LANDSTUHL, Germany -- Health care providers everywhere have answered the call to fight and prevent the spread of COVID-19. At Landstuhl Regional Medical Center, more than 75 nurses are among those who are volunteering to augment the critical care staff to combat the global pandemic if needed.
As part of larger efforts in staff readiness and development, clinical personnel not normally trained in critical care are undergoing various training elements designed to increase staffing capabilities in support of COVID-19 operations at LRMC.
“We’re focusing on skills directly related to critically ill patients that are common in the COVID-19 patients that are being seen throughout the world right now,” said U.S. Army Maj. Julie Duffy, a clinical nurse specialist at LRMC’s Intensive Care Unit. “We're working to make sure that (non-ICU nurses) are trained and have the understanding of COVID-19 and what (COVID-19) patients are experiencing, and the skills related to it.”
In recent guidance from the Centers for Disease Control and Prevention, health care facilities are urged to consider mitigation strategies for staffing shortages to continue providing safe patient care and work environments. The training aims to educate nursing augments from different areas of the hospital in critical care medicine, consisting of online and hands-on training under supervision. Subjects include training specific to COVID-19 patients such as hemodynamics monitoring, airway management and mechanical ventilation basics, treating adult respiratory distress syndrome, infection control and personnel protective equipment protocols.
