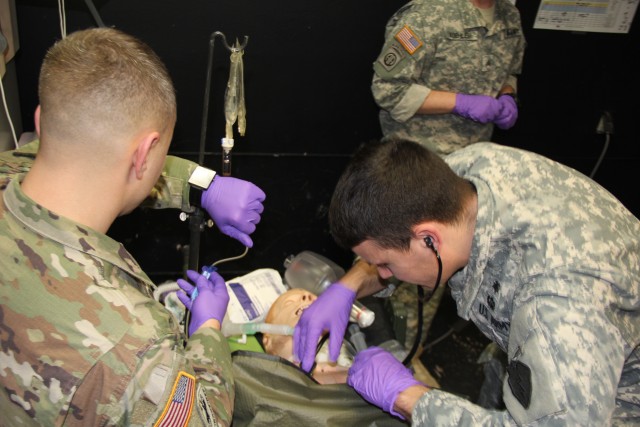
FORT WAINWRIGHT, Alaska - The nation's current deployed operational environment is evolving and so must Army medic training.
Medics from Medical Department Activity-Alaska, Madigan Army Medical Center, out of Joint Base Lewis-McChord, Washington, and 4th Brigade Combat Team (Airborne), 25th Infantry Division, gathered for a week-long Delayed Evacuation Casualty Management Course to begin the shift in mindset and to build the skills necessary for providing care on the ever-changing battlefield.
"The training our medics were provided made them successful and saved many lives in Iraq and Afghanistan," said Command Sgt. Maj. Uriah Popp, CSM for MEDDAC-AK, and the proponent behind the training. "However, as our battlefield requirements evolve so must the training of our medical personnel to meet this ever-changing environment."
According to Popp, many of our lessons learned and advancements in casualty management were learned from the Special Operations Forces community.
"The SOF community is extremely adaptive and able to mitigate changes in their operational environment through rapid fielding initiatives and instantaneous changes in their tactics, techniques and equipment," Popp said. "Looking at our current and future operating environment, I believe Army Medicine must also adopt these principles to continue the life-saving successes that were seen in Iraq and Afghanistan."
Popp and Army Medical Command leaders recognize that prolonged care will be a reality, and there will be a decision point for medics to decide stabilization care measures are necessary to further improve a patient's condition and prognosis when evacuation to a higher level of care is not possible.
"I think the notion of prolonged care is going to be very important," said Lt. Gen. Nadja West, U.S. Army Surgeon General and commanding general, U.S. Army Medical Command.
We may not have air superiority - they may not be able to have the leisure or the luxury to evacuate casualties at will, West continued.
Command Sgt. Major Gerald Ecker, CSM at the Office of the Army Surgeon General and MEDCOM further explained, "We are not going to be able to evacuate people in the future as aggressively as we did in the past. Our air platforms are going to be much more at risk and we are still going to need that capability on the ground."
