FORT BRAGG, N.C. (June, 2, 2017) -- In every military conflict throughout history, medics have proved their worth by providing care for those injured on the battlefield.
Recently, several studies conducted over 10-year span examined the battlefield injuries from Operation Iraqi Freedom and Operation Enduring Freedom. Two of these studies, "Death on the Battlefield: Implications for the Future of Combat Casualty Care" by B. Eastridge and "Eliminating Preventable Death on the Battlefield" by R. Kotwal demonstrate areas where Army Medicine could focus efforts in order to enhance the skills of our medics and potentially save lives.
The results stated that 90 percent of all battlefield deaths occurred prior to reaching a medical treatment facility. Twenty-four percent of those military members who died prior to reaching a surgeon had potentially survivable wounds. These wounds, though serious, could have been treated prior to evacuation thus saving a life. The assumptions from these studies are that these wounds were left inadequately treated due to lack of knowledge or skill, or lack of confidence on how to treat such extensive wounds.
According to an Army Medical Command Regulation, AR 40-50, Medical Treatment Facilities have a responsibility to ensure a "robust training program is instituted which ensures the development of medical Soldiers." The goal is for medics to be able to perform at a high level and be able to operate as independently as possible, especially within austere environments.
Concurrently, the Office of the Surgeon General submitted a memorandum in the fall of 2016 providing guidance that all enlisted Soldiers must be trained and developed within their skill set to meet the Army's number one priority: readiness.
We fight as we train, and historically medics have not been able to maintain the extensive knowledge they have received in the advanced individual training they receive upon entering the Army.
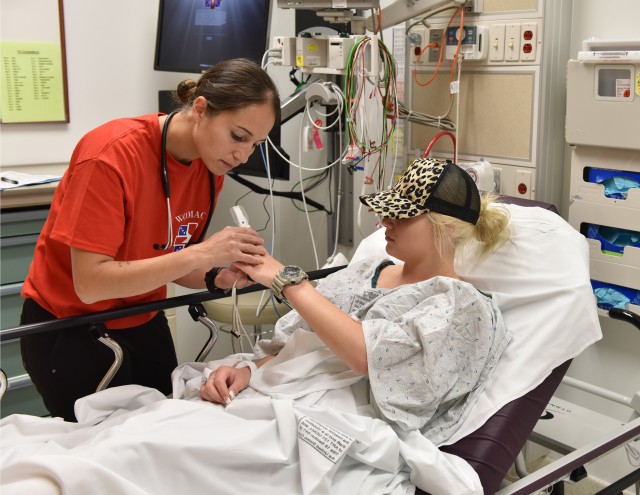
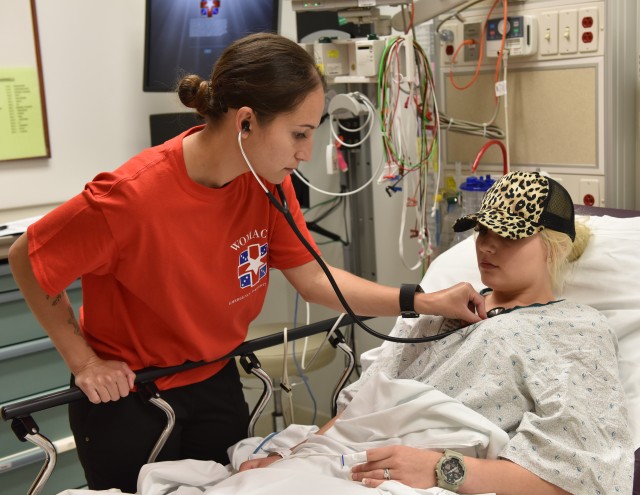
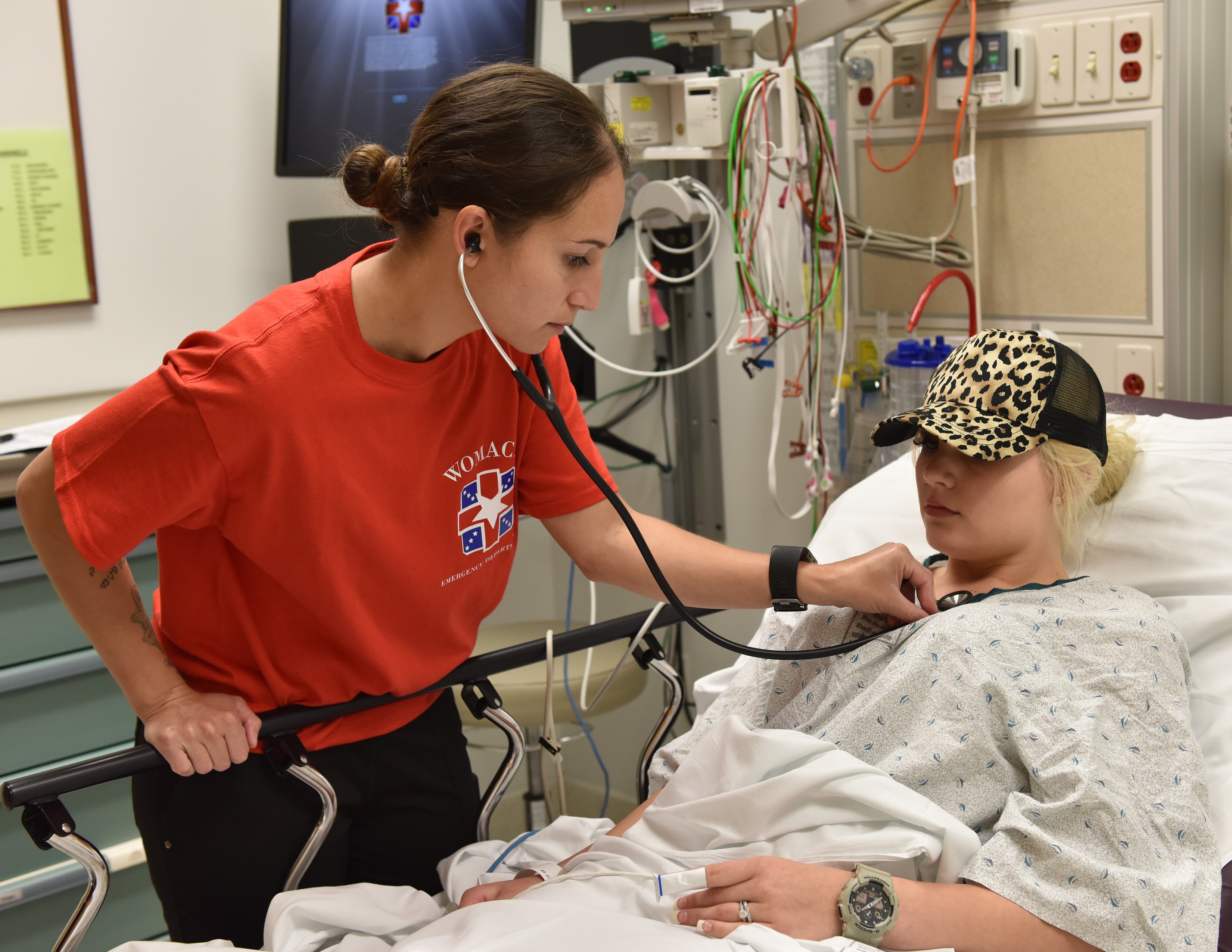
Womack Army Medical Center's Emergency Department has taken steps to change this culture of how medics are used in the garrison environment. The vision is to provide not only education, but a sustainment platform for medics to be constantly learning, both in skill development and medical knowledge. Several Emergency Department clinicians came together to develop an enhanced training program for medics with Maj. Scott Fisher