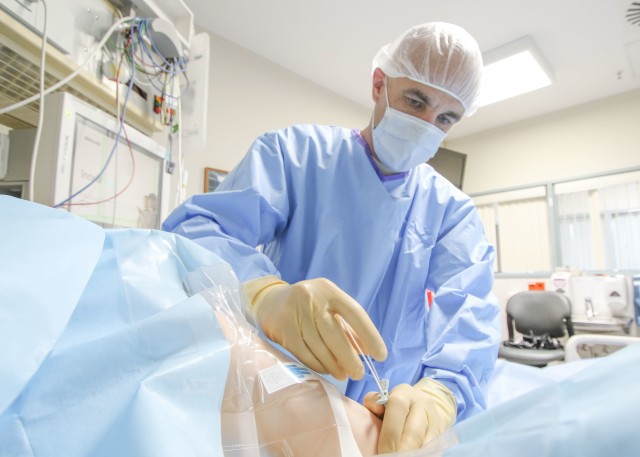
LANDSTUHL, Germany - Landstuhl Regional Medical Center’s Combined Intensive Care Unit recently added Peripherally Inserted Central Catheter as part of ICU capabilities at LRMC.
Peripherally Inserted Central Catheters, or PICC lines, are used for long-term intravenous antibiotics, nutrition, medication and blood draws. The treatment consists of a thin, flexible tube that is inserted into a vein in the arm and threaded to the superior vena cava, or right side of the heart. According to the National Cancer Institute, PICC lines may stay in place for weeks or months and helps avoid the need for repeated needle sticks.
“There's some medicines that are harsh on the veins and certain medicines are more effective when delivered to the central system, right to the heart,” said U.S. Air Force Capt. Arik Carlson, critical care nurse at LRMC’s ICU. “In emergent cases, normal (Intravenous therapy) is usually performed when admitted the emergency room. (IVs) are only good for a few days, a pic is a long term process for somebody who needs medication and antibiotics for a long term time.”
According to Carlson, Patients undergoing PICC treatments can be discharged with the line in their arm. This allows for reduced IV insertions, reducing patient discomfort and the risk for infection from repeated needle sticks.
“It can be very frustrating for patients if the IVs don't last very long because of the medications that they're getting. It’s very uncomfortable, of course, and depending on their course of antibiotics, it could be a long term course, some up to six weeks long,” Said Maj. Julie Duffy, critical care clinical nurse specialist, LRMC.
While the majority of patients at LRMC are Service Members and their families, PICC treatments will mainly benefit patients who must undergo multiple medical treatments or blood draws, such as hematology and oncology patients.
“Even nutritional support products that we can give that are very tough on the vasculature,” said Duffy. “If a patient is sick enough and having a hard time with oral intake of their nutrition, we will sometimes supplement it with nutrition that goes into their veins.”
“It's a quick procedure, it's done as sterile as possible,” said Carlson, native of Ottawa, Illinois.
As the medical evacuation and treatment center for all injured U.S. Service Members, civilians, and members of 56 Coalition Forces serving in Afghanistan, Iraq, as well as Africa Command, Central Command and European Command, LRMC’s implementation of PICC treatments will benefit patients who come to LRMC with central venous catheters, performed as emergent treatments in deployed, austere environments.
Because central venous access is one of the most common components in the care of critically-ill patients, using PICC treatments will also decrease the number and amount of time health care teams spend performing central and IV lines, increasing the teams efficiency and reducing patient touch points.
“COVID-19 patients generally do have central lines, but depending on their condition, and medical history, if we had somebody that would need a PICC it would help protect the staff and protect the patient, because if we need to get into the central bloodstream quickly, we can do that,” said Duffy. “
Because medical operations differ in Germany, the availability of PICC training is currently limited to those who have trained at other Military Treatment Facilities in the United States. Additionally, PICC-certified nurses can increase capabilities and efficiency at LRMC medical wards.
“(PICC-certified nurses) can lessen the load off physicians, provide good care to the patient, while reducing risk of infections,” said Carlson. “The cost of nurse placing one of these is substantially less than a physician having to place one. Physicians can be focused on other things while we're placing these.”
Carlson, along with other PICC-certified staff members, are designing a training program at LRMC to keep the capability at LRMC’s ICU and train future generations of nurses in the procedure.

Social Sharing