MADIGAN ARMY MEDICAL CENTER, Joint Base Lewis-McChord, Wash. – Just about every medical appointment includes a nurse or doctor taking vital signs. It’s easy enough when it simply requires placing a blood pressure cuff on an arm or a thermometer in a mouth. But, when the patient is a fetus in utero, there’s a bit more to the process.
Recently, a couple dozen Madigan team members masked up and attended a course in fetal monitoring from the Rebecca Cypher, the current president of the Association of Women's Health, Obstetric and Neonatal Nurses, the training leader on the subject.
“I’ve been involved with the fetal monitoring program since 1984,” said Cypher, who is both an instructor and the lead for AWHONN’s fetal monitoring task force.
Cypher’s history and relationship with Madigan brings her through the gates knowing that she has gained much from her military experience and she has plenty to give as well.
Cypher transitioned from being in the room for thousands of births over the last four decades as an active duty Air Force and Madigan civilian nurse to teaching current practitioners the best techniques for shepherding a mother and baby through the birthing process and all its potential ups and downs.
Beyond Cypher’s years of experience in the delivery room, the students also benefitted from the extensive knowledge of Karen Winter, who has been a registered nurse at Madigan for 30 years and been instructing since 2003. Maj. Brandy Clayton, RN, and Lt. Col. Danielle Molinar, also an RN and Madigan’s chief of Maternal/Fetal Medicine, also aided in the teaching of the course.
