FORT BLISS, Texas -- William Beaumont Army Medical Center is taking a page from U.S. Army line units by developing an Individual Critical Task List (ICTL) for healthcare professionals that promotes and measures readiness to deploy.
"A medic is never going to do a chest tube or a central line stateside, but down range, in a field setting, they need to be able to step in if needed," said Lt. Col. Maria Molina, a chair on the Central Simulation Committee, while observing the innovative training. "If you've done this training, you should be able to step in when needed if there are not enough general surgeons available to treat casualties, whether it's down range or even a mass casualty event stateside."
The ICTL training -- 27 tasks that are common in 7 main military occupational specialties -- will not only help leadership measure the clinical readiness of health care providers to better support battlefield medicine, it will be used to validate medical personnel for future deployments, added Molina.
"This is a big change, a big step for the Army," said Molina, who is also the chief of the Simulation Center at Fort Sam Houston. "There's never been a checklist for medical professionals that measure competencies to go downrange and that's what this training fulfills."
The bottom line up front: More versatile providers equals more lives saved
The scenarios took more than a year to develop and also offers health care professionals the opportunity to earn Continuing Medical Education (CME) credit while learning to work effectively in a team, said Maj. Janice Martinez, a staff officer for education and training at WBAMC.
"We have five person teams, so let's say, the medic in one doesn't get to intubate the patient, he has the opportunity in the other two scenarios to do that," said Martinez, who helped build the simulation program. "They're rotating the team members and the roles, so everybody can get a little hands on with this. Everyone gets credit, because they'll get that familiarization training, regardless. The more we can maximize everybody getting their hands on and actually doing these tasks the better."
Train as you fight, fight as you train
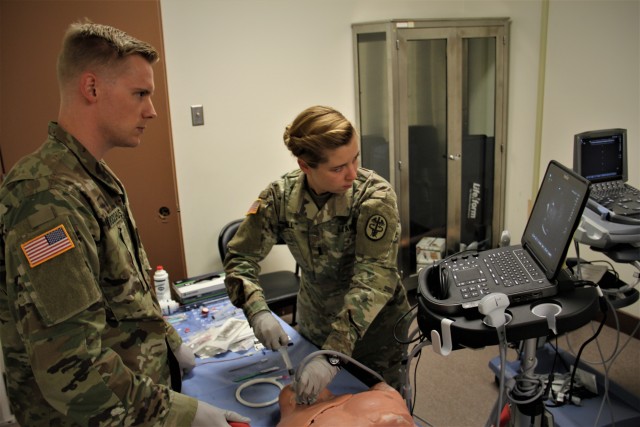
In August, participants rotated through seven stations at the Fort Bliss Medical Simulation Training Center which included three trauma scenarios, two with an emphasis on current available forward-thinking capabilities to train health care staff in practices different from normal operations.
After leading his team through a simulated burn casualty scenario at the WBAMC's Simulation Center, Lt. Col. David Escobedo said the last time he did this type of training was before his deployment to Baghdad, Iraq in 2008.
"As a family physician I'm not going to see a lot of burn victims," said Escobedo, a physician at WBAMC. "But, if I deploy, this type of training only reinforces what I already know and will help me hit the ground running. It's like muscle memory."
Sgt. Olena Solomnikova, a respiratory therapist, said she was inspired to change her military career path after watching her unit's Physician Assistant save their supply clerk after an Improvised Explosive Device nearly severed her femoral artery in Afghanistan in 2013.
"She would have died if it weren't for him. I want to do more, see the bigger picture. This training gives me the practical skills -- it's real-life, exposure to combat," said Solomnikova, who has applied for the Interservice Physician Assistant Program (IPAP) herself. "You never know, you might lose someone, or you might not have a doctor and you will have to be able to do those interventions."
Boots on the ground
After the training, WBAMC will analyze the feed-back to determine gaps and resource requirements to refine and establish a set of ICTL validation scenarios for future training events at military treatment facilities across the country.
"We essentially created a product that can be replicated very easily," said Maj. Chris Bell, a trauma critical care surgeon at WBAMC. "We can do it as a single day event, three-day event, 10-day event. We can tailor it to different MOSs or we can have the scenarios be very general and bring all the MOSs together."



Social Sharing