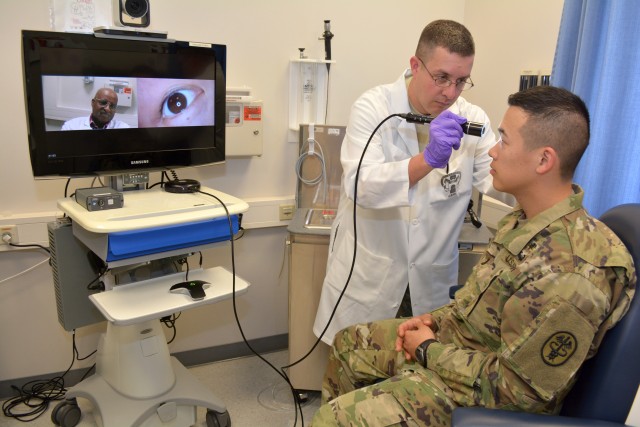
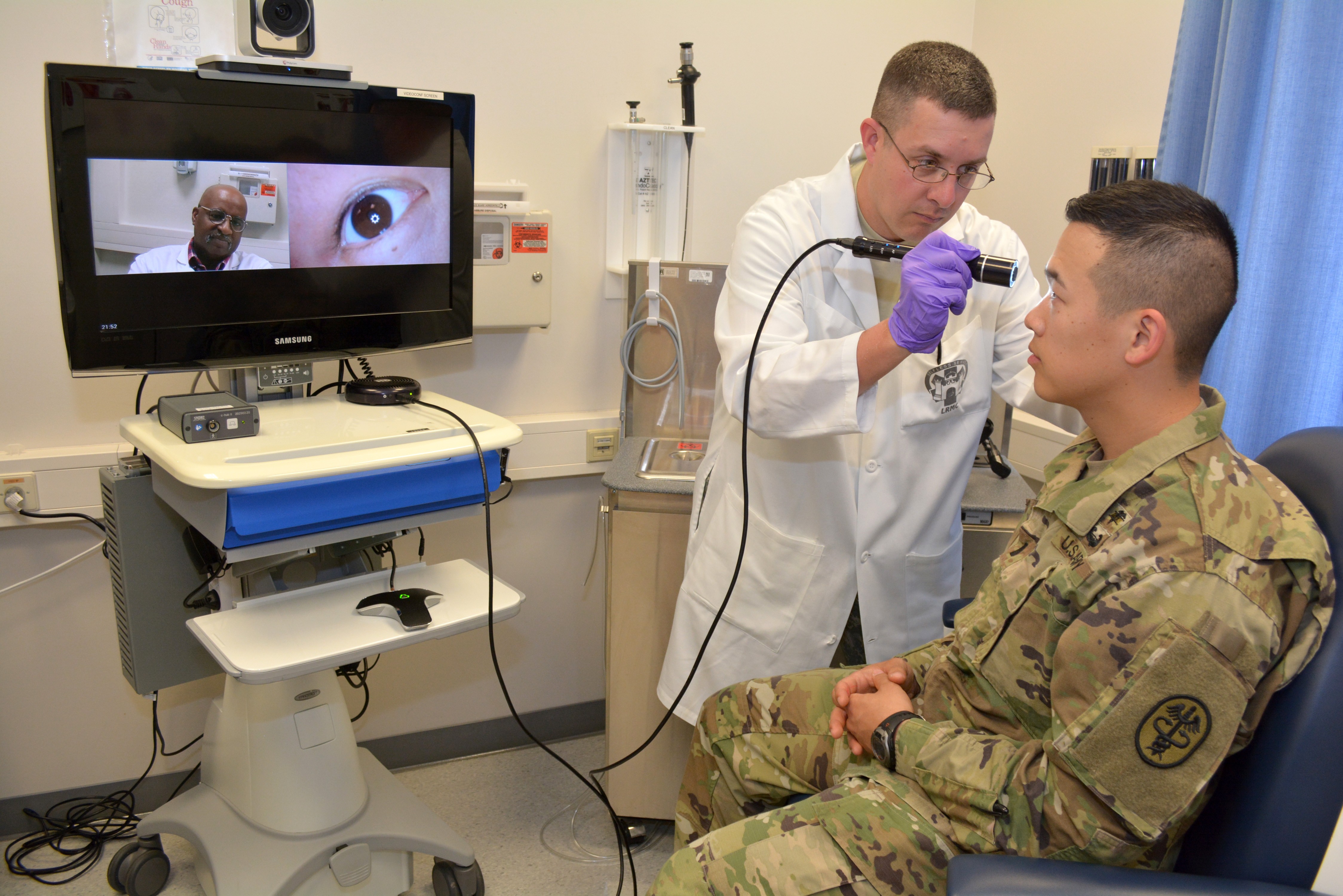
for Regional Health Command Europe, demonstrates the virtual eye exam
capabilities on 1st Lt. Alexander Cho, adjutant for Landstuhl Regional
Medical Center May 31, 2016. Virtua... VIEW ORIGINAL
Editor's Note: This is the first in a three-part series on virtual health. The next article will explain in-home virtual health. The third article will focus on Soldier care through virtual health.