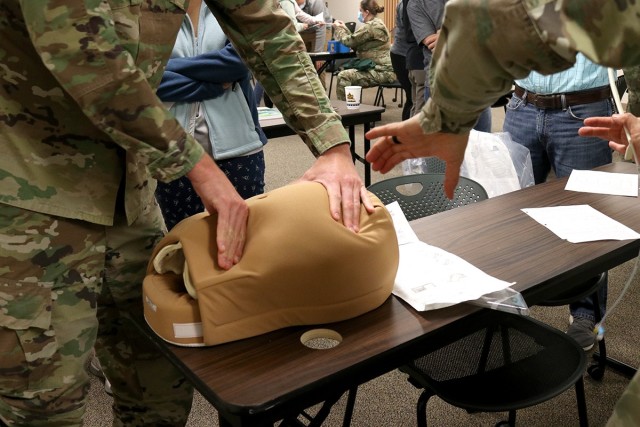
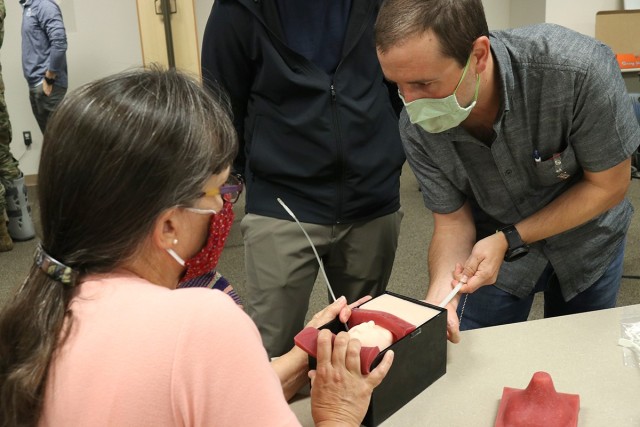
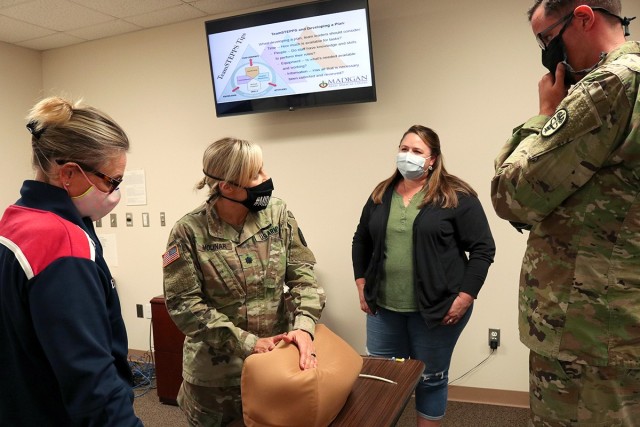
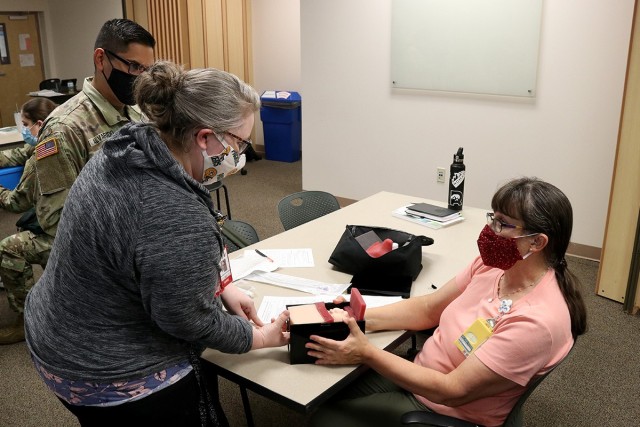
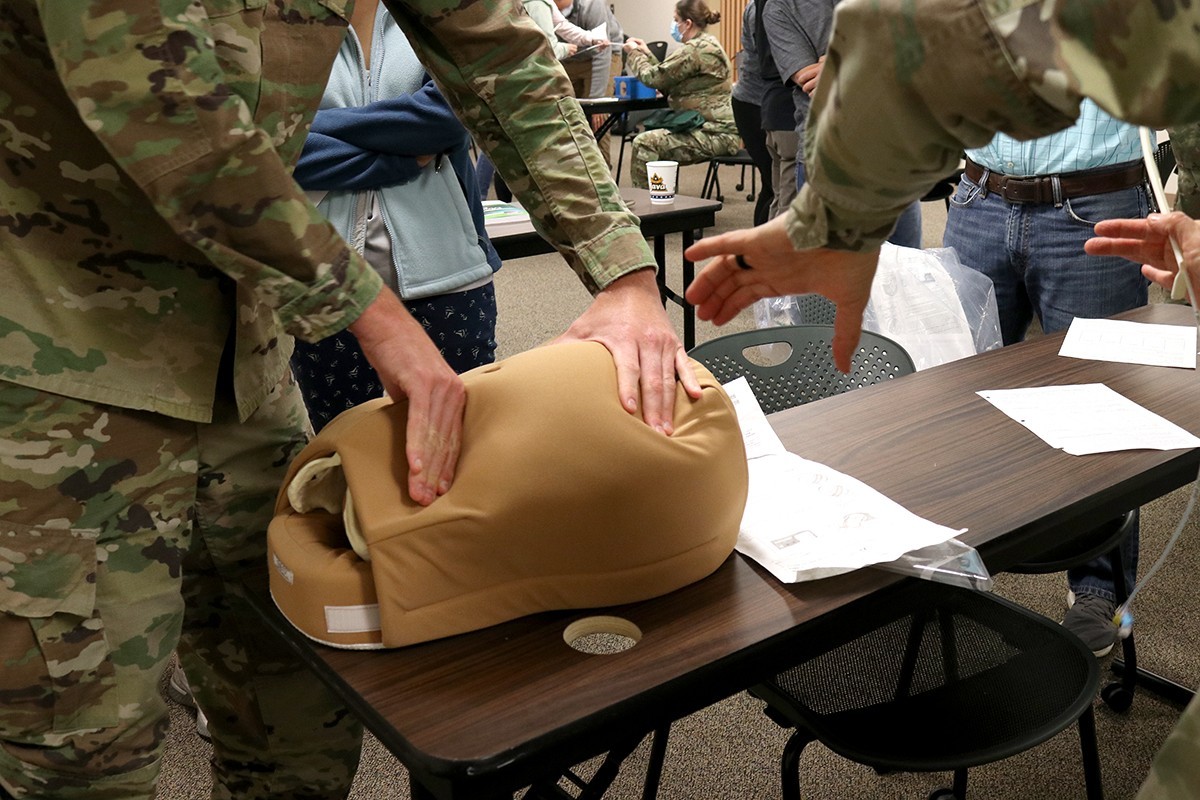
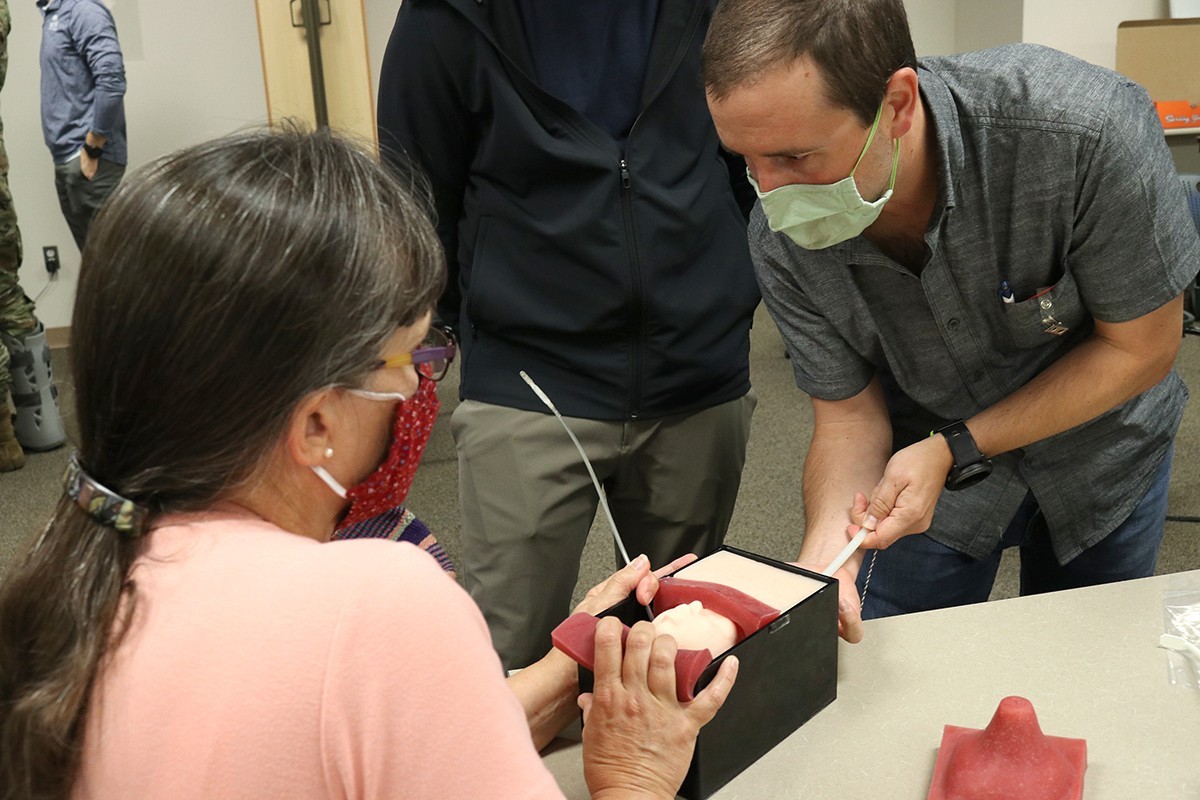
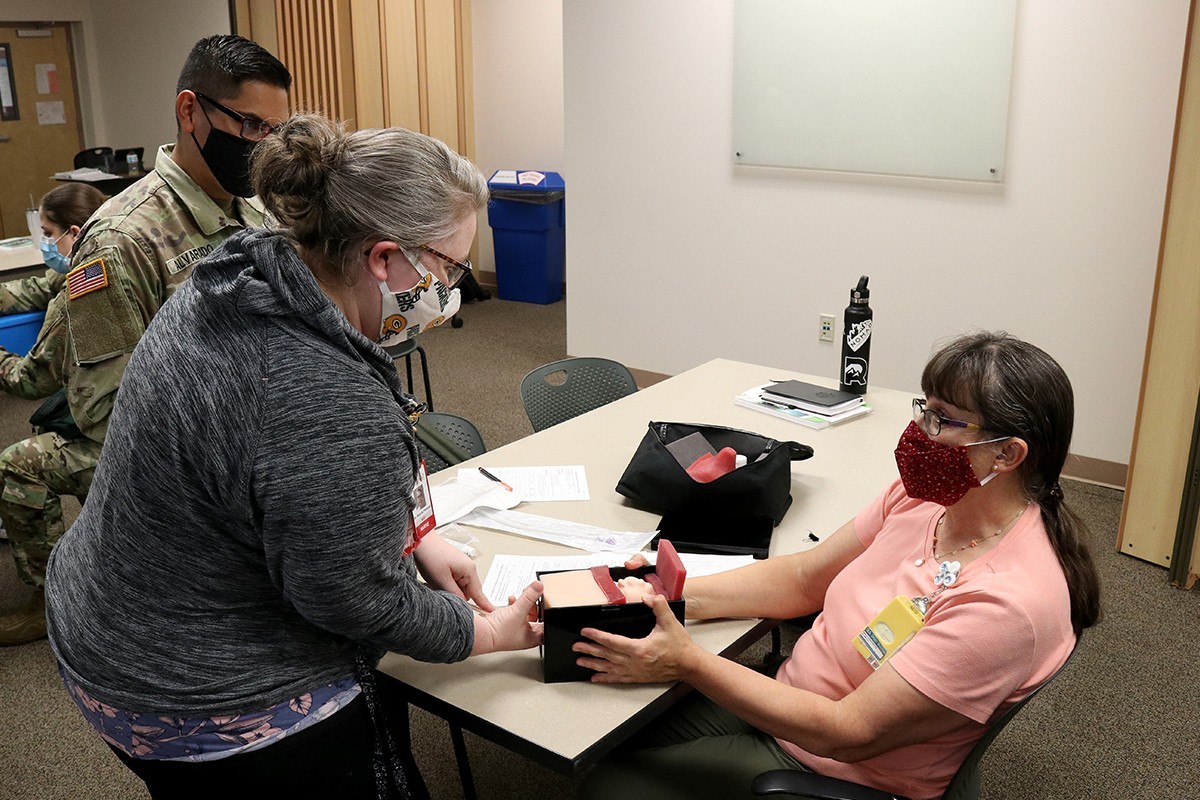
The course covered the basic assessment of a patient, through pregnancy and into delivery. It monitored vital signs of the fetus in utero, including heart rate and oxygenation and considered the uterine environment, especially contractions, to determine if the delivery is progressing properly. The class utilized textbook explanation, videos, demonstrations and a hands-on portion where students felt a mannequin belly, complete with baby, to determine where to place a monitor on the abdomen, as well as practiced placing a monitor on the fetus’ scalp and inserting a monitor into the uterine wall.
Cypher appreciated that this course has that hands-on element, which some do not. She expressed that practitioners should not rely on technology alone.
“Computers are great, but you still need to have that eyes-on, hands-on aspect to be able to bring all the pieces of the puzzle together to make sure that we have the right management plan for a patient, from a nursing perspective as well as the physician standpoint.” Cypher said. “Hands on the patient is always the best in terms of gleaning that clinical data that you need to make a difference.”
The makeup of the attendees was a multidisciplinary representation of a birthing team – from techs to nurses to doctors.
