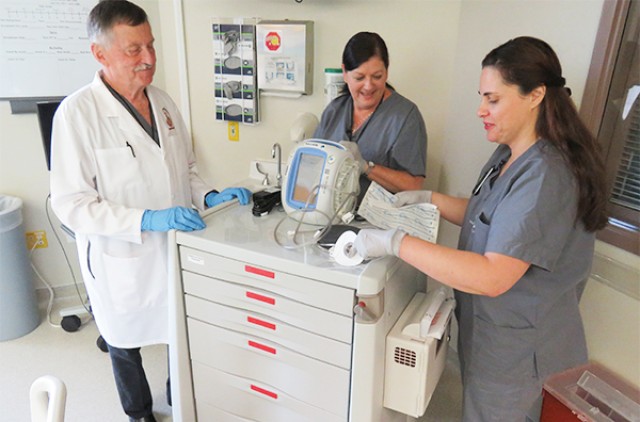
MADIGAN ARMY MEDICAL CENTER, Joint Base Lewis-McChord, Wash. -- When she underwent ankle surgery in December, Jess Smith had no idea the path she would navigate.
She unexpectedly experienced an allergic reaction to the internal sutures in her ankle and contracted an unusual bacteria as well -- both of which set off the perfect biological storm for a chronic wound to form.
"Since I'm a nonstop kind of person, there came to a point where I actually had to be admitted … I had an open wound down to the bone basically," said Smith, who is both a Madigan patient and a nurse in the Limb Preservation Clinic.
In stepped the Wound Care Service's inpatient team, which stood up just six months ago to provide dedicated expertise to hospitalized patients with chronic wounds. The two-nurse team, which boasts 25 years of wound care experience between them, joined forces with the service's long-standing outpatient clinic to provide a continuum of care for patients like Smith with chronic wounds.
"In addition to providing hands-on inpatient wound care, the goal was to work very closely with the staff nurses to educate them on the importance, for example, of the skin assessment. Joanie (Santucci) and Eloa (Reid) spend a lot of time working with the inpatient nurses to make sure there's an appropriate focus on assessing patients, preventing ulcers, identifying early skin breakdown with education, writing policies and hands-on care," said Dr. Charles Andersen, chief of Madigan's Wound Care Service.
Although most wounds don't require the extra care of this specialty, some just don't heal as expected and become chronic. In these cases, patients might be referred to the Wound Care Service.
Regardless of the type of the wound -- such as a pressure sore, burn or surgical site -- treating them involves three factors: treating the wound itself, addressing the cause of the wound, and remedying any negative healing factors, such as poor blood flow.
While the most common treatments for chronic wounds are advanced synthetic dressings and negative pressure wound therapies, an almost innumerable amount of treatment options exist with the common goal of creating an environment that contains the right level of moisture for optimal healing.
In Smith's case, regrowing tissues and receiving a skin graft required the inpatient nurse team to treat her with a Wound Vacuum-Assisted Closure device to increase blood flow and reduce edema (swelling caused by excess fluid buildup), and an instillation negative wound therapy that infused antibiotics directly into her wound bed for set periods of time.
"Their knowledge and ability to adapt to whatever the issue is, is amazing," said Smith of the team.
"We're often asked to see people to figure out what the etiology is (what caused it), how to best treat it and manage it and include possibly surgical teams, and then work directly with doctors and nurses and write wound care orders," said Santucci, who along with nurse Nancy Hodges also formally provides wound care education as a satellite site for the University of Washington's Wound Care Fundamentals Course.
The team works directly with multidisciplinary medical teams on a daily basis -- from nurses to doctors and from case managers to physical therapists.
"It's a cultural change; it's new for everybody," said Reid, who emphasized the team's role in offering consults. "We always leave the door open for the nurses."
In the inpatient setting, wound care is a focus for patients from admission to discharge, starting with nurses scanning the skin conditions of all patients. The inpatient Wound Care Service team focuses particular attention on identifying patients who are more susceptible to pressure ulcers, which can occur when patients are less mobile. In fact, patients who are in at-risk situations, to include surgical patients, are assessed more frequently, said Santucci. If patients do develop or come in with ulcers or other wounds, she and Reid work with care teams to treat the wounds early on.
To ensure wounds are still treated even after hospitalization, patients who need additional follow-up care are then set up with appointments with the outpatient clinic as a part of their discharge process.
"The idea is to make that seamless between the outpatient and the inpatient," said Andersen about the wound care pathway; patients can also now be more easily admitted if needed thanks to referrals from the outpatient wound clinic.
Smith took part in that pathway herself as she transitioned to the outpatient clinic after discharge. After four weeks as an inpatient, she offered nothing but praise for the service's inpatient nurse team.
"They literally don't stop until the day is done … There are days where they're still here well past their shift," she said. "That's the kind people they are, and how dedicated they are to their jobs here and to the patients."
Social Sharing