Regional Health Command Europe is responsible for the health care of Soldiers, family members and retirees across Europe. To help ensure health care is available where the customer is, the region has embraced virtual health.
Virtual health is the use of electronic information, imaging, and communication technologies to provide and support health care when distance separates the patient and the provider.
"Virtual health visits are similar to video conferencing applications but with the added benefit of a nurse in the room to help facilitate a robust appointment between the patient and the specialist," said Col. Kirk Waibel, RHCE Virtual Health medical director.
Up until early 2014, virtual health was mainly used for face-to-face encounters with either behavioral health or nutritional health patients, according to Steven Cain, RHCE Virtual Health deputy and surgical physician assistant.
"In 2013, most virtual health visits involved behavioral health and nutritional medicine," Cain said. "At the time we looked hard at existing resources in the Region and sought to provide patients with an expanded care model of virtual health. This expansion included many of the surgical and medical specialty clinics with great success."
In order to help facilitate this expansion, as well as recognizing the barriers and constraints outlying military treatment facilities faced, Landstuhl Regional Medical Center hired, trained, and placed three registered nurses in specific MTFs to support virtual health.
"We quickly realized that it was this dedicated nurse located within the MTF who was the catalyst to help grow virtual health while supporting local providers whose patients required specialty evaluation," said Waibel.
Within 12 months, virtual visits increased 70 percent and more growth is expected as dedicated patient presenters are now located at Vicenza Army Health Clinic, Italy and at SHAPE Army Health Clinic, Belgium.
"Almost every medical and surgical specialty at LRMC is involved with virtual health," said Waibel. "It is exciting to see the growth and interest from health providers at Landstuhl in being a part of virtual health."
Data from the RHCE Virtual Health office shows that in 2014, approximately 1,250 virtual health encounters were conducted. This increased to 2,500 in 2015 and virtual visits in 2016 surpassed 2015 by late summer.
In order to ensure patients receive high quality health care and the provider is able to maintain the same medical standards as a traditional visit, not every patient or diagnosis is a fit for virtual health, Cain said.
"We carefully select patients," he said. "We have standard operating procedures for every service that uses virtual health."
These SOPs outline which diagnoses can utilize virtual health and the procedures for before, during and after the appointment.
"Virtual Health is now part of normal operations in most clinics," Cain continued. "We work very closely with clinics and have excellent leadership support which helps ensure these services endure."
The Region is also ensuring the development of an enduring program by expanding virtual health in other ways.
Recently the RHCE virtual health team coordinated the first in-home virtual health appointment.
In-home virtual health allows patients to connect to their provider from the comfort of their own home through the web camera on their home computer. (Learn more about in-home virtual health in the next part of this series.)
According to Cain, the goal of Virtual Health is to make receiving medical care more convenient for the patient and at the same time maintain high medical and surgical standards which patients expect. A virtual health appointment does not mean a lower standard of care.
"Providers can use telehealth to get a good history, a good review of systems and even some aspects of a physical exam to really understand what is going on with the patient," Cain said. "If needed, they can order more test to be done at the patient's [local MTF]. From there they can send the patient to Landstuhl for additional testing in the morning and meet with them in the afternoon, for example. So providers are able to use the telehealth appointment to facilitate the Landstuhl visit."
Cain went on to say that using telehealth in conjunction with in-person visits creates efficiency for the patient, who may have had to drive to Landstuhl from an outlying area such as Vilseck, Germany.
Along with creating efficiency, there are other benefits to virtual health.
Virtual health increases access to care; leverages specialty providers; links medical resources; eliminates travel costs and optimizes Soldier readiness.
Cain says that while there is some initial skepticism by patients and providers who are new to virtual health, he has seen firsthand virtual health's high quality and a very high level of patient and provider satisfaction. Its benefit is proved even further by the 98 percent patient satisfaction rate the RHCE Virtual Health program has.
"I think what you see now is a mature and robust virtual health system that is still in expansion. The system is a comprehensive care model utilized in many different and exciting ways," Cain said. "Delivery of virtual health services in our region has now become a patient expectation, we continue to work hard to deliver and expand virtual health services in our region."
For more information on virtual health please talk with your health care provider or visit the telehealth home page located at http://rhce.amedd.army.mil/landstuhl/.
Social Sharing