developing a textbook, timeline, classes and exams that were easy to reproduce, flexible enough in the clinical environment and challenged medics to think outside the box. With this platform in hand, Roni Paul, the program clinical instructor has provided the medics with tools, clinical knowledge, skills and confidence to be on their own in a line unit or on the battlefield.
The program uses a combination of classroom instruction, skills classes, clinicals with preceptors and a dedicated program instructor. The initial group showed at least a 10-point increase in knowledge from beginning the program. The feedback from the medics and the nurses that mentor them has been extremely positive.
The Enhanced Medic Program is a pilot program. The second class to go through the program graduated June 2 and they are currently completing the two-week internship requirement. The next class is set to start on July 10.
Spc. Matthew Struys, one of the first graduates from the program, said that the classes definitely improved his skills and raised his confidence.
"Morale is higher," said Struys. "I know what I am capable of and I receive more of a higher level of respect from the nurses and those around me in the ED."
The impact is carrying over to the current class, as well.
"Before I didn't know the 'why' of running labs, EKGs, etc. Now I am starting to know and see the big picture and to come full circle is a huge benefit," said Sgt. Kelsey Douget, a medic who went through the second iteration of the program.
After the 10-week program the medics continue the pairing with nurses on the floor and work as a primary caregiver for one to two beds on a shift with nursing and provider oversight. This practice is based on the civilian practice model as noted in a literature review.
The nurses have to have full engagement with the medics to be effective. The preceptors are handpicked for their unique knowledge and their ability to teach while challenging the medics. The preceptors need to ensure the medics develop the skills to engender the trust in their ability to take on a patient assignment and see that patient through until the end of their stay in the Emergency Department.
Data is still being gathered on the effectiveness of the program for the medics, ED staff and mainly patient outcomes. The future plan is to begin training and sustaining the program for medics outside of those assigned to the ED in order to continue to improve the readiness of our medics.

Social Sharing