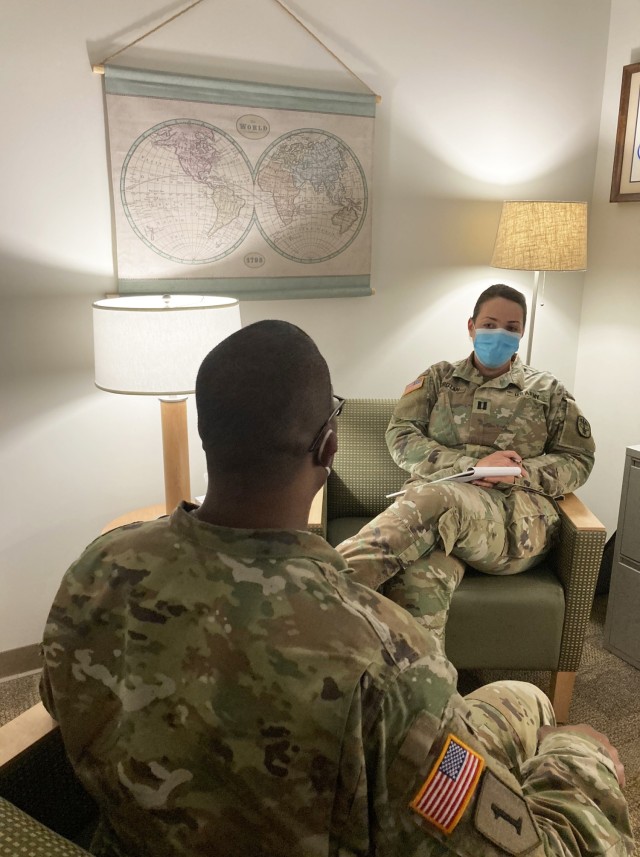
FORT CAMPBELL, Ky. – The consequences of binge drinking can reach far beyond a nasty, next-day hangover. It can cost those who overindulge self-control, relationships, careers and health.
“You run the risk of dying through excessive use of alcohol,” said Georgina Gould, clinical director of the Substance Use Disorder Clinical Care, or SUDCC, at Blanchfield Army Community Hospital. “Your body can only take so much.”
April is National Alcohol Awareness Month and SUDCC clinicians are partnering with the Fort Campbell Alcohol Substance Abuse Program, or ASAP, to highlight the risks and tolls of binge drinking, ways to make healthier choices and programs available to those who need help.
Gould said the National Institute on Alcohol Abuse and Alcoholism defines binge drinking as pattern of consuming alcohol that raises blood alcohol concentration to 0.08% or higher. For average adults, that pattern corresponds to consuming five or more drinks a day, for men, or four or more drinks for women over the course of about two hours.
Heavy alcohol use – defined as more than four drinks in one day for men or three drinks in one day for women – builds tolerance that can increase an individual’s risk of developing an alcohol use disorder. Women who consume more than seven drinks per week and men who take in more than 14 drinks per week run a higher risk than those who limit their intake, Gould said.
“Is there are a magical combination or pattern that you’re supposed to find? I think you’re supposed to have enough self-awareness to be able to be in tune with your body to understand why you’re using alcohol and what your pattern looks like,” Gould said. “I always tell Soldiers, challenge yourself for two weeks not to use any alcohol. If you find that challenging, then you may consider taking a pause and finding out why that is.”
Soldiers may find they are self-medicating to avoid other problems, whether it’s post-traumatic stress disorder, depression, isolation or boredom. They also may be surprised by how much time is spent procuring and consuming alcohol while neglecting activities that don’t involve alcohol, she said.
Measured approach
There are ways to reduce the chance of becoming dependent on alcohol or suffering alcohol poisoning, and that starts with keeping track of how much alcohol one consumes, Gould said.
“When you’re really analyzing how much someone is drinking, in terms of standard drinks, they may not know themselves, because they may just be pouring alcohol into a large cup,” she said. “We really try to increase awareness about how much the body is taking in and how the body processes alcohol.”
Binge drinking is often associated with young adults, who may not yet understand how their bodies will react to alcohol or know their limits, Gould said. Binge drinkers don’t have to drink daily to develop a drinking disorder and may not even realize their drinking is excessive, especially if they are not keeping up with drinks they had before going out.
“There is a myth that someone who is suffering from alcohol dependence lives under a bridge, with a grocery cart,” she said. “You can drink twice a month, and drink 22 to 25 standard drinks, but you’re still venturing toward an alcohol use disorder of some sort. This relates to your tolerance of alcohol, which is one of the criteria for alcohol use disorder.”
When the body absorbs so many toxins, there will be short- and long-term effects, Gould said.
“They are not very glamorous,” she said. “Pancreatitis, brain fog, muddy thinking. Then it starts bleeding into other parts of their lives, whether it is smelling like alcohol in formation or getting a DUI because their judgement lapsed from using alcohol.”
Women are more susceptible because their bodies process alcohol differently and the effects hit them faster, Gould said. Knowing and understanding that may help some make better decisions.
Alcohol impairment can lead to poor decision-making, increase the likelihood of being victimized or victimizing someone else, and keep drinkers from seeing reality clearly, she said. Those who have been drinking for many years and seek out help are often surprised by how their thinking changes after they sober up.
Seeking treatment
“After they have received treatment and are in recovery with six months of sobriety, they can’t believe how much they have been ignoring in life,” Gould said. “This clarity comes over them, to see the alcohol was really a coping mechanism for them.”
BACH offers primary outpatient care, outpatient services, and individual and group counseling to ad-dress concerns about alcohol use, educate Soldiers and help them find the resources they need to heal, she said. They also can help concerned spouses find the resources they need to stay healthy by partnering with other agencies on post, including Army Community Service.
In 2018, a voluntary self-referral program was launched so Soldiers who want help can get treatment without their command having to know.
Soldiers also can be referred to treatment by their command, often after a bad incident. Most people have an internal switch that flips when too much alcohol is consumed and the body tries to eject the toxins, Gould said.
“If you have drank so much that the switch cannot be turned on and you pass out in bed, a parking lot, your car – you run the risk of dying,” she said. “The BACH emergency room has seen the acute dangers. They’ll show up at the emergency room having to have some form of charcoal treatment to get toxins out of their bodies.”
Alcohol dependence can also jeopardize others, even when a Soldier is not drinking, because of the impact of alcohol withdrawal. For chronic abusers, it can even be fatal to quit without medical help. That dramatically impacts the readiness of any Soldier, Gould said.
Social Sharing