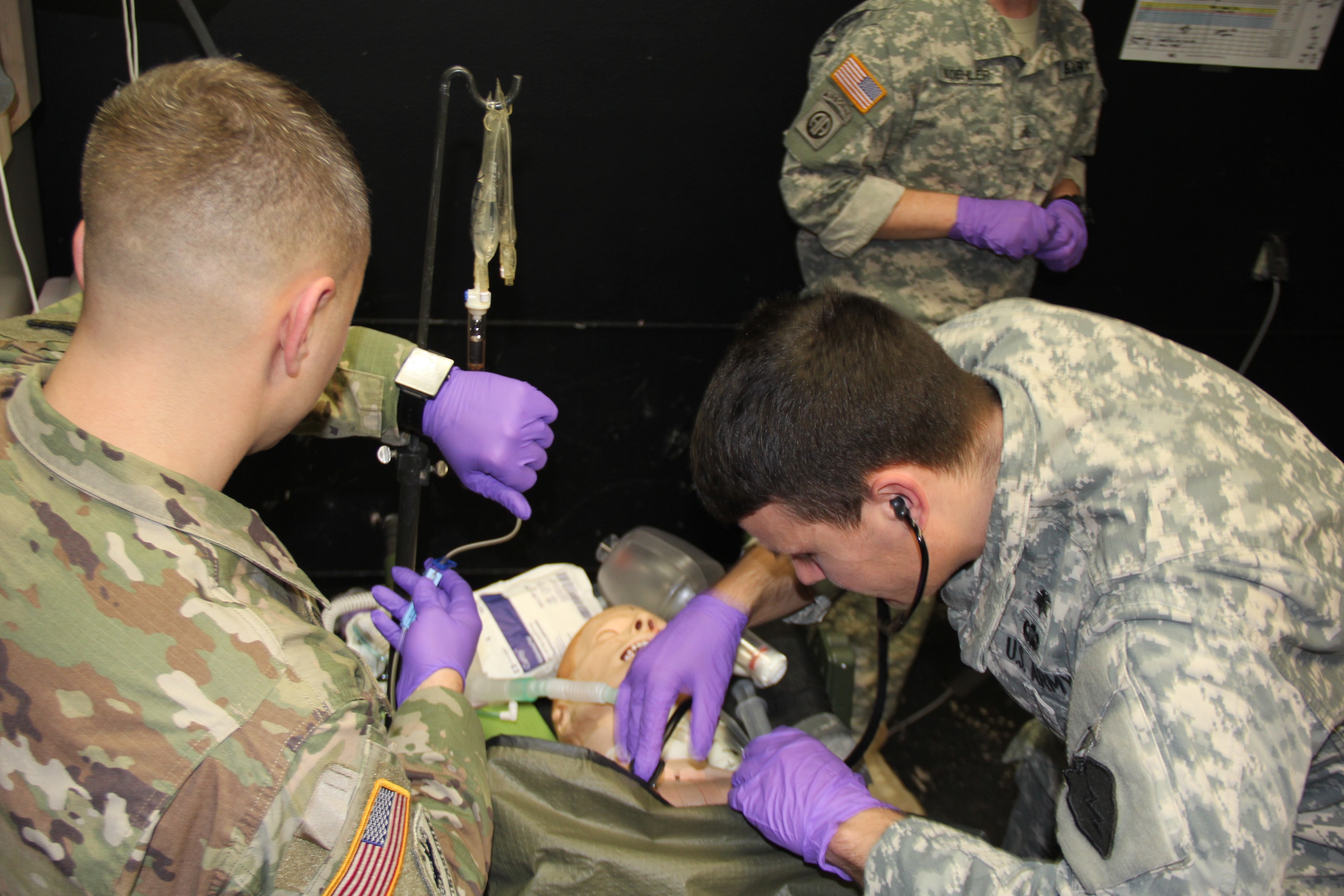
To prepare medics for this eventuality, Popp, working with other MEDDAC-AK medical leaders, designed the five-day course with both classroom and hands-on simulations to educate medics on prolonged care techniques and equipment.
"The course focused on the management of the lethal triad, with emphasis on dilutional coagulophies, hypovolemia and the managing of acid base imbalances," said Sgt. First Class Theodore Kirchmeier, senior clinical noncommissioned officer for MEDDAC-AK and course director.
Popp also used his background in SOF medicine during deployments, along with leveraging the knowledge of nursing principles and practices, and took these lessons learned to help develop the training curriculum and the equipment package for the extended evacuation or prolonged field care environment.
The students were also instructed and provided hands-on training in field blood transfusions, fluid resuscitation, ventilator management, long-term wound care and End-Tital carbon dioxide monitoring.
Many of these lessons were adopted from the Prolonged Field Care Working Group, established by U.S. Special Operations Command, information shared by the Joint Operations Medical Training Center, Fort Bragg, North Carolina.
Popp also uses his background in SOF medicine during deployments to take his lessons learned to help develop the training curriculum and the equipment package
"Regional Health Command-Pacific leaders had the foresight of knowing a gap in the training of our medics existed as well as the potential change to our deployed operational environment, which led to the creation of this course to help mitigate that gap," Popp said.
Popp stated he believes MEDCOM's current leadership is diligently working towards meeting this gap.
"I believe that MEDCOM, along with the surgeon general's emphasis to both enhance the combat medic and work toward providing prolonged field care training, will help close the gap between the SOF medic and the conventional Army medic," Popp said. "This is needed to sustain our current survival rates potentially preventable deaths on the battlefield."
The DECM course is currently being referred up to RHC-P for implementation at regional medical treatment facilities.
Social Sharing