Inpatient nurses, as well as nurses from other units throughout LRMC, are volunteering to augment the ICU unit, increasing the capability to care for both COVID and non-COVID critically ill patients.
According to Duffy, participation in the multidisciplinary efforts toward minimizing the impact of COVID-19 on other operations at LRMC has benefits beyond supporting critical care units.
“There is a benefit for the nurses as well: the sense of purpose and helping. I think it's going to be big for a lot of them,” said Duffy. “We know that there's a nursing shortage nationwide. So to be able to know that we helped in some way with the pandemic, I think that will emotionally help nurses.”
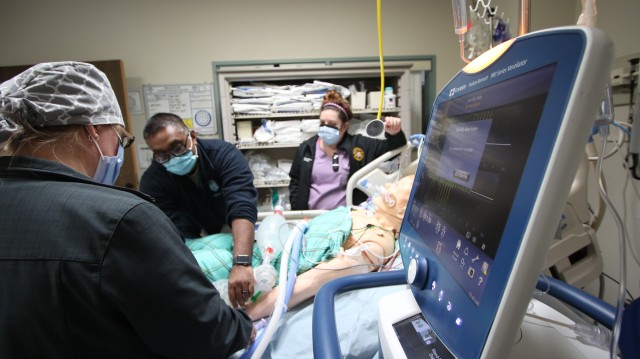
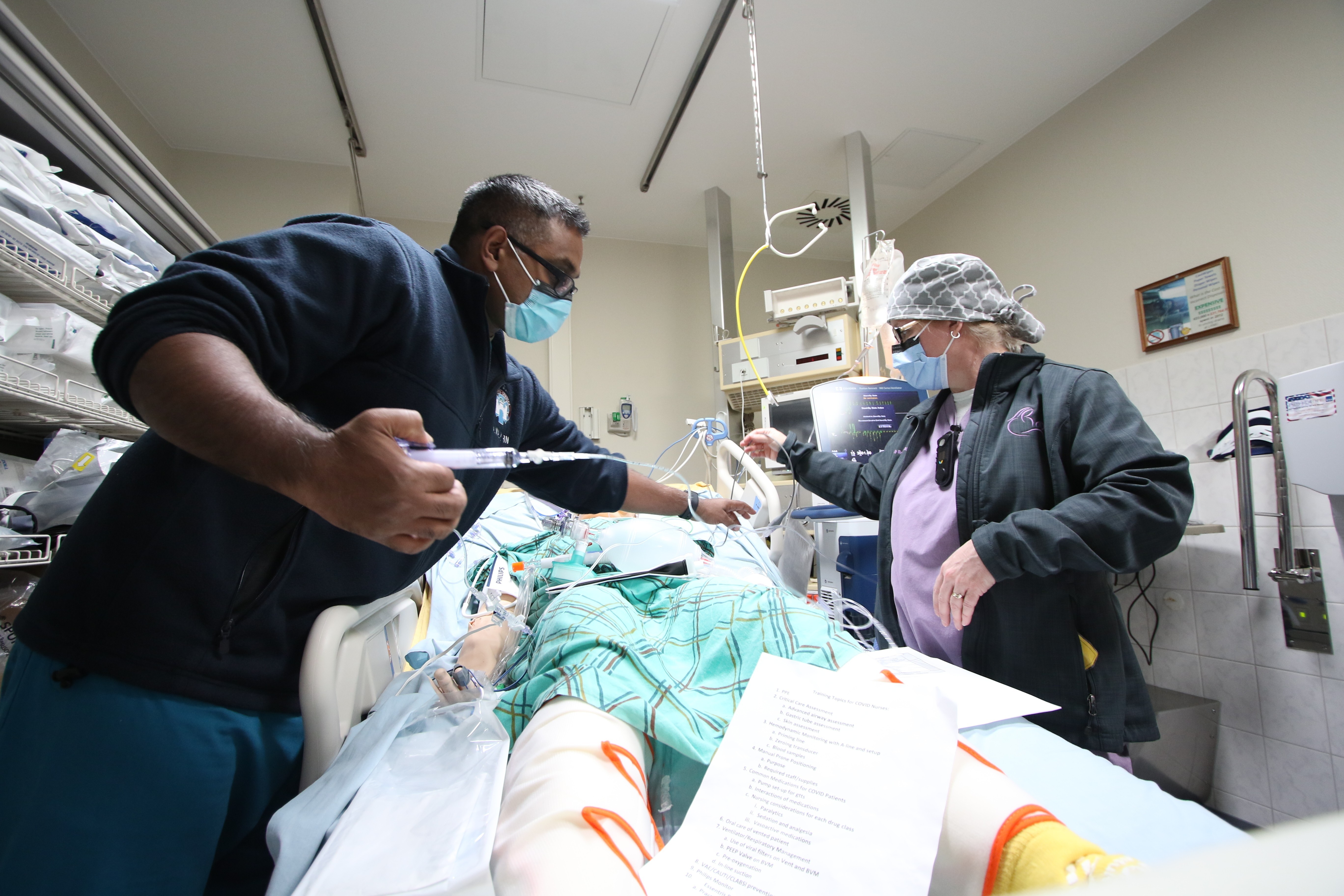
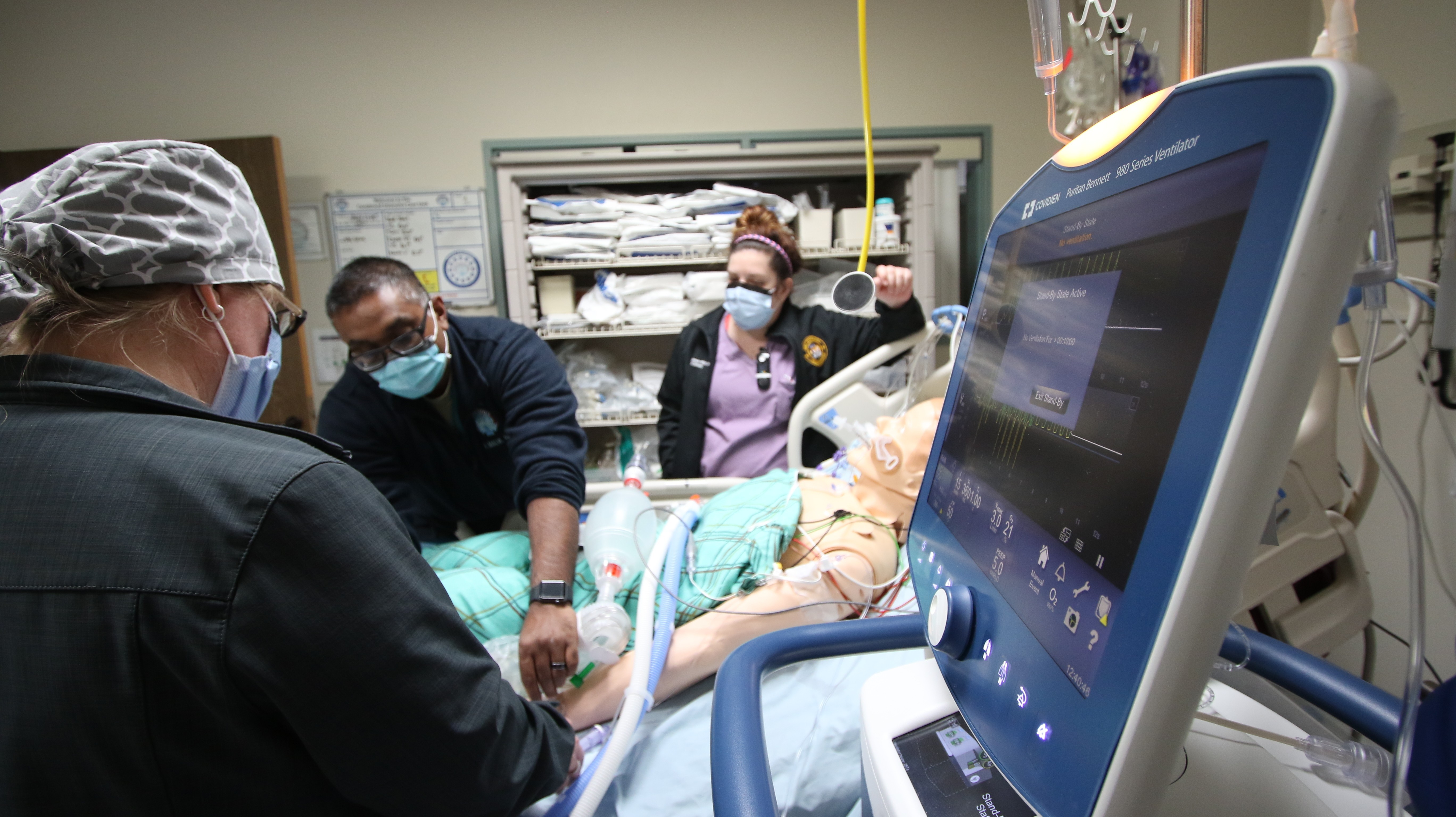
Three times a week, cohorts of nurses continue to train with ICU and pulmonary staff members using the latest evidenced-based practices in treating individuals diagnosed with COVID-19. As more staff members are trained, Duffy expects training objectives to evolve.
“Right now, it's really more about familiarization with the equipment and just getting some hands on working with it, then we'll be able to throw it into patient scenarios,” said Duffy. “Soon enough, nurses from throughout the facility will be trained so they're able to help (ICU) should the time arise.”



Social Sharing