MADIGAN ARMY MEDICAL CENTER, Joint Base Lewis-McChord, Wash. – Since the U.S. hasn’t seen a pandemic since the inaccurately named “Spanish Flu” outbreak that killed tens of millions of Americans in 1918 and 1919, it is highly unlikely many people in this country have firsthand experience with a pandemic.
Maj. Stacey Bateman, a microbiologist who is the chief of Immunology and Molecular Diagnostics at Madigan Army Medical Center on Joint Base Lewis-McChord, Wash., is proof that the doctors of military medicine know no borders.
“Part of why I went with science was I love learning new things and understanding how they work,” said Bateman. “And with science, in terms of infectious diseases, I get to apply towards helping people.”
After earning her Ph.D. from Duke University, Bateman immediately found herself in the heart of research at U.S. Army Medical Research Institute for Infectious Diseases in Frederick, Md.
“USAMRIID was research and essentially clinical diagnostics in a pandemic; that’s where I deployed for Ebola to Liberia,” Bateman said.
For two months, plus 21 days of quarantine on the way back, in 2014 into 2015, she worked at the Liberian Institute of Biomedical Research, a facility that was out in the jungle, but within a half hour drive of the capital city of Monrovia.
During the six months of the operation, personnel rotated in from USAMRIID in three-person teams, bringing fresh supplies with them. Though they fell in on a fixed facility, they retrofitted and augmented to create the level of biosafety and containment components needed for an infectious disease the likes of Ebola.
While she had great comfort with the laboratory testing, the setting and interactions of this deployment added a whole new angle to her work.
“You’re in an austere setting with an outbreak going on, and you’re not just the one doing the testing, you’re also now the laboratory expert sitting at the table with WHO and CDC and the local government and then command elements from Operation United Assistance, the 101st. intergovernmental working groups, to look at what’s our testing strategy, where is our capability and how do we streamline those processes?” added Bateman.
The list of similarities and differences between the Ebola outbreak and COVID-19 is long.
The intensity of the experience of an infectious outbreak is palpable in Bateman’s discussion of each. The constant up-tempo aspect has filled her days, nights and weekends with work. The urgency of finding the best possible recommendations to offer physicians so they can provide well-informed care to their patients is ever-present as well.
“It’s our backyard and it is a weird juxtaposition to have things both be so normal and so abnormal at the same time. In general, my experiences had been in remote and austere environments. And that brings its own challenges in logistics, in getting what you need and working with various partners,” she noted. “In a lot of respects, it’s different in flavor but similar to here where we may have a test, but there are logistics constraints because state, commercial and DOD/federal assets are all looking at the same suppliers and not having enough resources to go around for testing.”
Bateman has no trouble recognizing some significant differences either, though.
“Ebola was massive, but it was the eyes of the world on a relatively confined region. This is now global supply chains taxed because this is concurrently going on in all of those locations. The environment is different. To me, that’s the most different, and the scale,” she continued.
The novelty of this disease contributes confounding factors that help keep Bateman’s day from reaching a steady state.
“As a laboratorian and a scientist, I like to be able to give people an answer. Not just an answer, the right answer. With Ebola, for instance, we had 30 years of some level of scientific understanding of this organism, of how it impacts disease and cell types and all these other questions that we have answers to. And I find myself more often than not describing the limitations of what we know,” Bateman said of COVID-19.
Even many months in, this is still a new disease for which medicine has more questions than answers.
“In first world health, we’re used to having an answer. Emerging diseases don’t give us that luxury because we’re trying to figure it all out and what does it all mean while we’re trying to maintain patient care and test and develop all these things,” confirmed Bateman.
Since this pandemic really took off in March, Bateman and Madigan have developed increasingly greater testing capability.
“Back when we brought this on in March, we were talking 20-40-60 was a big day. We’re at 10 times that. We’ve consistently tested 500 or 600 people in a day,” she said. “Supply has been a challenge across all the systems, but that’s also why we brought on so much different capability to make sure that we’re always able to move forward a test for our patients.”
COVID-19 first struck in the U.S. in the Pacific Northwest. Madigan was up and running with its response while most DoD facilities were still unaffected; it provides nearly all of the testing needs in the area for Army, Navy, Air Force and some Coast Guard, Reserve and Guard units as well. This has put Madigan and Bateman squarely in the spotlight for leaders in the DoD.
In the last few months, Bateman has shared her lab and knowledge with Gen. James McConville, the chief of Staff of the Army and Lt. Gen. Ronald Place, the director of the Defense Health Agency.
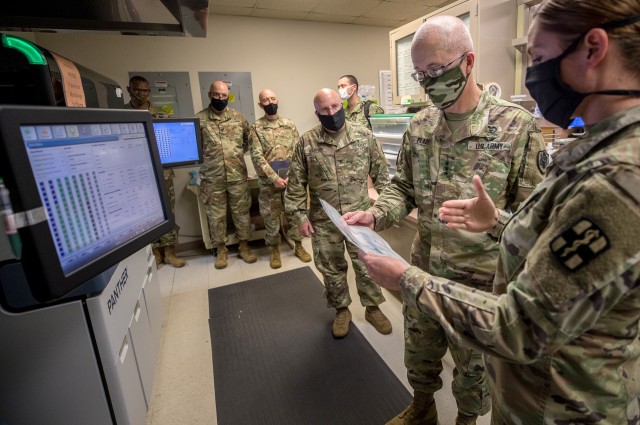
“He had very clearly been taking notes and following the development of all the testing systems and the implementation across the Army. We were able to show him the actual instruments, what was already on board and what was planned to come on board,” said Bateman of McConville’s impromptu visit that he asked to have added to his schedule specifically to see its operations.
Place was also interested in seeing the instrumentation and what testing is onboard; he also absorbed information on how the lab helps project for the command what supply lines and needs for capability look like.
Looking ahead, Bateman expects some of those needs to include the incorporation of COVID-19 into the coming respiratory season. That will take more collaboration, as so much in dealing with this pandemic has.
“I am just absolutely impressed with how Madigan has really pulled together from different areas that don’t always work together, all coordinating all these various efforts. It’s really a hospital list because it’s such a change to how we do things. It’s very encouraging to be able to see everybody come together to tackle those problems. No one section would be able to have the solution set,” she said.
She also looks forward to filling some of the gaps in knowledge we have about the virus and the toll it takes on the body.
With the understanding that exists about the disease now there are significant gaps in knowledge concerning transmissibility, the development of disease from one person to the next, the true rate of mortality, what will confer long-term immunity and what the long-term effects on health will be for the survivors.
“The best that we can do is understand as much of the science as we can, understand where there are still gaps and limitations in knowledge and advise appropriately,” said Bateman. “I'd say over the course of the next year we're going learn a lot scientifically on this but we're still going be learning stuff about it 10 years from now.”
Madigan’s Social Media Links:
Madigan’s Facebook:
www.Facebook.com/Madiganhealth
Madigan’s Twitter:
www.Twitter.com/Madiganhealth
Madigan’s Instagram:
www.Instagram.com/Madiganmedicine
Madigan’s LinkedIn:
www.Linkedin.com/company/madigan-army-medical-center/
Madigan’s YouTube:









Social Sharing