LANDSTUHL, Germany - As the COVID-19 global pandemic continues, wearing a face mask has become normal in most work settings. In particular, medical facilities continuing toprovide patient care during COVID-19 has led to increased risks with droplet and contact transmission.
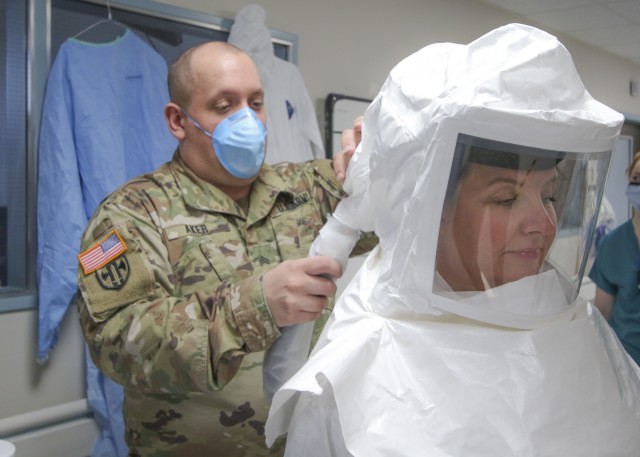
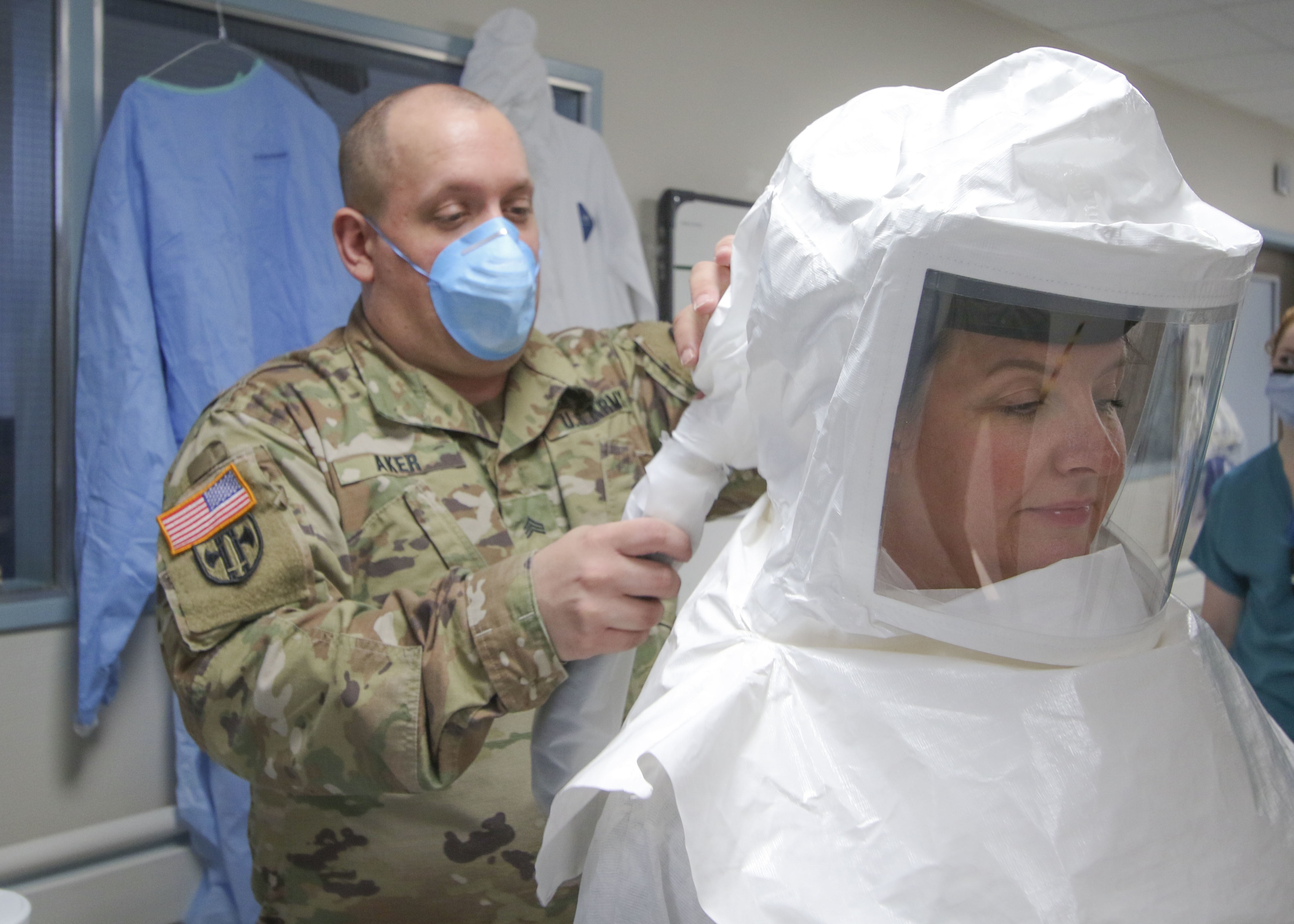
To reduce the risk of exposure to the coronavirus in the hospital wards and clinics, Landstuhl Regional Medical Center medical personnel are conducting training on the Powered Air-Purifying Respirator system, a full-body respirator used to safeguard staff members from contaminants. While most PAPR systems are similar, the critical introduction to proper use, donning and doffing procedures, and safety measures are unique to each organization.
“The N95 (facemask) provides adequate protection to staff members, but what the PAPR system does is provide increased comfort while purifying the air,” said U.S. Army Capt. Mario Vergara, a clinical nurse specialist for LRMC’s Medical-Surgical Unit. “It actually feels like air conditioning is pushing the air through the suit itself. The purpose of the training is to get the staff up to speed and comfortable using the system.”
While LRMC’s critical care staff are already familiar with such systems, efforts to increase manpower capabilities for COVID operations requires the cross-training of providers from non-inpatient settings. Additionally, by practicing with the system staff members are more adept to react when needed with the PPE they have on hand.
“When receiving a patient, a lot of things are going on and you want using PAPR systems and other equipment to already be checked off in your mind,” said Vergara, who is also the PAPR training lead at LRMC. “We're working to get the staff comfortable using the equipment and supplies that we have here, and retraining staff in the environment in which they're going to be providing care.”
Although the PAPR system provides head-to-toe coverage and protection against droplet and contact risks, Vergara says the system will only be utilized during initial COVID-19 patient admissions to minimize supply strains.
“Our goal is to be able to use the PAPR system for an extended period of time as opposed to taking off N95 masks, goggles, shield, hood, multiple equipment items where risks of contamination through contact is more possible,” said Vergara. “While treating the patient, (medical personnel) are more focused on treating the patient and not worried so much about the way the masks fits, the comfort of the mask pushing into your face, the goggles rising up, the goggles fogging up. There's a lot of factors that are involved with PPE.”
Additionally, Vergara states the PAPR systems hooded face shield allows medical personnel to present themselves to a patient who may already be fearful and vulnerable, advancing the patient care process.
Aside from critical care and inpatient staff, any staff member who would go into the room with the COVID-19 patients are receiving the training.




Social Sharing