Both Cypher and Winter constantly work to stay abreast of the latest research. Winter reads articles that are written specifically for physicians so that she can speak their language and be knowledgeable of what they’re reading. She hopes this helps make the class more interesting to them.
The wide net the class casts in its attendees was considered paramount by instructors and students alike.
“I think that we have really benefited by doing the class as a multidisciplinary class since 2006. It really enhances that collaborative relationship with the physicians and the nurses that they recognize that nurses are experts that they can rely on us to give them good information or to help them with their decision-making in patient care and keeping things safe,” said Winter.
The Army Medical Command, and later the Defense Health Agency, started requiring this course in December 2016 for all nurses and physicians who play a role in fetal/maternal medicine.
Winter explained that Madigan’s multidisciplinary approach was born of the TeamSTEPPS program, which Madigan helped to develop, and its strong belief that all members of a team must work in concert to ensure safe, quality care for the patient.
“When physicians and nurses are in the same room we can have some open dialogue about who's responsible for what and who makes the decisions about when a patient needs to be delivered,” added Cypher.
Being in the room with all members of the team gives a clear view of how each sees the situation.
“There are people with all different kinds of backgrounds including nursing, nursing assistants, maternal/fetal medicine, general practice, regular OB/GYNs so it’s been very valuable to be in an environment with all those different perspectives,” said Maj. (Dr.) Derrick Thiel, a physician.
Thiel has delivered his share of babies already, but hasn’t been in a delivery suite for a couple of years. Taking the course gave him the opportunity to refresh his familiarity with the terminology and skill set. Additionally, as every Madigan resident is required to take the course, it puts every player in the room together.
Thiel appreciated the introduction.
“It’s helpful to meet the people with whom you’re going to be working because these are the people who are on the floor already. So, seeing faces, learning names and building up a rapport starts today,” he said.
While his skills were being refreshed and topped off, this course serves as one example of the DoD’s commitment to developing the skills of its entire team by affording opportunities like this class to staff for whom the knowledge isn’t required.
Malynda Piskorski is a licensed practical nurse who has worked in the civilian sector and found learning skills not within her scope of practice to be an unusual opportunity.
“Most of the fetal monitoring, the RNs do,” she said, noting that understanding the fetal monitoring equipment and techniques allows her to help identify when a mother or fetus is in trouble.
“It’s nice to be able to see these things and get the experience,” she added. “It’s a great learning opportunity; thanks to Madigan, I get to do that.”
Cypher and Piskorski agreed that the military affords them opportunities that are not readily available elsewhere, especially in terms of training and skill development.
Piskorski, for example, is a “baby nurse” who is also trained in triage and as an operating room technician.
Her main duties revolve around taking care of infants from the time of birth until they are transferred either to the Mother/Baby unit or the Neonatal Intensive Care Unit. But, her additional skills give her the versatility to step into other roles in the birthing process. She expects the new insights gained in the fetal monitoring course will simply deepen her ability to switch gears.
“It will help me monitor how the babies are doing and be able to identify when I’m needed for either the OR, or for in the room when the baby is being born,” she concluded. “It gives me a clearer view of what the overall picture is.”
Having worked in the civilian sector, she knows firsthand that training outside the scope of practice is a rarity.
“A lot of LPNs don’t get opportunities like this,” she said. “It’s nice to be able to see these things, have these opportunities and get the experience. It’s a great learning opportunity; thanks to Madigan, I get to do that.”
Madigan’s Social Media Links:
Madigan’s Facebook:
www.Facebook.com/Madiganhealth
Madigan’s Twitter:
www.Twitter.com/Madiganhealth
Madigan’s Instagram:
www.Instagram.com/Madiganmedicine
Madigan’s LinkedIn:
www.Linkedin.com/company/madigan-army-medical-center/
Madigan’s YouTube:









Social Sharing