MADIGAN ARMY MEDICAL CENTER, Joint Base Lewis-McChord, Wash. -- The military's medical professionals know that the ready-to-fight tonight mantra assumes a hearty foundation of healthcare support. Madigan's clinics and teams are in constant pursuit of improved healthcare delivery, and access to care is top of the list to support the service member's ability to be continually ready.
Maj. (Dr.) Eliza Szymanek, a physical therapist, was a key member of a team implementing a performance improvement project to provide timelier care for acute musculoskeletal conditions in the active duty population.
"We saw this as an initiative to start to help the Soldiers get in earlier," said Szymanek.
In early 2018, physical therapists within Madigan's outlying clinics and brigades started seeing active duty patients at sick call. During the ensuing year, over 2,100 service members were evaluated and treated through direct access.
Every physical therapist on Joint Base Lewis-McChord is a provider with a doctoral level degree and both diagnostic and prescriptive capabilities. When a service member comes to a clinic for sick call due to a complaint of an injury or pain, being evaluated and treated by a PT shortcuts the typical process of initial evaluation by their primary care manager and then being referred. That process can take up to 28 days before a patient sees a PT.
Through this initiative, all clinics on JBLM that have PTs now offer direct access. Lt. Col. (Dr.) Lisa Konitzer, the chief of Physical Therapy, offered some insight into why this matters.
"If we can see patients earlier, we've found that we can decrease medication prescription and we can decrease imaging," said Konitzer. "We can improve that lost duty time and we can also have a significant impact on profile management, returning Soldiers and Airmen to duty faster. All of those things we've seen."
The PI project utilized research that shows a projected cost savings of $1,543 per patient over the next year for those who entered physical therapy through direct access. It also showed that musculoskeletal conditions are the leading cause of healthcare visits, lost duty days, non-deployability and disability in the Army.
When Konitzer did the math for the 2,100 patients counted thus far at $1,500 each, that's a $3 million savings in patient care costs. She also knows that the impacts are just beginning to be felt.
"I can tell you it just keeps building. Winder Clinic in the month of August saw 222 people in their sick call; there are three PTs there. That's a pretty hefty number," said Konitzer.
She expects the numbers to keep climbing especially since, starting Aug. 12, a PT has been embedded in Madigan's Family Medicine Clinic. She knows having that provider within a clinic raises awareness.
"When you're co-located, now you have that ability to just tag someone right down the hall," Konitzer said. "He's definitely spreading the word and making sure that the providers are aware of what he can do for them."
What a PT in a sick call clinic can do is take on those ankle and knee sprains and those back pain issues and move that patient into a rehabilitation plan right from the point where they come into the clinic for care. In the process, the primary care providers and specialists can focus their attention on other ailments and injuries.
"We have these skillsets, but we reviewed those things that come into sick call that typically we wouldn't see in a referral," said Szymanek.
Konitzer elaborated, saying, "We are all instructed in school on musculoskeletal evaluation and treatment so the train up that we do is focusing a little bit more on the pharmaceuticals, the imaging, the differential diagnosis -- the things that are going to be really important to ensure that the patients that we're seeing are appropriate for us to be seeing."
With nine physical therapists in clinics throughout the base and an additional nine assistants and techs who can do initial ankle and knee evaluations, that takes a load off other clinicians. It also furthers Madigan's teaching mission.
The techs, for example, come to Madigan for their Phase II training where they will become adept at those evaluations. "That's in their knowledge base," said Konitzer. "That is part of a downrange mission, if they were separated from the PT, to be able to see an ankle sprain and initially manage that."
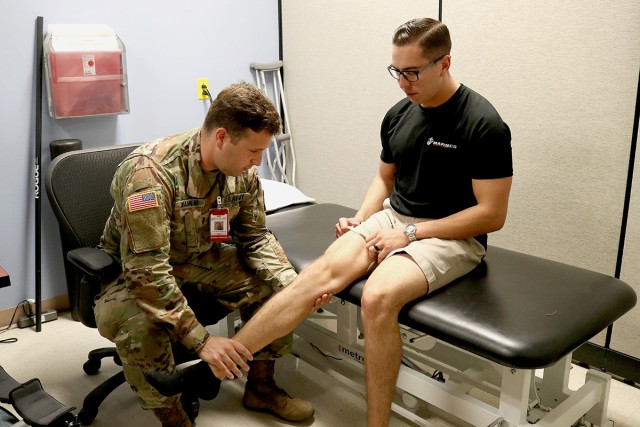
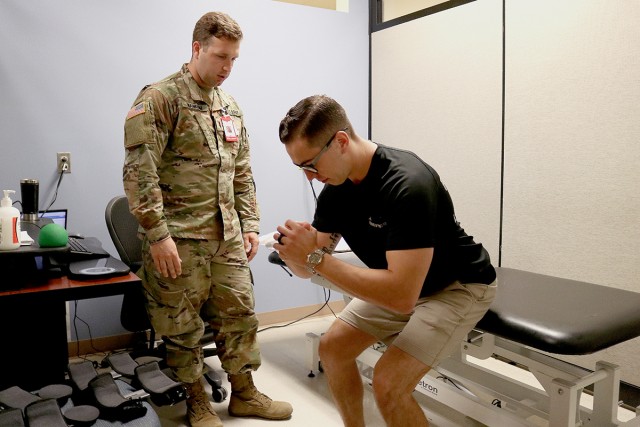
As Physical Therapist 1st Lt. (Dr.) Nicholas Wankum evaluates the range of motion of Marine Staff Sgt. Dalton Everhart's injured knee in a follow up visit, the advantages for the patient of direct access become apparent.
"I went straight from the ER when I was referred over to here," said Everhart. "I called over; I was supposed to come in for sick call, but they just set me up with an appointment which was way easier because I didn't have to wait. Ever since then, Lt. Wankum has been helping me out. It's been really easy. "
"Working in direct access has been an awesome opportunity for me to be able to help out soldiers very acutely after injury," concurred Wankum.
He was able to start working with Everhart five to six days out from his injury as opposed to potentially three to six weeks out, which would be the usual referral process.
"For something like an acute injury like this, things can get stiff and then you're working to get range of motion back after it has stiffened, which can take a lot longer," noted Wankum. "So, for people to be able to get in soon in those situations, I think it can make a big difference."
Speeding a patient's healing process has benefits for the person and their unit.
"Ultimately, it helps with readiness which is really what we're trying to go for with this -- trying to get them back to where they need to be. It helps the units take these issues and handle them a lot quicker so we can help the force be ready," said Wankum.
During his visit, Everhart's greatest focus was on getting back to where he was, physically and professionally, before his injury.
"Ninety percent of my job is moving around. It doesn't look great when I have to sit in the office and say, "Have fun working out, guys; I'll be there eventually," Everhart said. "So, for me to go from when it happened that I couldn't walk and I was limping -- it was awful -- to exactly almost a month later and now I'm back out there working out with them and being able to do a lot more. It feels a lot better and makes me be a lot more confident."
The long-term goal is to put personnel in place to offer direct access to dependents and retirees as well. For now, direct access is already equaling direct impact on active duty units.
"Winder is a great example of unit level commanders coming up to them and saying, 'Thank you so much for how you've changed some of your processes, making this so much more accessible for our Soldiers.' When you have a unit commander coming up and telling you that this is making a difference in our Soldiers' lives and our ability to get them back off profile sooner to do any of the things we need them to do at work, that to me is the biggest impact," said Konitzer.


Social Sharing