ABERDEEN PROVING GROUND, Md. – As part of National Sleep Awareness Week, held March 14-20, the U.S. Army Public Health Center is reminding the Army Family of the benefits of quality sleep and the importance of seeking help if they have trouble sleeping or suspect they may have a health condition that is preventing them from sleeping well.
Sleep disorders may have immediate adverse impacts on physical and mental military readiness due to their influence on weight problems, injury risk, and visual and mental acuity.
Sleep disorders are health conditions that disturb normal sleep patterns. Although there are more than 80 different sleep disorders, the Army regularly assesses the following five conditions:
- Sleep apnea – a breathing disorder in which one stops breathing for 10 seconds or more during sleep, often several times throughout the night
- Insomnia – a condition of being unable to fall asleep and stay asleep. This diagnosis is given when a person routinely experiences this problem.
- Hypersomnia – a condition in which one is excessively sleepy and unable to stay awake during the day. Often individuals have trouble waking right away
- Narcolepsy – sometimes associated with hypersomnia, narcolepsy is a separate diagnosis that is associated with daytime sleeping. Unlike Hypersomnia patients, those with narcolepsy may feel refreshed after their unplanned nap.
- Circadian rhythm disorders – problems with the sleep-wake cycle. They make a person unable to sleep and wake at the right times.
According to the most recent Army Health of the Force report, also referred to as the HOF, 14 percent of active-duty Soldiers had at least one of these sleep disorder diagnoses. Many Soldiers experienced more than one of the conditions. The HOF notes that diagnoses such as insomnia have been associated with anxiety, depression, post-traumatic stress syndrome, chronic pain, alcohol abuse, and even suicide. The report also showed that sleep apnea and insomnia made up more than 50 percent of all the diagnosed sleep disorders among Soldiers.
The HOF report notes sleep apnea diagnoses were mostly for what is called “obstructive sleep apnea,” a disorder that is linked to being overweight or obese. Male Soldiers were diagnosed with sleep apnea two times as often as female Soldiers.
Insomnia, in contrast to sleep apnea, was diagnosed among female Soldiers over 1.5 times more frequently than male Soldiers, according to the HOF report.
Even Soldiers who are not diagnosed with a sleep disorder may get inadequate or poor quality sleep that prevents them from being at their physical and mental best.
According to the HOF report, a third of Soldiers did not get at least 7-8 hours of sleep for optimal health (7 – 9 hours is now recommended). The report indicates that Soldiers who get only 4-6 hours may experience a 10-15 percent degradation in their performance.
As a Soldier, training and deployment situations can make it difficult to maintain a regular sleep schedule and find a quiet, dark and comfortable sleep environment. Sleep can become a low priority – and getting by with little to no sleep may even be considered a ‘badge of honor.’ But better sleep means more resilient Soldiers.
Soldiers and leaders should recognize the benefits and strive for good sleep by considering the following:
- PLANNING. Factor adequate sleep time into training schedules and identify means to improve sleep environment
- TACTICAL NAPPING. During sustained operations, take advantage of short opportunities for napping (20 minutes or less) until longer sleep period opportunities
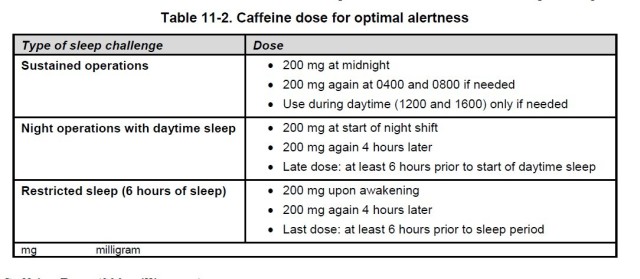
- CAFFEINE OPTIMIZATION. Follow caffeine dose for optimal alertness outlined in Army Field Manual 7-22, Holistic Health and Fitness, to temporarily boost alertness during sustained operations, but avoid caffeine approximately six hours prior to sleep.
- SLEEP BANKING. When sleep loss is unavoidable, “bank” sleep ahead of time by sleeping more than usual since sleep loss has compounding, cumulative effects.
- SLEEP ENVIRONMENT. Reduce ambient noises and light, maintain a cool temperature, and sleep on a comfortable surface.
- SLEEPING BEHAVIORS Avoid bright and blue lights (turn off TVs and electronics), exercising to exhaustion, consuming heavy meals, taking certain medications, and consuming caffeine and/or alcohol close to sleep time. Get bright light as soon as possible in the morning.
- MEDICAL SUPPORT: If you think you may have a sleeping disorder, seek the advice of a medical provider.
For more information:
- Army’s 2019 HOF report, (pages 18, 40 – 43 of the pdf)
- U.S. Army Walter Reed Institute of Research – Sleep Research Center: Dedicated to research to improve sleep among Soldiers
- Army’s Performance Triad (P3) initiative: Promoting Sleep, Activity, and Nutrition among Soldiers and Army Family members to improve health and wellness
- Army Wellness Centers, Soldiers can also request personalized assessments and education through their local AWCs
The Army Public Health Center focuses on promoting healthy people, communities, animals and workplaces through the prevention of disease, injury and disability of Soldiers, military retirees, their families, veterans, Army civilian employees, and animals through population-based monitoring, investigations, and technical consultations.



Social Sharing