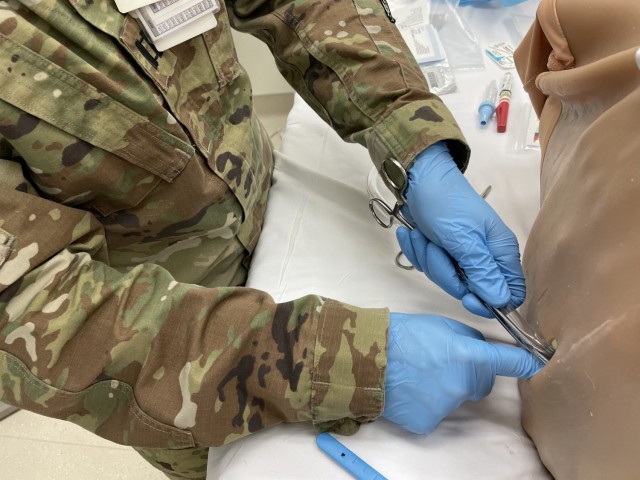
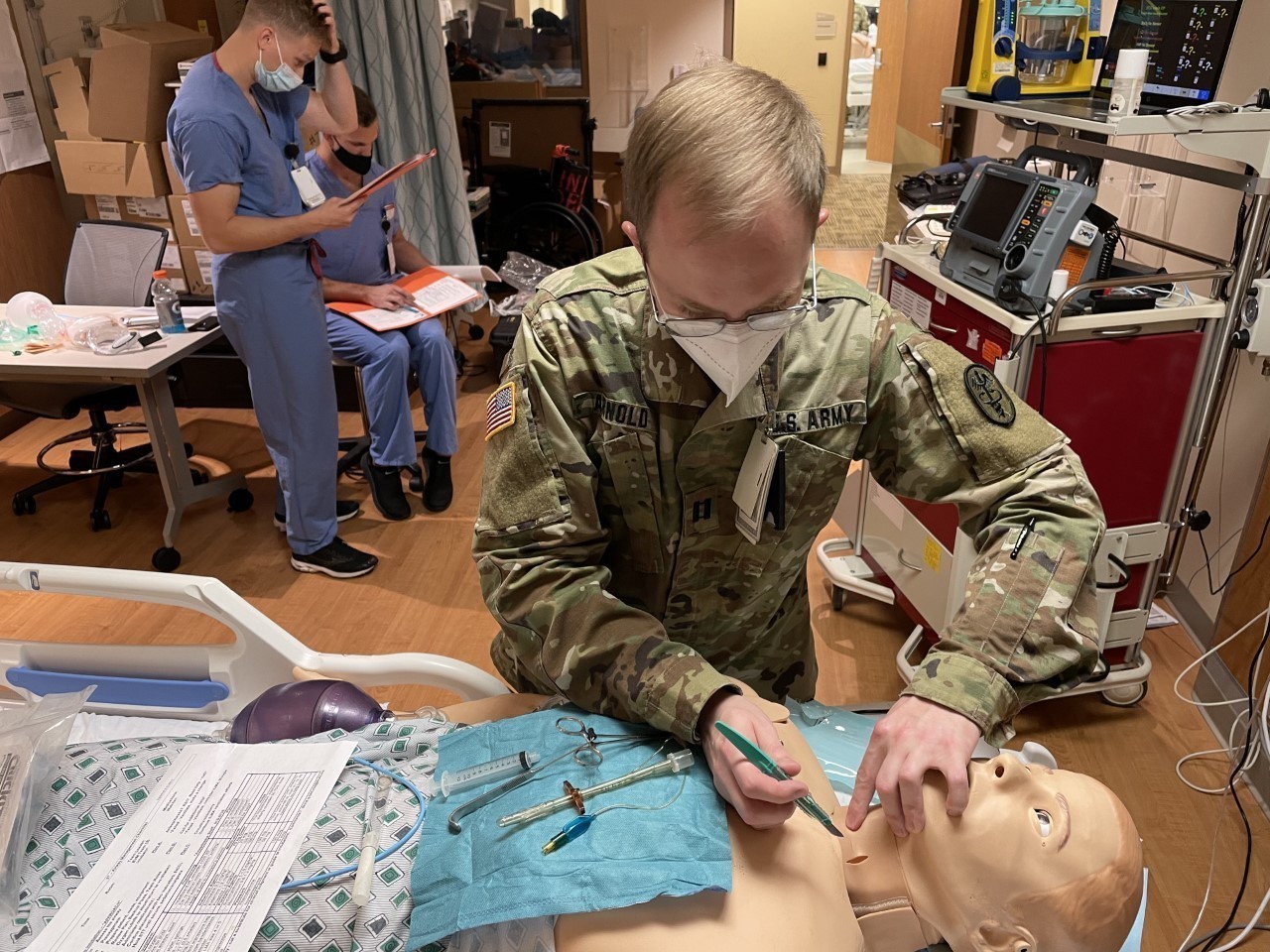
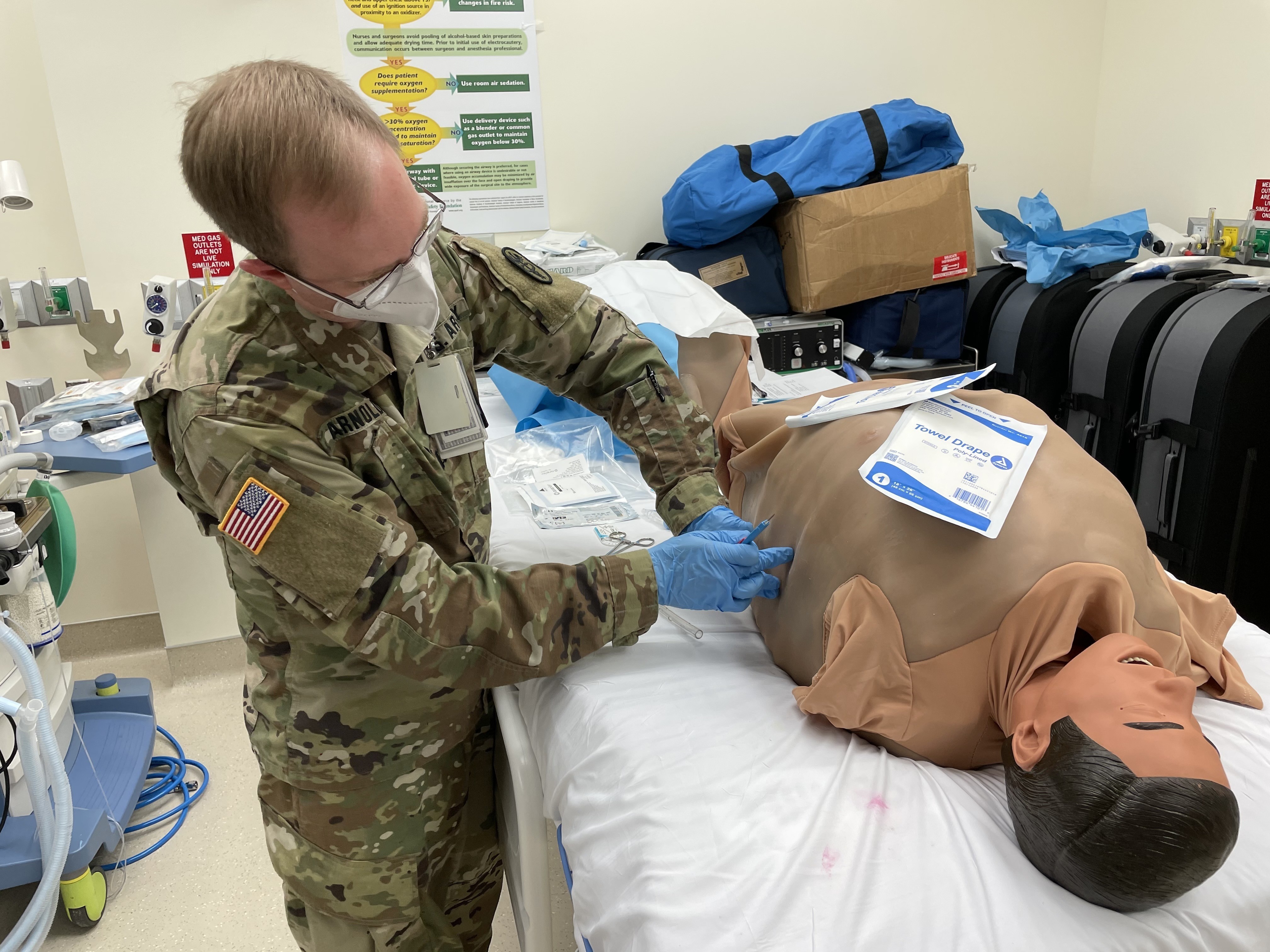
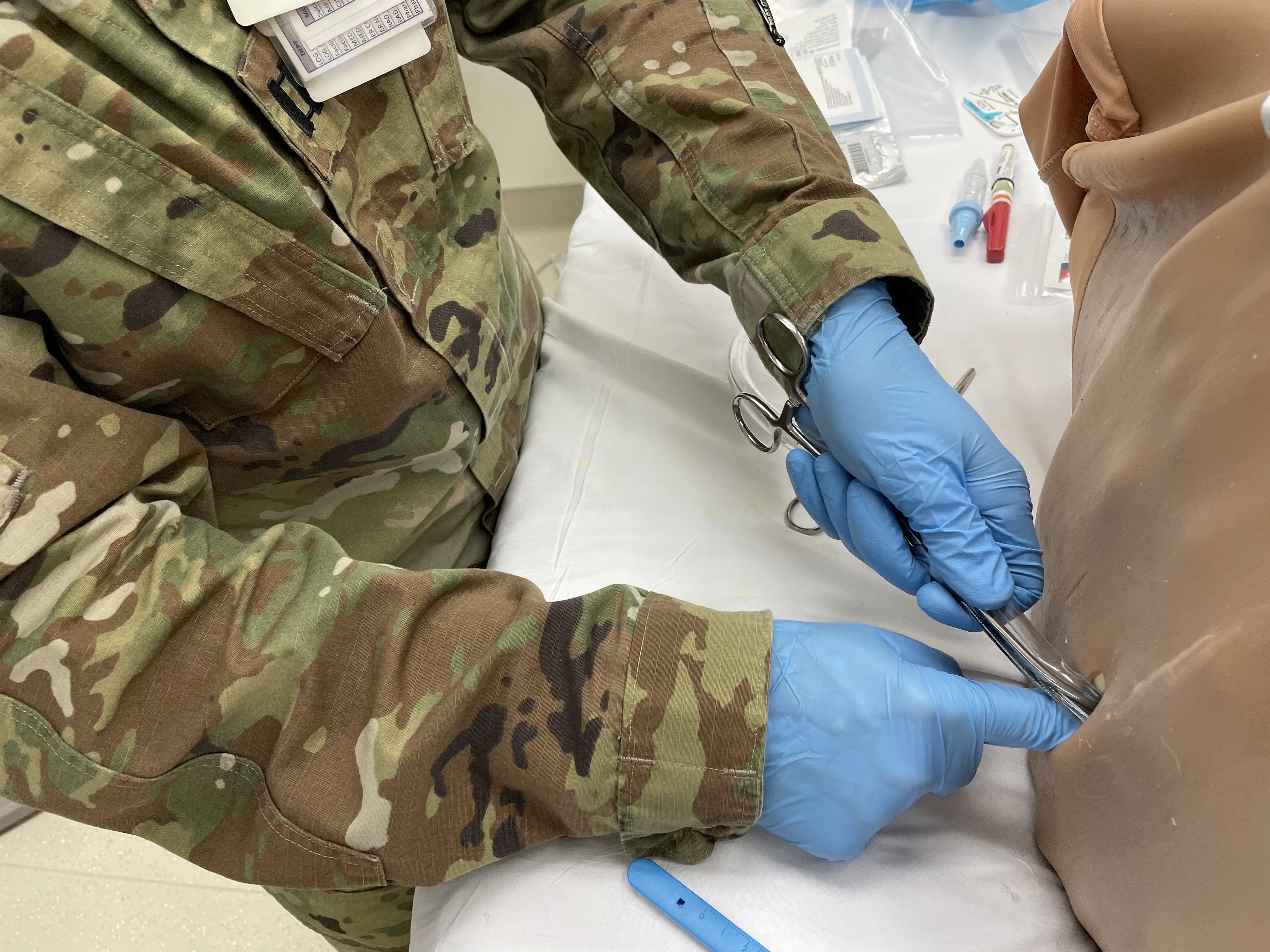
Proving that learning never ends, BMACH ER Physician Capt. Jacob Arnold demonstrated his mastery of chest tube (tube thoracostomy) and needle D (decompression) insertion, with feedback from BAMC’s Maj. Michael Sobieszczyk. Arnold had just last month taught BMACH’s graduating residents those very same ICTL skills.
“Sometimes you can take those curved Kellys (clamps) and use them to your advantage by kind of twisting up,” suggested Sobieszczyk. “That will thread the chest tube toward the apex. It might help the positioning.”










Social Sharing